1. Introduction to the MACIS Score (Thyroid) Calculator
Differentiated thyroid cancer usually carries an excellent prognosis, yet long‑term outcomes can vary widely between patients with seemingly similar tumors. For busy endocrinologists and thyroid surgeons, reliably quantifying risk—without juggling multiple tables and formulas during clinic or MDT—is a daily challenge. The MACIS Score (Thyroid) calculator on OncoToolkit is designed to turn this complex prognostic model into a fast, point‑of‑care tool that fits how clinicians actually work.1, 2, 3
At OncoToolkit, we’ve built our MACIS Score (Thyroid) calculator to estimate 20‑year cause‑specific survival for adults with papillary thyroid carcinoma using the original Mayo Clinic model, while minimizing cognitive load and “calculator fatigue.” You can access it directly at: https://oncotoolkit.com/calculator/macis-thyroid-cancer-score.4, 5
2. What is the MACIS Score (Thyroid)?
The MACIS score is a validated prognostic system for differentiated thyroid cancer that incorporates five key variables: distant Metastasis, patient Age, Completeness of resection, local Invasion, and tumor Size. It was developed at the Mayo Clinic from a large cohort of 1,779 patients with papillary thyroid carcinoma treated between 1940 and 1989, with the primary endpoint of 20‑year cause‑specific survival.5, 6
In its original formulation, the MACIS score is calculated as:
- Score = 3.1 if age < 40 years, or 0.08 x age if age ≥ 40 years
-
- 0.3 x tumor size in centimeters
-
- 1 point if the primary tumor is incompletely resected
-
- 1 point if there is local extrathyroidal invasion
The resulting continuous score correlates with long‑term disease‑specific survival and can be grouped into discrete risk categories with distinct 20‑year survival estimates, which our calculator displays visually for easy interpretation.8, 5
Clinical Context: The original MACIS development cohort utilized the core formula above so users can quickly recall what each variable represents and how it contributes to the score.

Figure 1: Clinical context panel summary
3. Why the MACIS Score Matters in Thyroid Cancer Practice
For papillary thyroid cancer, most patients will live decades after diagnosis, but a subset has a substantially higher risk of disease‑specific mortality or recurrence. Prognostic systems like MACIS help thyroid specialists stratify this risk and guide decisions regarding the extent of surgery, radioactive iodine use, and intensity of follow‑up.2, 3, 9, 5
Without a digital tool, the MACIS formula and risk bands require clinicians to repeatedly perform manual arithmetic, cross‑check survival tables, and mentally reconcile MACIS with TNM and ATA risk systems—tasks that are error‑prone when done under time pressure. By contrast, our mobile‑responsive MACIS Score (Thyroid) calculator computes the score and risk group instantly, using a clear risk bar and numerical survival estimate that can be referenced during MDT discussions or bedside counseling.3, 4
3.1 Specific Use Cases for the OncoToolkit MACIS Calculator
The OncoToolkit MACIS Score (Thyroid) calculator is being used in clinical workflows that mirror how prognostic scores are applied in the literature and guideline documents. Typical applications include:4, 2
- Post‑operative risk counseling: After thyroidectomy for papillary or follicular carcinoma, clinicians can communicate an individualized 20‑year disease‑specific survival estimate, which aligns with published MACIS data and helps contextualize the need for adjuvant radioactive iodine.10, 5, 4
- MDT case stratification: Endocrine MDTs often review cases by “low,” “intermediate,” or “high” mortality risk; MACIS, displayed as a continuous score and risk band, provides a quantitative anchor for these discussions.11, 3
- Follow‑up planning: Higher MACIS scores identify patients who may benefit from more intensive surveillance and closer biochemical and structural monitoring, complementing ATA recurrence‑risk categories.12, 2
- Documentation and communication: Incorporating the MACIS value into clinic letters or electronic notes offers a concise, evidence‑based summary of long‑term mortality risk that can be understood across disciplines, including primary care.2, 3
4. Clinical Evidence, Regional Validation, and the Math Behind MACIS
The MACIS score emerged from a Cox proportional hazards analysis of papillary thyroid carcinoma outcomes at the Mayo Clinic, where variables such as age, tumor size, extrathyroidal invasion, resection status, and metastases were evaluated for their independent association with cause‑specific mortality. The final model distilled these into a weighted linear formula, with higher coefficients assigned to more prognostically powerful features like distant metastasis and incomplete resection.9, 5
In the original development cohort, 20‑year cause‑specific survival rates were approximately:
Subsequent studies have extended the use of MACIS to follicular thyroid carcinoma and have compared it with other systems such as AGES, AMES, EORTC, and TNM, often finding MACIS to have the highest proportion of variation in survival explained. In a UCSF follicular thyroid carcinoma cohort, MACIS achieved a PVE of 0.48, outperforming AGES, EORTC, AMES, and TNM as a predictor of survival.10, 3
4.1 Western vs Asian Validation Data
MACIS has been most extensively studied in Western cohorts, where it consistently shows strong discrimination for disease‑specific mortality in both papillary and follicular thyroid carcinoma. In these populations, the classic risk bands and 20‑year survival figures have been repeatedly confirmed, supporting its integration into risk‑stratified management algorithms.3, 10, 5
In Asian populations, several series have evaluated MACIS—often alongside AGES, AMES, and TNM—and have again demonstrated its prognostic utility, although event rates and disease patterns may differ. A Singaporean cohort of 82 patients with follicular thyroid carcinoma found that AGES and MACIS provided the best prognostic information on multivariable analysis, with MACIS emerging as the most accurate system for guiding management. Other regional studies have reported that MACIS retains predictive value but may benefit from recalibration in settings with different age distributions, iodine status, or treatment strategies.13, 11
Pediatric and young‑adult data illustrate further nuance: a multicenter analysis identified a MACIS cut‑off of >4 as predictive of poorer prognosis in children and young adults with differentiated thyroid carcinoma, suggesting that standard adult thresholds may not directly translate to younger populations.14
5. How Our MACIS Score (Thyroid) Calculator Works
On our platform, the MACIS Score (Thyroid) calculator is structured as a streamlined, single‑screen workflow designed for rapid use in clinic or MDT meetings. The interface asks only for the variables strictly required by the original model:
- Age in years
- Tumor size in centimeters
- Completeness of resection (complete vs incomplete)
- Local invasion (yes/no)
- Distant metastasis (yes/no)4, 5
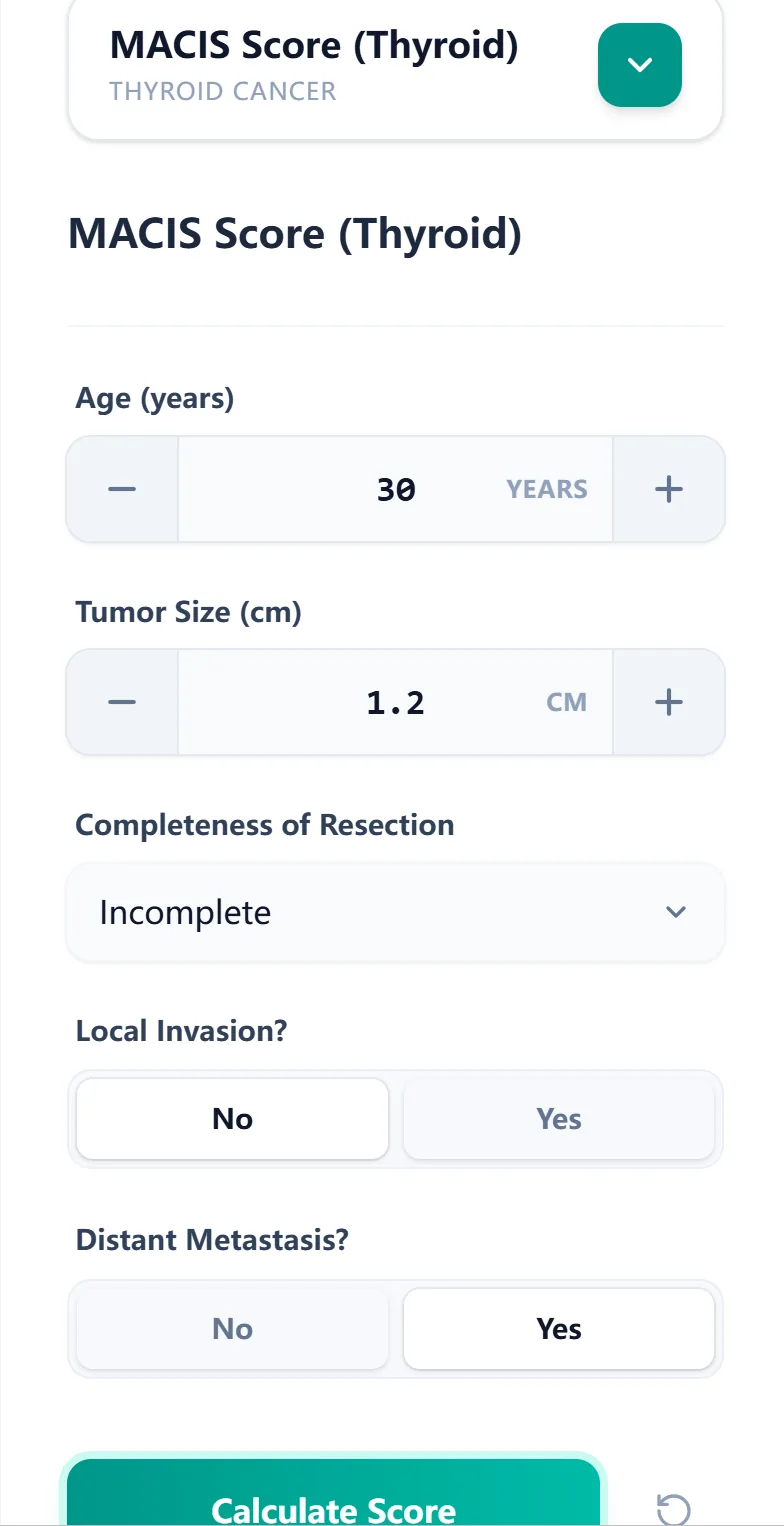
Figure 2: Calculator input form
Once inputs are entered, the calculator executes the MACIS formula exactly as published, applying the appropriate age term (constant 3.1 for patients under 40 or 0.08 x age for those 40 or older), scaling tumor size by 0.3 per centimeter, and adding point increments for incomplete resection, local invasion, and distant metastasis. The final MACIS score is then mapped to:7, 5, 4
- A numeric score to two decimal places
- A qualitative risk band (e.g., low, intermediate, high)
- An estimated 20‑year cause‑specific survival percentage

Figure 3: Reference data mapping
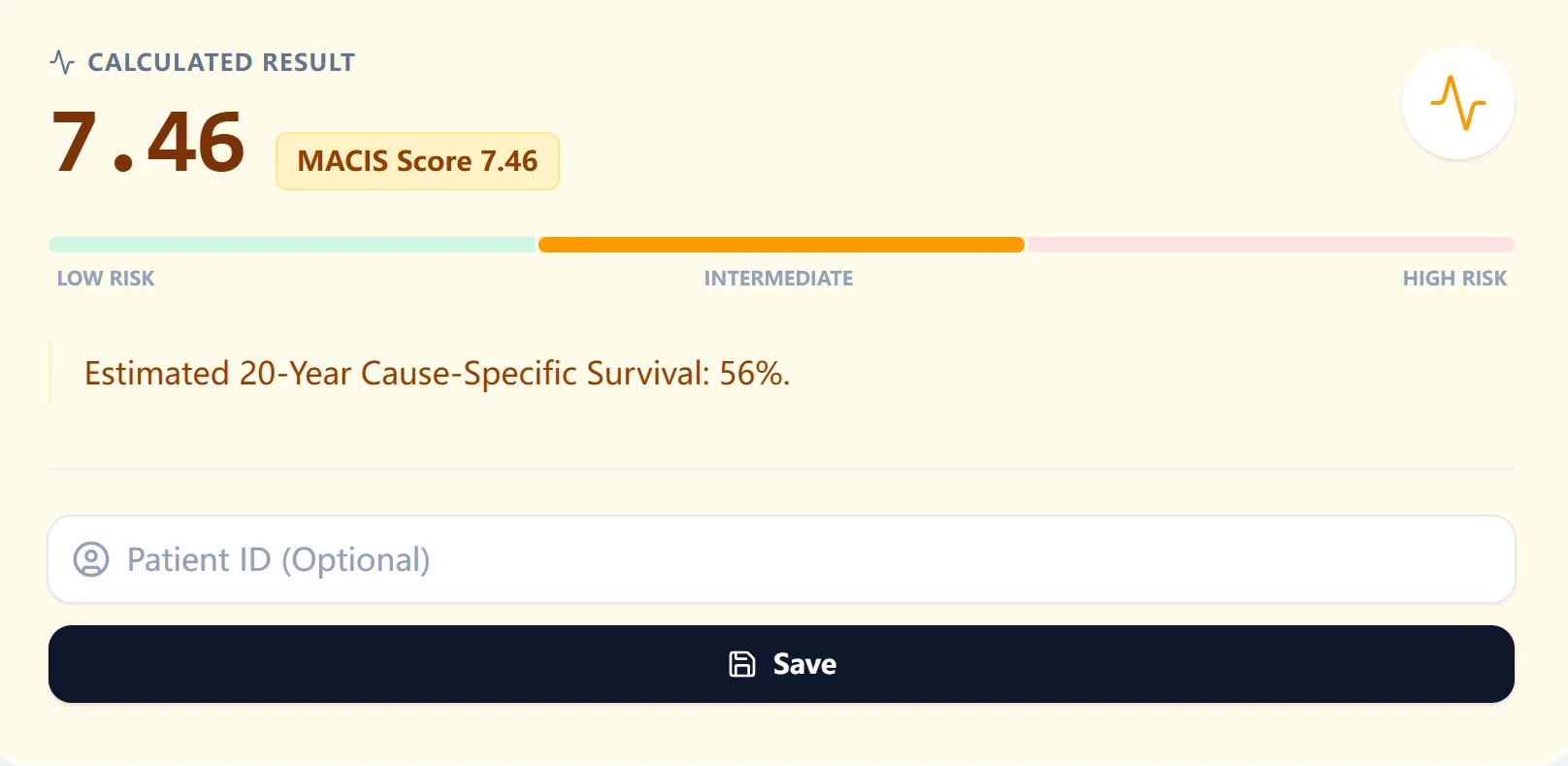
Figure 4: Result screen example
Because the logic is transparent and the reference table is visible on the same page, the tool doubles as a teaching aid, especially for fellows learning how changes in tumor size or resection completeness shift long‑term survival estimates.
6. MACIS in Guidelines and Evolving Evidence
Modern guideline frameworks recognize MACIS as one of several validated prognostic systems for differentiated thyroid carcinoma, though TNM staging and ATA recurrence risk now serve as the primary structuring tools. The 2015 American Thyroid Association (ATA) guidelines reference the original MACIS development paper when discussing prognostic systems that inform risk stratification and long‑term outcome prediction in papillary carcinoma. These guidelines emphasize integrating clinicopathologic risk scores with dynamic response‑to‑therapy assessments over time, rather than relying solely on a single baseline system.15, 2
The AJCC 8th edition thyroid cancer staging system, adopted in calculators endorsed by professional societies, explicitly notes that MACIS is particularly predictive for papillary thyroid carcinoma mortality and complements, rather than duplicates, anatomic staging. NCCN guidelines for thyroid carcinoma similarly encourage multidimensional risk assessment, citing MACIS among prognostic tools that can refine risk estimates in selected patients, especially when considering the intensity of adjuvant therapy and follow‑up.16, 17, 18, 12
6.1 Recent Modifications and Extensions of MACIS
While the core MACIS formula has remained stable, several studies have proposed refinements or new applications:
- Pediatric and young‑adult thresholds: As noted, a MACIS cut‑off >4 has been identified as a marker of poorer prognosis in children and young adults with differentiated thyroid carcinoma, effectively adapting the score for younger cohorts.14
- Follicular carcinoma–specific validation: Work from UCSF and Singapore has confirmed that MACIS retains strong prognostic value in follicular thyroid carcinoma and may outperform other scores, supporting its extension beyond papillary histology.13, 11, 10
- Integration with molecular and genomic signatures: Newer research in intermediate‑risk papillary carcinoma has developed genomic signatures that stratify prognosis beyond what MACIS can capture, with high‑risk genomic groups showing higher MACIS scores but additional predictive power independent of MACIS. These efforts do not replace MACIS but rather build layered models where clinicopathologic scores like MACIS are combined with molecular data.15
- Comparisons with TNM 8th edition: Analyses comparing MACIS to TNM7 and TNM8 have shown that TNM8 downstages many patients yet remains less accurate than MACIS for predicting disease‑specific mortality, reinforcing the value of MACIS as a complementary prognostic tool in contemporary practice.18, 12
OncoToolkit’s implementation stays faithful to the original, well‑validated formula so results can be interpreted against published survival data and guideline discussions, while the platform architecture allows future incorporation of MACIS‑derived or genomically augmented models as evidence evolves.
7. How OncoToolkit Supports Clinical Care, Education, and Research
At OncoToolkit, we’ve designed the MACIS Score (Thyroid) calculator to fit into three high‑value use cases for endocrine teams.
- Routine clinical decision support
- At diagnosis or post‑thyroidectomy, clinicians can calculate MACIS alongside TNM and ATA risk, then use the projected 20‑year survival to frame discussions about adjuvant radioactive iodine, intensity of TSH suppression, and follow‑up intervals.12, 2, 5
- During MDT board reviews, the risk bar and survival percentage provide a shared visual anchor, reducing ambiguity when discussing “higher‑risk” cases and aligning with evidence that MACIS outperforms TNM alone in predicting mortality.18, 12, 3
- Education and simulation for trainees
- Fellows and residents can adjust age, tumor size, or invasion status in the calculator to see how each variable incrementally affects the score and survival estimate, reinforcing a mechanistic understanding of risk that mirrors published hazard relationships.3, 5
- Supervisors can create teaching cases with different combinations of metastasis and completeness of resection, using the calculator’s result display as a starting point for guideline‑based management discussions grounded in ATA and NCCN recommendations.17, 2
- Clinical research and quality improvement
- When used consistently across a clinic’s cases, MACIS provides a standardized numeric index that can be paired with outcomes dashboards to explore associations between risk category, treatment patterns, and long‑term results, echoing approaches taken in comparative staging‑system studies.11, 10, 3
- Our platform’s ability to save or export results (if enabled in your configuration) can support retrospective audits, prospective registries, or QI projects aiming to align care with risk as defined by both MACIS and contemporary guidelines.
From point‑of‑care calculations to aggregated survival analyses, the MACIS Score (Thyroid) calculator is intended as one node in a broader ecosystem of thyroid oncology tools on OncoToolkit. Internal link anchor opportunities include calculators such as a “thyroid nodule risk stratification calculator” and an “AJCC thyroid cancer staging tool,” which together can offer a more complete risk picture for each patient.16, 2
8. When and How to Use the MACIS Score in Practice
In daily endocrine practice, MACIS is most applicable to:
- Adults with papillary thyroid carcinoma who have undergone primary surgery
- Patients where long‑term disease‑specific survival is a key outcome of interest
- Situations where a numeric risk estimate may influence adjuvant treatment or surveillance intensity2, 5
Typical workflow patterns include:
- After histopathology and initial surgery, enter age, tumor size, resection status, invasion, and metastasis into the OncoToolkit calculator.
- Review the MACIS score, risk band, and 20‑year survival percentage alongside TNM and ATA risk stratification, noting that MACIS remains a strong predictor of mortality even in the TNM8 era.12, 18, 3
- Use these data to structure MDT discussions and document risk in letters to referring physicians and patients, while recognizing that dynamic response‑to‑therapy assessments may refine risk over time.2
As always, MACIS is a prognostic framework and not a prescriptive treatment algorithm. Our calculator is a decision support tool that complements, but does not replace, individualized clinical judgment, multidisciplinary review, and shared decision‑making with patients.17, 2
9. Frequently Asked Clinical Questions
Can the MACIS score be used in patients with follicular or poorly differentiated thyroid cancer?
The original MACIS model was developed and validated primarily in adults with papillary thyroid carcinoma, and its best‑supported use remains in that population. Subsequent studies suggest MACIS can also provide useful prognostic information in follicular thyroid carcinoma, sometimes outperforming alternative scoring systems such as AGES, AMES, and TNM, but data are more limited and practice patterns vary. For poorly differentiated or anaplastic tumors, MACIS is generally not appropriate because the biology and outcomes differ markedly from the differentiated cancers on which the score is based.10, 13, 11, 5, 12, 2
How does the MACIS score differ from TNM staging or ATA risk categories?
MACIS is a continuous prognostic score focused on long‑term disease‑specific survival, whereas AJCC TNM staging primarily describes anatomic extent of disease and ATA risk stratification focuses on the likelihood of recurrence. MACIS integrates age, tumor size, extrathyroidal invasion, completeness of resection, and distant metastasis into a single weighted number that correlates with 20‑year survival, offering a more quantitative mortality‑focused estimate than the broader TNM and ATA categories alone. In practice, many endocrine teams use MACIS alongside TNM and ATA to triangulate risk rather than substituting one system for another, a strategy supported by comparative staging‑system analyses.9, 16, 5, 12, 3, 2
What is the most common mistake when calculating the MACIS score?
The most frequent sources of error are misapplying the age term and inaccurately categorizing completeness of resection or local invasion. The formula uses a constant value of 3.1 for patients under 40 and 0.08 x age for those 40 or older, so using 0.08 x age for a 30‑year‑old would overestimate risk. Similarly, confusing microscopic capsular invasion with gross extrathyroidal extension, or labeling a margin “incomplete” when only minimally involved, can shift the MACIS category and its associated survival estimate. OncoToolkit helps mitigate these errors by hard‑coding the age logic and presenting simple yes/no options for invasion and metastasis in the calculator interface.5, 4, 3
Is the MACIS score validated for Western or Asian populations?
The foundational MACIS cohort comes from a Western (North American) tertiary center, and most early validations were similarly Western. More recent studies have evaluated MACIS and related scores in Asian populations, including cohorts with follicular thyroid carcinoma, and have generally confirmed its prognostic utility, though absolute event rates and treatment patterns may differ. When applying MACIS across regions, clinicians should interpret the survival percentages as approximate rather than exact and consider local epidemiology, iodine nutrition, and treatment practices.13, 11, 10, 3, 5
When should you be cautious about using MACIS for decision‑making?
Caution is warranted in pediatric and young adult patients, in whom the relationship between age and outcome may differ and where a lower MACIS threshold (e.g., >4) has been associated with poorer prognosis. Clinicians should also be careful when histology is poorly differentiated, when the resection margin status is uncertain, or when substantial comorbidities may influence overall mortality more than thyroid cancer itself, since MACIS models cause‑specific survival rather than competing risks. In these settings, MACIS can still inform discussions but should not be the sole determinant of therapy.14, 9, 2
10. Call to Action: Integrate MACIS Into Your Thyroid Cancer Workflow
To start using the MACIS Score (Thyroid) calculator in your practice, visit: https://oncotoolkit.com/calculator/macis-thyroid-cancer-score. Embed it into your workflow by bookmarking the page in your clinic browser, adding it to MDT agendas, and encouraging fellows to use it when presenting new thyroid cancer cases.
On our platform, this calculator is built to be quick enough for point‑of‑care use yet transparent enough for education and research—helping you move from individual risk estimates at the bedside to aggregated survival analyses across your patient cohort. Explore our other thyroid tools, such as a thyroid nodule risk stratification calculator and an AJCC thyroid cancer staging tool, to create a unified, digital decision‑support environment for your endocrine oncology practice.16, 11, 10, 3, 2
