MSKCC (Motzer) Score Calculator for Metastatic Renal Cell Carcinoma
Master metastatic RCC risk stratification with the MSKCC (Motzer) Score. Learn how this 5-factor model predicts survival and guides systemic therapy.

1. Introduction to the MSKCC (Motzer) Score Calculator
Managing metastatic renal cell carcinoma (mRCC) requires integrating performance status, laboratory markers, disease tempo, and rapidly evolving systemic therapy options. Clinicians are often left mentally juggling multiple prognostic variables while simultaneously counseling patients and aligning with guideline‑based treatment pathways. The MSKCC (Motzer) Score calculator on OncoToolkit is designed to offload this cognitive burden by turning a classic five‑factor risk model into a fast, intuitive digital tool that fits naturally into busy mRCC clinics and multidisciplinary team (MDT) meetings.1, 2, 3, 4
The Memorial Sloan Kettering Cancer Center (MSKCC) or Motzer Score is one of the most widely recognized prognostic models in mRCC, historically used to stratify patients into favorable, intermediate, or poor risk based on clinical and biochemical factors. On our platform, this calculator automates the scoring, clearly maps the total number of risk factors to risk group and historical median overall survival, and presents the result in an immediately interpretable visual format tailored to oncologists.2, 4, 5, 1
You can access the calculator here: /calculator/mskcc-rcc.
2. Understanding the Clinical Components of the MSKCC (Motzer) Score
The MSKCC (Motzer) Score is a prognostic model developed to estimate overall survival in patients with metastatic RCC treated with systemic therapy, originally interferon‑alpha. It assigns one point for each of five adverse prognostic factors present at the start of systemic therapy:4, 5
- Karnofsky Performance Status (KPS) less than 80%.5, 2, 4
- Serum lactate dehydrogenase (LDH) greater than 1.5 times the upper limit of normal (ULN).2, 4, 5
- Hemoglobin below the lower limit of normal.4, 5, 2
- Corrected serum calcium above normal (commonly > 10 mg/dL or > 2.5 mmol/L).5, 2, 4
- Time from initial RCC diagnosis to initiation of systemic therapy less than one year.2, 4, 5
The total number of risk factors (0 to 5) is then used to classify patients into three risk groups that correlate with median overall survival. Although originally derived in the cytokine era, the MSKCC model remains a reference standard and is still used in some trials and real‑world practice, particularly as a benchmark alongside more contemporary models such as IMDC.6, 7, 3, 8, 4, 5, 2
On OncoToolkit, we implement the classical five‑factor Motzer model and clearly label it as a prognostic tool for adults with metastatic RCC, intended to complement—not replace—clinical judgment.1, 4, 2
3. Why the MSKCC Score Matters in mRCC Practice
For metastatic RCC oncologists, accurate baseline risk stratification is central to:
- Framing prognosis and shared decision‑making discussions with patients.
- Selecting and sequencing systemic therapies (e.g., IO‑IO, IO‑TKI, or TKI‑TKI regimens) in line with international guidelines that continue to reference MSKCC and/or IMDC risk categories.9, 3, 8, 6
- Designing and interpreting clinical trials, where risk groups influence eligibility, stratification, and subgroup analyses.10, 11, 4, 5
Clinical Pearl: Without digital support, applying the MSKCC criteria often means paging back to tables, checking lab values across multiple EHR screens, and manually tracking counts of risk factors—an easy setup for small errors and “calculator fatigue.”
The OncoToolkit implementation reduces this friction:
- Each risk factor is presented as a clear yes/no question with clinically meaningful labels (e.g., “KPS < 80%?”).12
- The interface is mobile‑responsive and optimized for use at the bedside, in tumor boards, or on shared screens during MDT meetings.1
- Results are displayed visually along a low‑to‑high risk spectrum, immediately reinforcing the patient’s risk group.13
4. Clinical Evidence and Validation of the Motzer Model
4.1 The math behind the tool
The core MSKCC (Motzer) model is intentionally simple: it uses a point‑based approach in which each of the five adverse factors contributes one point to a total score from 0 to 5. There are no weighted coefficients or continuous risk curves; instead, prognosis is driven by the cumulative burden of risk features:4, 5, 2
MSKCC score = sum from i=1 to 5 of (adverse factor_i present ? 1 : 0)
Risk categories are then defined as:
- 0 risk factors: favorable risk.
- 1–2 risk factors: intermediate risk.
- ≥3 risk factors: poor risk.5, 2, 4
OncoToolkit’s calculator simply counts the number of “Yes” responses across the five items and maps the total to the corresponding risk group and historical median overall survival, as originally published.14, 4, 5
4.2 Validation cohorts and outcomes in Western populations
The original Motzer study evaluated 670 patients with mRCC treated with interferon‑alpha, identifying the five factors above as independent predictors of survival and establishing the three‑tier risk classification. In that cohort, median overall survival was approximately:4, 5
- 30 months for favorable‑risk patients.
- 14 months for intermediate‑risk patients.
- 5 months for poor‑risk patients.4
A later validation and extension study from Cleveland Clinic confirmed the model in 353 previously untreated mRCC patients, reporting median survivals around 26 months for favorable, 14.4 months for intermediate, and 7.3 months for poor‑risk groups using closely related criteria. Real‑world registry analyses of patients treated with first‑line sunitinib have also demonstrated that MSKCC risk groups maintain prognostic discrimination for progression‑free and overall survival in Western practice.11, 7, 10
4.3 Validation data and adaptations in Asian populations
Multiple studies have explored how well MSKCC and related models perform in Asian cohorts:
- A Korean multicenter analysis of non‑clear‑cell mRCC showed that both IMDC and MSKCC models reliably predicted first‑line progression‑free survival, total progression‑free survival, and cancer‑specific survival in patients treated with VEGF‑TKIs or mTOR inhibitors.6
- Japanese investigators developed the Japanese Metastatic Renal Cancer (JMRC) classification after noting that MSKCC tended to cluster a disproportionate number of Japanese patients into the intermediate‑risk group. The JMRC system reclassified some intermediate‑risk patients into favorable or poor categories based on additional factors, achieving a more even distribution and better calibration for overall survival in Asian populations.15, 16
4.4 Key limitations and caveats
Thoughtful use of the MSKCC score requires recognizing its boundaries:
- It was derived in pre‑TKI, cytokine‑era populations; absolute survival estimates may not match outcomes with contemporary IO‑based combinations.3, 8, 9, 4
- It is designed for metastatic RCC and should not be applied to localized RCC or non‑RCC kidney tumors.2
- Factors such as comorbidity burden, frailty, and specific metastatic patterns may influence prognosis but are not explicitly captured in the original five‑factor model.17, 18, 11
- Disagreement between MSKCC and other models like IMDC can occur and may signal more complex risk biology.7, 19, 6
5. How Our MSKCC (Motzer) Score Calculator Works
5.1 Step‑by‑step user workflow
On our platform, the MSKCC calculator is structured around a simple, guided interaction:
- Step 1: The clinician is presented with the five prognostic variables as discrete, clearly worded questions (e.g., “Karnofsky Performance Status (KPS) < 80%?”).12
- Step 2: For each item, the user selects “Yes” or “No,” based on the patient’s current clinical status and laboratory data.12
- Step 3: As soon as all fields are completed, the calculator computes the total number of risk factors and assigns the appropriate risk group.13
- Step 4: The result view displays the numeric score, categorical risk group, and corresponding historical median overall survival.14, 13
Figure 1. The input form guides clinicians through each of the five MSKCC prognostic factors.
5.2 Mapping inputs to risk groups and survival
The calculator then surfaces the historically reported median overall survival for that group—30 months (favorable), 14 months (intermediate), and 5 months (poor) in the original Motzer interferon‑treated cohort.14, 1, 4

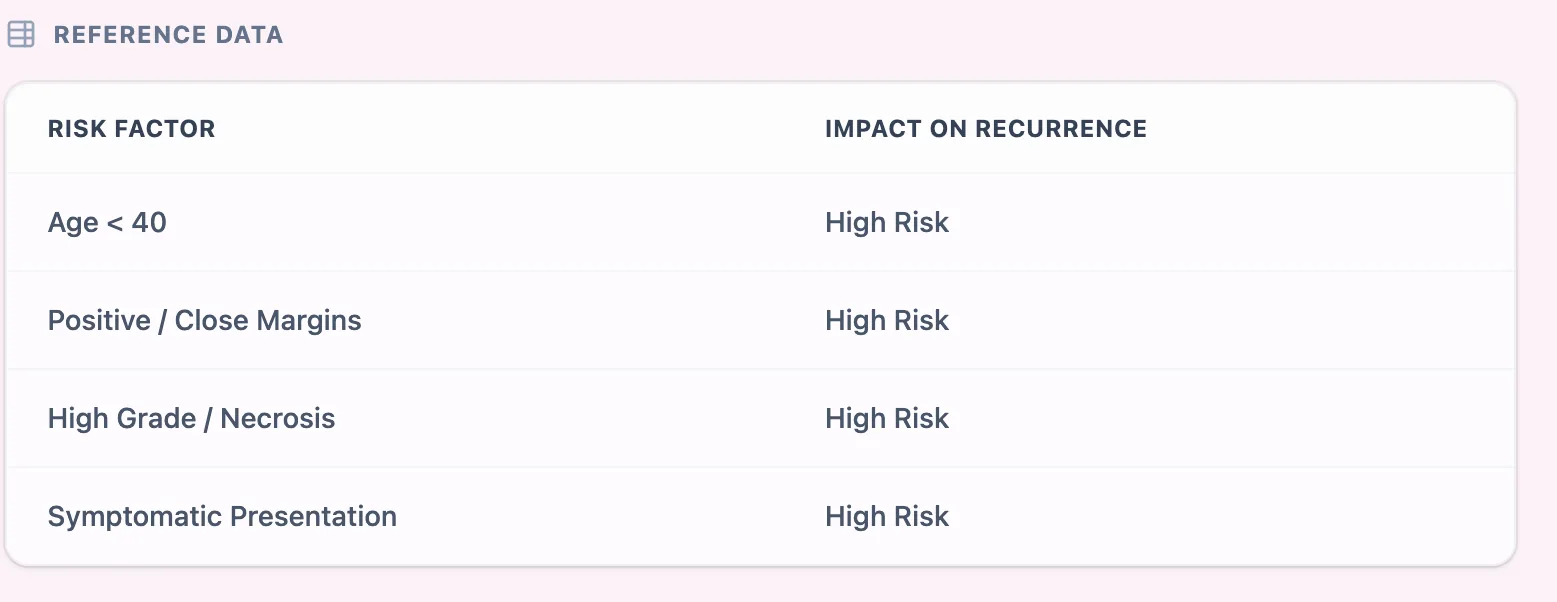
Figure 2. The embedded reference table links the number of adverse factors to risk group.

Figure 3. The calculated result screen highlights the total MSKCC score and risk group.
6. Specific Clinical Use Cases for the OncoToolkit Platform
The MSKCC calculator can be embedded into several practical workflows:1
- First‑line treatment planning: Before initiating IO‑TKI or IO‑IO therapy, clinicians can calculate risk and use it to contextualize survival expectations.8, 9, 3, 6
- Cytoreductive nephrectomy discussions: Poor‑risk patients are less likely to benefit from immediate nephrectomy; using the calculator prior to MDT can help frame this decision.3
- Clinical‑trial screening: Many mRCC trials specify eligibility by MSKCC risk; storing calculator outputs within OncoToolkit can streamline trial enrollment.10, 9, 8
7. Guideline Context and Latest Advances
International guidelines and contemporary reviews continue to recognize both MSKCC and IMDC models:
- EAU guidance: States that MSKCC and IMDC risk groups are “prevalently used” prognostic tools and influence decisions such as immediate versus deferred cytoreductive nephrectomy.3
- Recent overviews: Emphasize that while IMDC has become the preferred model in the targeted era, MSKCC remains an important historical benchmark.9, 8, 3
8. Expansions, Modifications, and Updates to the Original MSKCC System
- Cleveland Clinic extension: Validated the MSKCC model and proposed an expanded system incorporating additional factors such as the number of metastatic sites.11, 7, 17
- Japanese (JMRC) classification: Improves calibration in Asian cohorts where intermediate‑risk patients were over‑represented under MSKCC.15, 16
- Integration with IMDC: Comparative studies show that IMDC may better reflect outcomes with VEGF‑TKIs and IO‑based therapy.8, 6, 9
9. How OncoToolkit Supports Clinical Care, Education, and Research
9.1 Routine clinical decision support
In day‑to‑day mRCC practice, the MSKCC calculator can be incorporated into workflows at diagnosis, treatment selection, and follow-up documentation.8, 5, 4, 6, 9, 10, 3
9.2 Education and simulation for trainees
Our implementation supports teaching by making each risk factor explicit and providing clear mapping to risk groups.2, 5, 4, 13, 14
Figure 4. The clinical background panel supports transparency and educational use.
9.3 Clinical research and quality improvement
Consistent application of prognostic scores is critical when retrospectively stratifying cohorts or designing prospective registries.17, 11, 10, 5, 18, 15, 6
10. Clinical FAQ
When should you not use the MSKCC (Motzer) Score?
The MSKCC score was specifically developed for adults with metastatic RCC and should not be applied to localized RCC, non‑RCC renal tumors, or pediatric cases.11, 18, 9, 5, 2, 4
11. Next Steps: Put the MSKCC Calculator Into Practice
To integrate the MSKCC (Motzer) Score into your workflow, open the calculator at /calculator/mskcc-rcc and bookmark it. Try running a few cases and consider displaying the result live during MDT discussions.14, 13, 1
Ready to Simplify Your mRCC Risk Stratification?
Calculate the MSKCC (Motzer) Score instantly and get immediate clinical context for your patients.
Use the MSKCC Calculator
Free to use. No registration required.
References
- OncoToolkit Official Site. Source
- Pathway Medicine: MSKCC Score for mRCC. Source
- EAU Guidance on Metastatic RCC Surgery. Source
- Motzer et al., J Clin Oncol 2002. Source
- Motzer et al., J Clin Oncol 1999. Source
- Korean Multicenter Analysis of mRCC. Source
- Comparison of Prognostic Models (IMDC vs MSKCC). Source
- Cancer Network: Risk Scoring Systems for mRCC. Source
- Clinical Outcomes and Risk Models in the IO Era. Source
- Clinical Trial Eligibility and Risk Groups. Source
- Cleveland Clinic Validation Study. Source
- OncoToolkit: MSKCC Calculator Input Interface.
- OncoToolkit: MSKCC Results Visualization.
- OncoToolkit: MSKCC Reference Data Mapping.
- JMRC Classification for Asian Cohorts. Source
- Cancer Science: Validation of MSKCC in Japan. Source
- Mekhail et al., Cleveland Clinic Extension. Source
- Limitations of Risk Models in mRCC. Source
- Forbes TIP: Risk Model Comparison. Source
- OncoToolkit: Clinical Background and Documentation.
- IMDC Online Portal. Source