AJCC Prognostic Stage (Breast) Calculator: The Complete Clinician's Guide to 8th Edition Breast Cancer Staging
Breast cancer remains one of the most clinically heterogeneous malignancies, with survival driven not only by tumor size and nodal status but also by hormone receptors, HER2, and tumor grade.
AJCC Prognostic Stage (Breast) Calculator — Free Online Tool
Use the free AJCC 8th Edition Breast Cancer Prognostic Stage Calculator. Enter T, N, M, grade, ER, PR, HER2 to get precise staging in seconds.
Quick Navigation
- 1. Understanding the AJCC 8th Edition Prognostic Stage for Breast Cancer
- 1.1 How Prognostic Staging Modifies Anatomic Stage
- 2. Why the AJCC Prognostic Stage Matters in Practice
- 2.1 Impact on Treatment Planning and Prognosis
- 2.2 The Pain Points Without Digital Support
- 3. Clinical Evidence and Validation
- 3.1 Logic Behind the Staging System
- 3.2 Key Validation Studies Across Populations
- 3.3 Limitations and Considerations
- 4. How the OncoToolkit Calculator Works
- 4.1 Inputs Captured in the Tool
- 4.2 From Input to Output: Mapping to Stage
- 4.3 Usability for Day-to-Day Practice
- 5. How OncoToolkit Supports Clinical Care, Education, and Research
- 5.1 Routine Clinical Decision Support
- 5.2 Education and Simulation for Trainees
- 5.3 Clinical Research and Quality Improvement
- 6. Clinical FAQ
- 7. Integrate Digital Staging Into Your Breast Practice
1. Understanding the AJCC 8th Edition Prognostic Stage for Breast Cancer
Breast cancer remains one of the most clinically heterogeneous malignancies, with survival driven not only by tumor size and nodal status but also by hormone receptors, HER2, and tumor grade. This biological complexity motivated the American Joint Committee on Cancer (AJCC) to overhaul breast cancer staging in its 8th edition, moving from purely anatomic TNM groups to a Prognostic Stage that integrates key biomarkers.[1], [2], [3]
However, the 8th edition defines roughly 170 unique prognostic stage groups, each reflecting a specific combination of T, N, M, grade, ER, PR, and HER2. For breast surgical oncologists and breast surgeons managing full MDT lists, this complexity makes manual staging time‑consuming and error‑prone, especially when juggling multiple cases and evolving pathology reports.[4], [5], [6], [1]
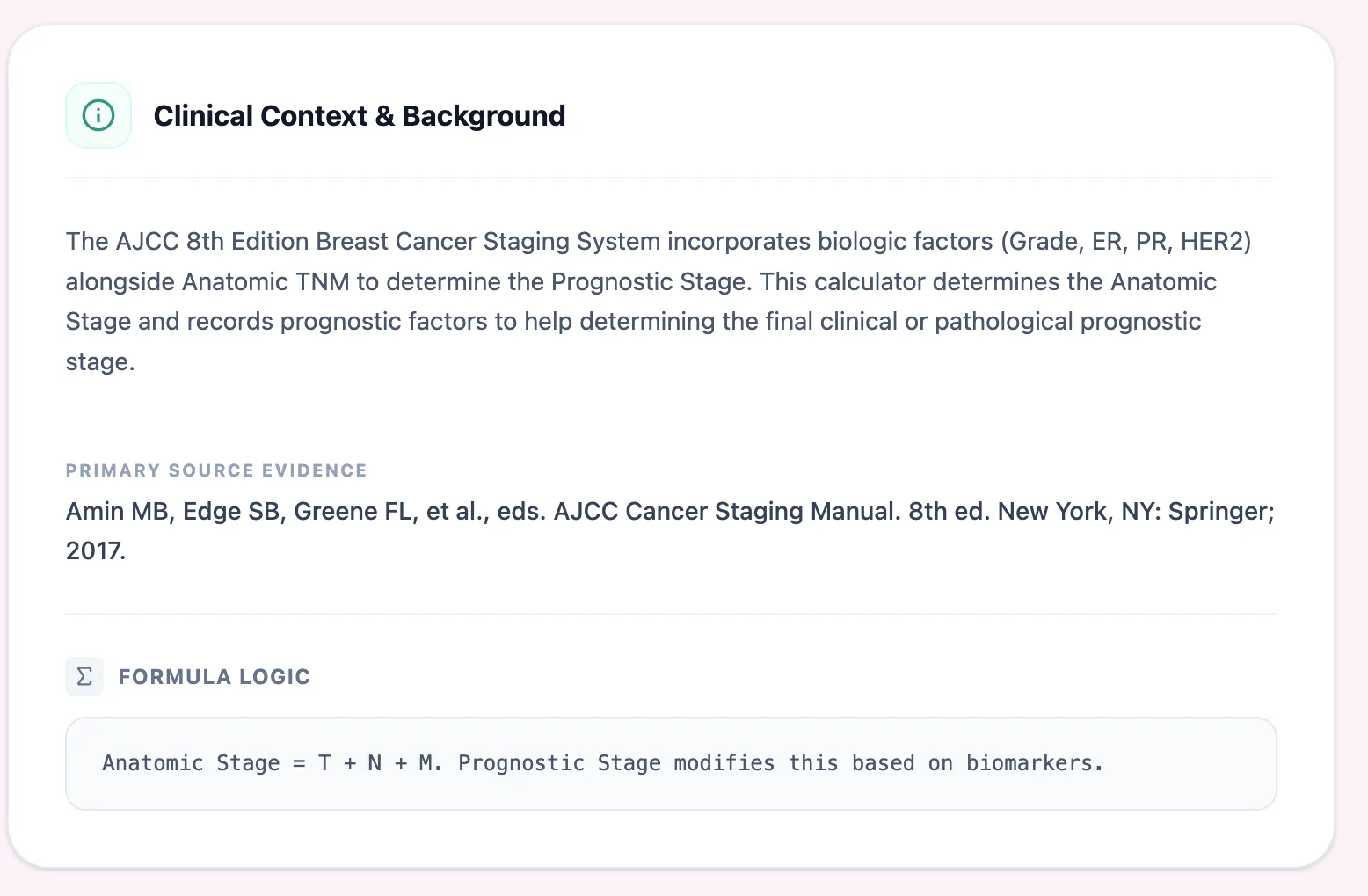
At OncoToolkit, the AJCC Prognostic Stage (Breast) Calculator was designed to offload this complexity. On our platform, this calculator determines the anatomic stage and records the prognostic factors needed to identify the final clinical or pathological prognostic stage—instantly and consistently across the team.[7]

Figure 1. The Clinical Context & Background panel within the OncoToolkit AJCC Breast Cancer Staging calculator summarizes the AJCC 8th Edition framework and cites the primary staging manual, reinforcing transparency and guideline alignment for users.[8]
The AJCC 8th Edition Cancer Staging Manual, released in 2017 and implemented globally from January 1, 2018, represents the most substantial revision of breast cancer staging to date. It introduces two complementary staging concepts:[3], [9]
- Anatomic Stage
- Prognostic Stage
- Integrates anatomic TNM with:
- Histologic grade (Nottingham)
- Estrogen receptor (ER) status
- Progesterone receptor (PR) status
- HER2 status
- Optionally incorporates genomic assays (e.g., Oncotype DX, MammaPrint) in selected ER‑positive, HER2‑negative, node‑negative or limited‑node‑positive cases.[1], [10]
- Integrates anatomic TNM with:
The staging committee concluded that these biologic factors are as prognostically important as extent of disease and must be included for the system to remain clinically relevant. Prognostic staging is now recommended as the primary staging method whenever biomarker data are available.[5], [10], [3], [1]
1.1 How Prognostic Staging Modifies Anatomic Stage
Under the 7th edition, a T2 N1 M0 tumor was uniformly Stage IIB, irrespective of grade or biomarker profile. In the 8th edition, the same T2 N1 M0 tumor may receive very different prognostic stages depending on biology:[6]
- A grade 1, ER‑positive, PR‑positive, HER2‑negative tumor may be downstaged to a lower prognostic group (e.g., Stage IA or IB) to reflect excellent endocrine‑responsive outcomes.[11], [10]
- A grade 3, triple‑negative tumor with the same TNM may be upstaged, recognizing higher relapse risk despite identical anatomy.[12], [3], [1]
Large registry analyses show that more than half of patients are reassigned to a different stage when moving from anatomic to prognostic staging, with substantial downstaging of hormone receptor–positive disease and upstaging of triple‑negative cancers.[11], [6], [12]
2. Why the AJCC Prognostic Stage Matters in Practice
2.1 Impact on Treatment Planning and Prognosis
The 8th edition was built to align staging with modern systemic therapy, where targeted and endocrine treatments markedly alter outcomes for biologically favorable tumors. Key clinical implications include:[3], [1]
- More accurate survival estimates: Validation work shows prognostic staging has a higher concordance index (C‑index) for disease‑specific and overall survival than anatomic staging alone.[13], [14], [6]
- Better risk stratification for adjuvant therapy: Stages now reflect both tumor burden and treatment sensitivity, supporting nuanced conversations about chemotherapy, radiation, and endocrine therapy.[15], [16]
- Improved clinical trial selection: Many trials now specify AJCC 8th edition prognostic stage rather than anatomic stage, particularly in early‑stage hormone receptor–positive disease.[17], [1]
For breast surgeons, this staging framework underpins discussions about breast‑conserving surgery plus radiotherapy versus mastectomy, regional nodal irradiation, and de‑escalation for very low‑risk luminal disease.[4], [15]
2.2 The Pain Points Without Digital Support
Applying the full AJCC 8th edition at the bedside presents several challenges:
- Volume of combinations: Approximately 170 prognostic stage groups exist once all TNM and biomarker permutations are considered.[5], [1]
- Multi‑page tables: The official tables span numerous pages, making quick lookup during MDT meetings or in clinic impractical.[10], [5]
- Cognitive overload: MDT members must synthesize imaging, pathology, and prior treatments while simultaneously recalling complex staging matrices; ethnographic work shows cognitive biases and information gaps often emerge in cancer MDTs under time pressure.[18], [19]
- Risk of misclassification: Population studies reveal that reassigning from anatomic to prognostic staging changes stage in 30–50% of patients; performing this mapping manually increases the chance of error, particularly around intermediate combinations like T2N1 with borderline biologic features.[20], [6], [11]
On our platform, this calculator distills the entire staging matrix into a single, responsive interface optimized for MDT projectors, desktop browsers, and mobile devices. It eliminates table‑hunting and reduces the cognitive load of applying complex rules during real‑time case discussions.[21], [22], [7]
3. Clinical Evidence and Validation
3.1 Logic Behind the Staging System
The AJCC 8th edition breast staging committee used large NCDB datasets, supplemented by external cohorts, to derive stage groupings that cluster patients with similar survival. Key design features include:[1], [3]
- Data foundation: Over 238,000 invasive breast cancer cases with complete biomarker and treatment data were analyzed for 5‑year breast cancer–specific survival, using Kaplan–Meier curves and multivariable modeling.[11], [1]
- Rule‑based grouping: Rather than a single numeric formula, the system uses cross‑tabulated stage groups:
- Determine anatomic stage from T, N, and M.
- Modify this by grade, ER, PR, and HER2 according to survival patterns.
- Optionally incorporate genomic assays (e.g., Oncotype DX) in selected low‑burden luminal disease to refine early stages.[10], [1]
- Biologic rationale: Molecular profiling confirms that higher prognostic stages correlate with enrichment of proliferation and cell‑cycle pathways (e.g., E2F targets, G2M checkpoint), while favorable prognostic groups tend to show more indolent signatures.[23], [3]
This structured but complex rule set is exactly what the OncoToolkit calculator encodes, shielding clinicians from manual cross‑referencing without hiding the logic of the system.
3.2 Key Validation Studies Across Populations
Multiple independent groups have tested the prognostic stage against the older anatomic system:
| Study / Setting | Population | Main Findings | | :-- | :-- | :-- | | Weiss et al. (JAMA Oncol)[11] | 3,327 MD Anderson + 49,767 California Cancer Registry | Prognostic stage C‑index 0.84 vs 0.74 for anatomic stage (P < 0.0001) for disease‑specific survival; major stage migration with better risk discrimination. | | Jin et al. (SEER analysis)[6] | 168,076 SEER patients | 53.2% restaged; 8th edition had superior Akaike Information Criterion (better model fit) and resolved the IIIB vs IIIC paradox. | | Kim et al. (Korean Breast Cancer Society)[24] | 24,014 Asian patients | Pathologic prognostic stage outperformed anatomic staging in predicting breast cancer–specific survival, confirming applicability in East Asian cohorts. | | Wu et al. (Aging)[16] | 24,014 elderly early‑stage patients | Pathologic prognostic staging better stratified survival and informed surgical choices in women ≥65 years, especially regarding breast‑conserving surgery plus RT. | | Li et al. (TNBC)[12], [25] | >12,000 T1‑2N0M0 triple‑negative patients | 57.4% upstaged under 8th edition; prognostic staging provided improved stratification and chemotherapy benefit prediction in TNBC relative to anatomic stage. | | Recent clinical‑trial pooled analysis[13] | Clinical trial cohorts | Prognostic stage improved OS prediction vs anatomic (C‑index 0.721 vs 0.700, p = 0.020) though some intermediate groups (IB vs IIA, IIB vs IIIA) still overlapped. |
Collectively, these studies support the use of prognostic staging as a more discriminating and clinically aligned system across Western and Asian populations, elderly subgroups, and triple‑negative disease.[16], [24], [6]
3.3 Limitations and Considerations
Important caveats to keep in mind when using the AJCC prognostic stage and any calculator based on it:
- Unclassified combinations: Early SEER analyses noted that about 8–9% of patients could not be mapped because their exact biomarker/grade combination lacked a defined group; updates and clarifications from AJCC have reduced but not entirely eliminated these gaps.[6], [10]
- Evolving systemic therapy: As targeted and immunotherapies expand, survival associated with specific stages may change, especially in HER2‑positive and PD‑L1–positive subsets.[13], [15]
- TNBC and high‑risk subsets: In very high‑risk biology (e.g., early‑stage TNBC), the prognostic system may not add substantial granularity beyond recognizing overall poor risk; treatment choices often depend more on chemo‑immunotherapy data than on small stage distinctions.[25], [12]
- Scope of validity: The system is intended for initial staging of invasive breast cancer without prior systemic therapy and should not be applied to DCIS without invasion, recurrent disease, or post‑neoadjuvant settings.[7], [5], [10]
4. How the OncoToolkit Calculator Works
4.1 Inputs Captured in the Tool
At OncoToolkit, this calculator mirrors the AJCC 8th edition requirements while keeping the interface as streamlined as possible. The tool currently collects:[7]
- Tumor size (T): from Tis through T4, with descriptive size brackets.
- Regional lymph nodes (N): including N0, N1, N1mi, N2, N3.
- Metastasis (M): M0 or M1.
- Histologic grade (G1–G3).
- ER status (positive/negative).
- HER2 status (positive/negative).
Oncotype DX and menopausal status are deliberately not included within this calculator, as they are handled in other dedicated breast cancer calculators on the platform (e.g., recurrence‑risk tools).[26], [27]
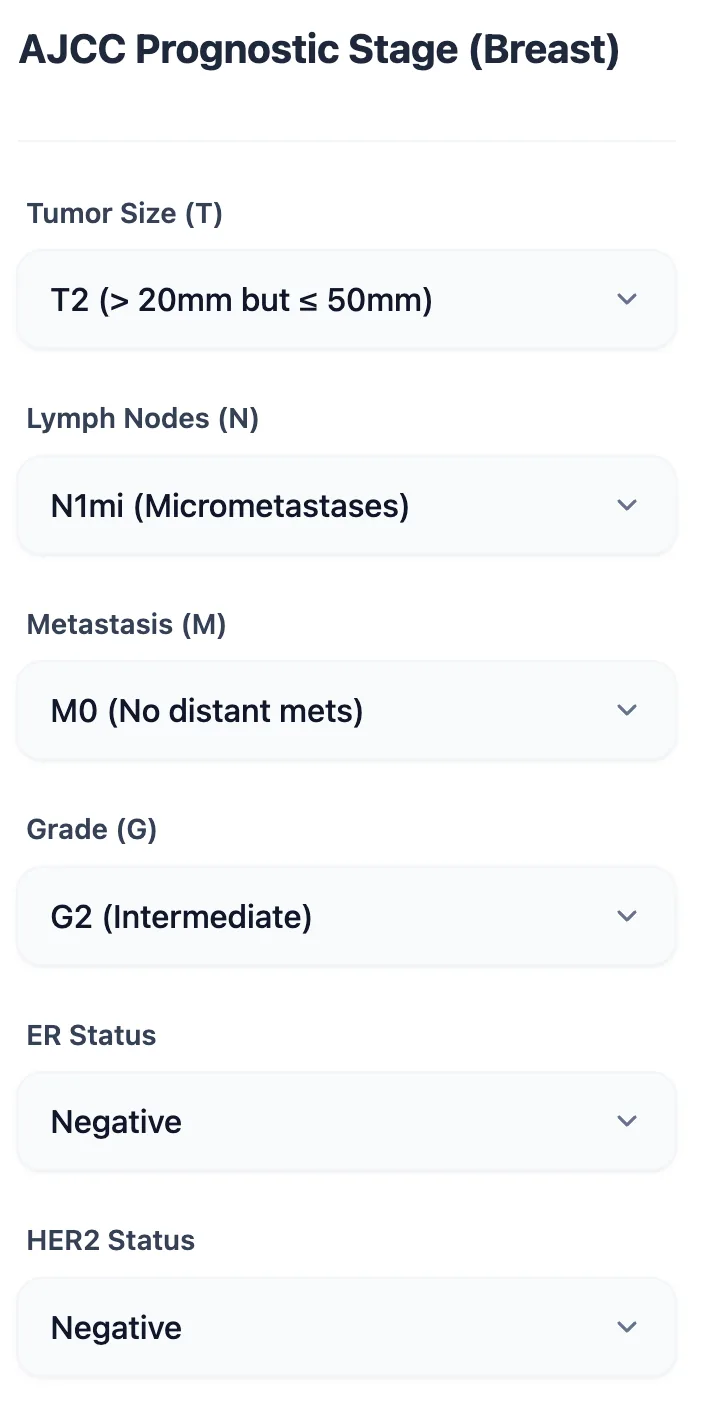
Figure 2. The input interface of the OncoToolkit AJCC Prognostic Stage (Breast) calculator. All required staging variables are captured via labeled dropdowns, optimized for quick, error‑resistant use on both desktop and mobile devices.[28]
4.2 From Input to Output: Mapping to Stage
Once the clinician selects the appropriate values and submits, the algorithm:
- Calculates the anatomic stage by applying standard AJCC TNM grouping rules (Stage 0–IV).[5], [10]
- References an internal staging matrix to identify the corresponding prognostic group for the given T, N, M, grade, ER, PR (assumed per AJCC if not explicitly entered), and HER2 combination, matching the 8th edition definitions.[1], [5]
- Displays the output with:
- Anatomic stage label (e.g., “Stage IIB – Anatomic Stage”).
- Biologic profile summary (e.g., “ER‑negative / HER2‑negative”).
- Visual risk band (low, intermediate, high).
- A note reminding users that the AJCC 8th Edition Prognostic Stage may differ from the anatomic stage, particularly for ER‑positive or triple‑negative disease.[3], [11]
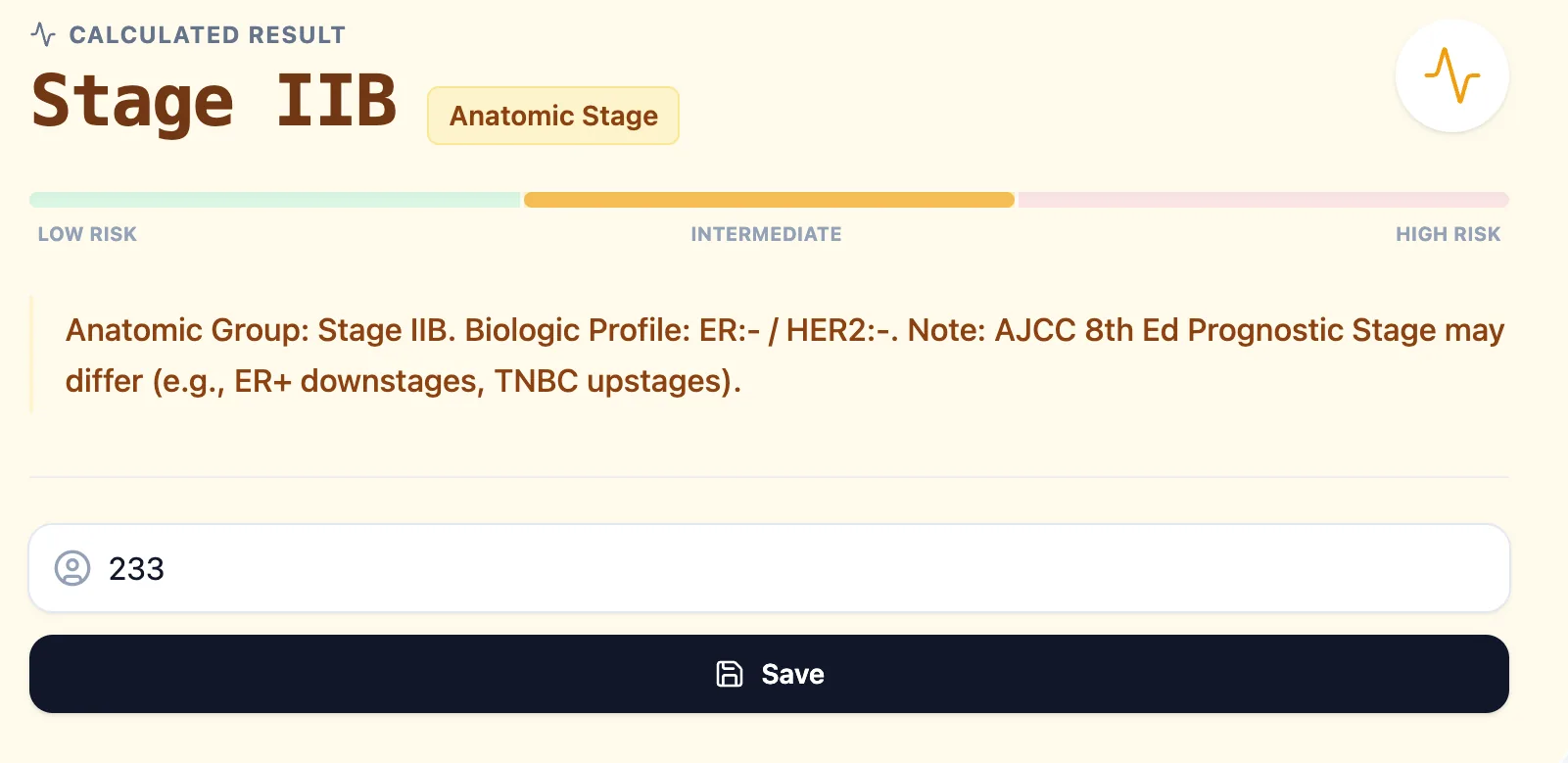
Figure 3. Example calculated result from the OncoToolkit AJCC calculator. The anatomic stage is clearly labeled, the biologic profile is summarized, and a color‑coded bar indicates relative risk, supporting rapid interpretation and teaching discussions.[29]
Alongside the dynamic output, the calculator includes a built‑in reference table mapping anatomic stages to their TNM criteria, which doubles as a quick check for trainees and as a safety net for users verifying borderline T or N categories.[7]
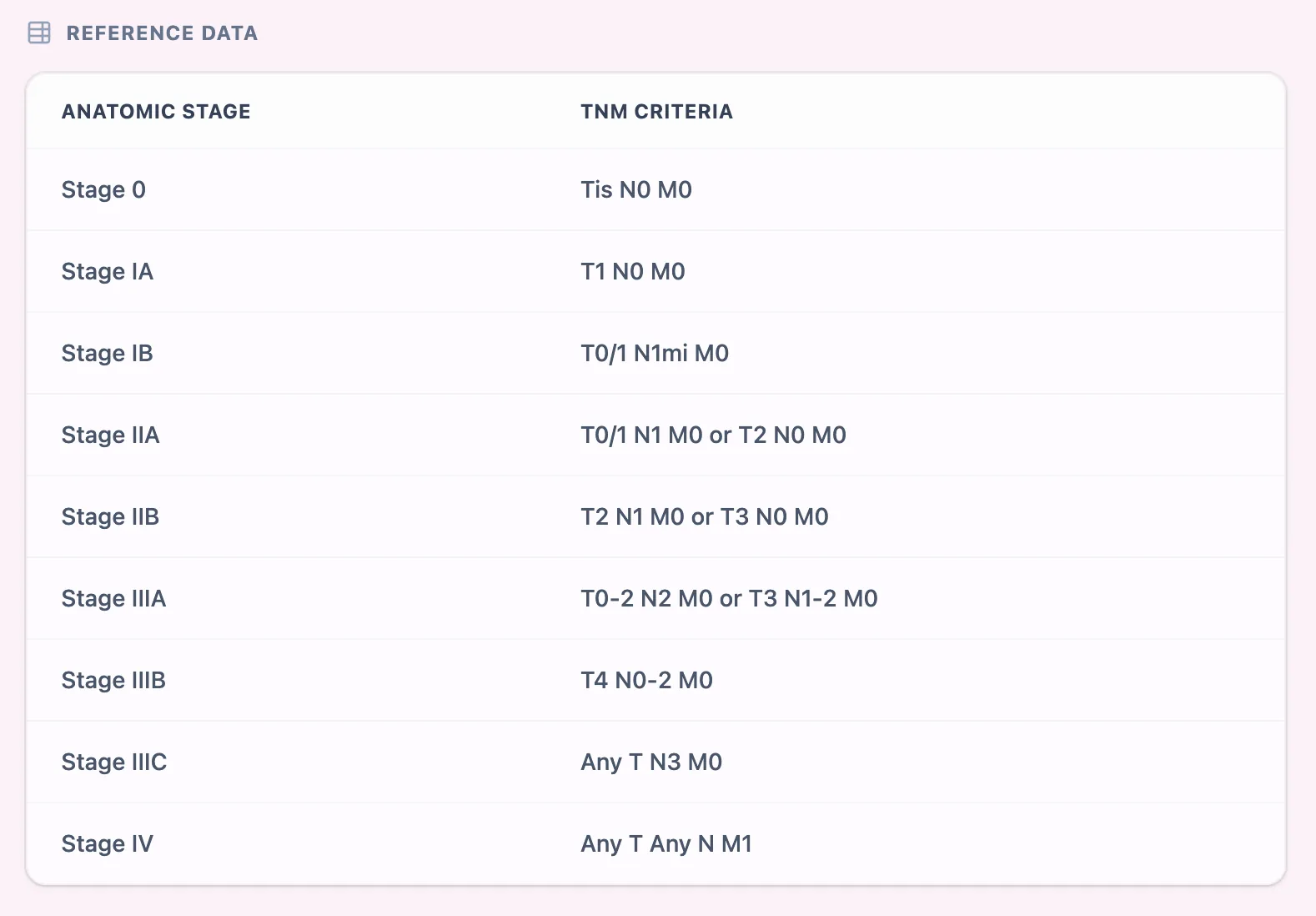
Figure 4. The integrated reference table shows the TNM criteria for each anatomic stage from 0 to IV (e.g., Stage 0 = Tis N0 M0; Stage IIIC = Any T N3 M0), eliminating the need to open separate PDFs or staging manuals mid‑consultation.[30]
4.3 Usability for Day-to-Day Practice
The tool is designed to minimize clicks and reduce staging time to seconds:
- Dropdowns prevent invalid combinations and standardize terminology.
- Mobile responsiveness allows use on smartphones during ward rounds and MDTs.[22], [21]
- A “Save” or export field enables users to store results against a pseudonymized patient identifier, facilitating later review or registry extraction.[7]
5. How OncoToolkit Supports Clinical Care, Education, and Research
5.1 Routine Clinical Decision Support
For breast surgeons and oncologists, the calculator supports:
- Initial staging at diagnosis as soon as definitive pathology is available—without waiting for someone to manually cross‑check tables.[10], [5]
- MDT preparation, where consistent staging across cases helps anchor treatment discussions and reduce variation.[31], [21]
- Treatment selection discussions: combining prognostic stage with recurrence‑risk tools and comorbidity indices helps delineate when to escalate or de‑escalate systemic therapy in early‑stage disease.[15], [16]
On our platform, this calculator sits alongside other breast‑focused tools such as:
- BI‑RADS Score (Breast) for imaging assessment and recall decisions.[32]
- Nottingham Prognostic Index (NPI) for postoperative prognostication.[33]
- MSKCC DCIS Nomogram for in situ disease counseling.[34]
These calculators interlock to cover the full spectrum from screening through definitive surgery and long‑term follow‑up.
5.2 Education and Simulation for Trainees
For fellows, residents, and advanced practice providers, the AJCC calculator doubles as a teaching tool:
- Interactive staging drills: trainees can practice staging real or hypothetical cases and compare their manual answer to the calculator output, reinforcing familiarity with TNM and biomarker impact.[3], [10]
- MDT simulation exercises: educators can project the calculator during teaching MDTs to show how altering ER/HER2 or grade changes the stage for the same anatomic disease, making the concept of “biologic upstaging/downstaging” concrete.[4], [15]
- Reduced cognitive load: decision support tools like MATE and MDT‑focused apps have been shown to improve guideline adherence and confidence in breast cancer MDT decisions, supporting the case for digital staging assistants.[31], [21], [22]
5.3 Clinical Research and Quality Improvement
From a research perspective, using a standardized digital staging tool offers several advantages:
- Consistent application of AJCC rules across large retrospective cohorts, minimizing inter‑observer variability in stage assignment.[24], [6]
- Exportable datasets: on our platform, staging results can be exported and merged with outcomes data to support institutional survival analyses and QI dashboards.[22], [7]
- Stage‑stratified benchmarking: researchers can evaluate whether local outcomes for specific stage‑biology combinations align with published benchmarks from SEER, NCDB, or regional registries.[16], [6]
Clinicians using OncoToolkit can thus move seamlessly from point‑of‑care staging to population‑level analytics without re‑entering data.
6. Clinical FAQ
Can the AJCC Prognostic Stage Be Used After Neoadjuvant Therapy?
No. The AJCC 8th edition prognostic staging is intended for pretreatment staging of invasive breast cancer and specifically excludes patients who have received neoadjuvant chemotherapy, endocrine therapy, or targeted therapy. Post‑neoadjuvant cases should be staged using ypTNM and specialized residual‑disease metrics such as Residual Cancer Burden, which are not captured by this calculator. OncoToolkit’s AJCC calculator should therefore only be applied at initial diagnosis in treatment‑naïve patients.[5], [10]
How Does the AJCC Prognostic Stage Differ from the Nottingham Prognostic Index (NPI)?
The Nottingham Prognostic Index calculates a continuous score based on tumor size, nodal status, and grade to stratify patients into prognostic bands, and has been widely used in surgical series since the 1980s. The AJCC prognostic stage is a categorical system that adds ER, PR, and HER2 to TNM and grade, aligning more closely with current biologic understanding and registry requirements. In practice, many centers use both: AJCC for standardized reporting and NPI for additional prognostic nuance and historical comparisons, and both calculators are available on our platform.[33], [15], [1], [3]
What Is the Most Common Mistake When Applying AJCC 8th Edition Staging?
Common pitfalls include:
- Reporting only the anatomic stage without considering receptor and grade data, effectively reverting to 7th‑edition staging.[11], [3]
- Applying prognostic staging to ineligible patients, such as those post‑neoadjuvant therapy or with pure DCIS.[10], [5]
- Misinterpreting N1mi (micrometastases) or borderline HER2 results, which can shift stage grouping if not classified according to contemporary ASCO/CAP standards.[4], [10]
The OncoToolkit calculator reduces these errors by enforcing complete entry of staging‑critical fields and by clearly labeling outputs and indications.
Is AJCC 8th Edition Prognostic Staging Validated in Asian Populations?
Yes. Large series from the Korean Breast Cancer Society and other Asian institutions show that prognostic staging outperforms anatomic staging in predicting survival, even in populations with different age distributions and subtype frequencies compared with Western cohorts. Some studies also highlight unique age‑ and ethnicity‑related disparities in molecular profiles, underscoring the importance of local validation and ongoing surveillance.[35], [36], [24], [16]
When Should You Avoid Using the OncoToolkit AJCC Prognostic Stage (Breast) Calculator?
On our platform, this calculator is not recommended for:
- Metastatic breast cancer (M1) at initial diagnosis.
- Patients who have already received neoadjuvant systemic therapy.
- Bilateral primary breast cancers (each side requires individualized assessment).
- Pregnancy‑associated breast cancer.
- Pure DCIS without invasive components (use DCIS‑specific tools instead).[34], [5]
- Restaging after recurrence or distant metastasis.
- Non‑primary breast malignancies (e.g., lymphoma, sarcoma, phyllodes tumors).[10]
In all these situations, clinicians should rely on disease‑specific staging frameworks and multidisciplinary judgment rather than this calculator alone.
7. Call to Action: Integrate Digital Staging Into Your Breast Practice
The AJCC 8th Edition Prognostic Stage has redefined how breast cancer is staged, bringing anatomy and biology together into a single framework. Yet its complexity makes manual use challenging in real‑world MDTs and high‑volume clinics.
The AJCC Prognostic Stage (Breast) Calculator on OncoToolkit provides:
- Rapid, guideline‑aligned staging using TNM, grade, ER, and HER2.
- Clear anatomic and prognostic context for treatment decisions.
- Exportable, standardized data to support research and quality improvement.
👉 Open and bookmark the calculator now: /calculator/ajcc-breast-cancer-staging[7]
Next steps for your team:
- Use the calculator for all newly diagnosed invasive breast cancer patients who have not received neoadjuvant therapy.
- Incorporate it into MDT workflows by projecting it during case discussions.
- Pair it with related tools—such as BI‑RADS, NPI, and the MSKCC DCIS Nomogram—for a complete digital decision‑support pathway in breast cancer care.[32], [33], [34]
On our platform, the goal is simple: let the staging logic live inside the calculator, so your attention can stay on the patient in front of you. [37]
Ready to Simplify Your Breast Cancer Staging?
Eliminate manual table lookups and ensure precise 8th Edition prognostic staging in seconds.
Try the Calculator Now
Free to use. No registration required.
References
- Hortobagyi GN, et al. AJCC Cancer Staging Manual: Breast Cancer. Source
- Giuliano AE, et al. Breast Cancer—Major Changes in the AJCC Eighth Edition Cancer Staging Manual. Source
- Amin MB, et al. The Eighth Edition AJCC Cancer Staging Manual. Source
- Doane AS, et al. AJCC 8th Edition: Breast Cancer. Source
- AJCC Breast Cancer Staging System 2018. Source
- Jin MS, et al. Comparison of the 7th and 8th Editions of AJCC Staging. Source
- OncoToolkit AJCC Calculator. Source
- OncoToolkit: Clinical Context Panel. /images/AJCC/AJCC-calculator-clinical-background.webp
- Wang M, et al. Clinical implications of staging. Source
- FACS: Breast 8th Ed Manual. Source
- Weiss A, et al. Validation in MD Anderson Cohort. Source
- Li X, et al. TNBC Validation SEER. Source
- Clinical-trial pooled analysis. Source
- JCO meeting validation. Source
- Gland Surgery: Treatment sensitivity. Source
- Aging: Elderly patients staging. Source
- PMC: Clinical trial selection rules. Source
- BMJ Open: Cognitive load oncology. Source
- PMC: Information gaps MDT. Source
- AACR: Misclassification risk. Source
- JMIR Cancer: Digital interface MDT. Source
- PMC: Mobile responsiveness in clinic. Source
- JCO: Biologic rationale staging. Source
- Kim et al. Korean validation. Source
- Li et al. Surgical choices TNBC. Source
- OncoToolkit Hub. Source
- NCI Breast Risk Tool. Source
- OncoToolkit: Input Interface Image. /images/AJCC/AJCC-calculator-input-data-submission-form.webp
- OncoToolkit: Results Interface Image. /images/AJCC/AJCC-calculated-result-example.webp
- OncoToolkit: Reference Table Image. /images/AJCC/AJCC-calculator-reference-table.webp
- BMJ Open: Decision supportConfidence. Source
- OncoToolkit BI-RADS. Source
- OncoToolkit NPI. Source
- OncoToolkit MSKCC DCIS. Source
- PMC: East Asian validation data. Source
- PMC: Ethnic disparities study. Source
- AACR: Validation prognostic updates. Source