NCCN-IPI (Lymphoma) Calculator: A Practical Guide for Oncologists and Hematologists
Diffuse large B-cell lymphoma (DLBCL) remains a biologically and clinically heterogeneous disease. The NCCN-IPI refines the classic IPI to provide accurate baseline prognostication for patients treated with rituximab-based immunochemotherapy.
Quick Navigation
1. Introduction: Prognosticating DLBCL in the Rituximab Era
Diffuse large B-cell lymphoma (DLBCL) remains a biologically and clinically heterogeneous disease, even in the rituximab era. Risk at diagnosis can vary from curable with standard R-CHOP to highly refractory, making accurate baseline prognostication essential for counseling, trial selection, and follow‑up planning. The NCCN International Prognostic Index (NCCN‑IPI) refines the classic IPI and has become an important tool in modern DLBCL management, particularly for patients treated with rituximab-based immunochemotherapy.1, 2
At OncoToolkit, we’ve built a streamlined, mobile‑responsive NCCN‑IPI (Lymphoma) calculator that allows clinicians to obtain a fully interpreted risk category and estimated 5‑year overall survival in seconds, reducing cognitive load and “calculator fatigue” during busy clinics and MDT meetings. You can access it directly at: /calculator/nccn-ipi-lymphoma-prognostic-index.
2. What is the NCCN-IPI (Lymphoma)?
The NCCN‑IPI is a prognostic scoring system developed for patients with DLBCL treated in the rituximab era, using routinely available clinical variables at diagnosis. It retains the core constructs of the original IPI but refines age and LDH, and emphasizes involvement of specific extranodal sites, to better discriminate low- from high‑risk groups.2, 3
The score incorporates five clinical factors:
- • Age in refined brackets (for example, ≤40, 41–60, 61–75, >75 years).
- • Serum LDH level expressed as a ratio to the upper limit of normal (ULN).
- • Involvement of key extranodal sites (bone marrow, CNS, liver/gastrointestinal, or lung).
- • Ann Arbor stage (I–II vs III–IV).
- • ECOG performance status (0–1 vs ≥2).
Each factor contributes a weighted number of points, which are summed to generate a total NCCN‑IPI score ranging from 0 to 8. The score maps into four risk groups with distinct 5‑year overall survival (OS) estimates:4, 5
- Low risk: score 0–1; 5‑year OS around 96%.
- Low‑intermediate risk: score 2–3; 5‑year OS around 82%.
- High‑intermediate risk: score 4–5; 5‑year OS around 64%.
- High risk: score ≥6; 5‑year OS around 33%.
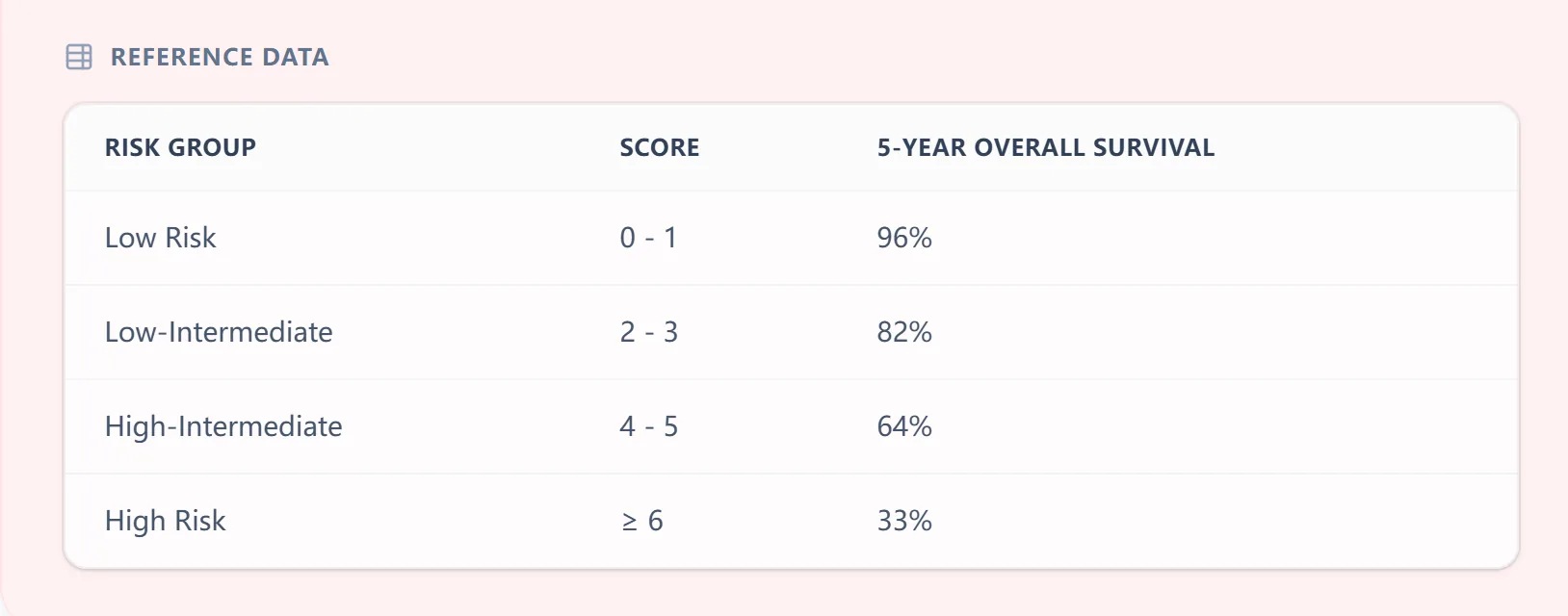
Figure 1. The embedded reference table on our NCCN‑IPI (Lymphoma) calculator shows the four risk groups, corresponding score ranges, and approximate 5‑year OS, providing an at‑a‑glance visual for patient counseling and MDT discussions.
3. Why the NCCN-IPI Matters in Daily Practice
For clinicians managing DLBCL, prognostic indices frame expectations, guide intensity of therapy and surveillance, and help identify candidates for clinical trials or consolidative strategies such as autologous transplant. The NCCN‑IPI has shown improved risk discrimination compared with the original IPI, particularly in separating the very favorable and very poor‑risk ends of the spectrum in rituximab‑treated cohorts.4, 2
Without digital support, applying the NCCN‑IPI requires remembering nuanced age and LDH cut‑offs, specific high‑risk extranodal sites, and translating the total score into four survival‑linked risk categories. In practice, this often leads to:
- Reliance on simplified IPI approximations or rule‑of‑thumb heuristics.
- Time‑consuming checks of PDF tables or guideline appendices.
- Inconsistent risk stratification across clinicians and institutions.
On our platform, the NCCN‑IPI (Lymphoma) calculator removes this friction by:
- Presenting each variable as a clean, structured input (e.g., age range, LDH ratio band, yes/no for high‑risk extranodal sites).
- Automatically summing and mapping to the correct risk group and survival estimate.
- Displaying results in an intuitive visual risk bar that is easy to reference during MDTs, ward rounds, or telehealth visits.
Because the tool is mobile‑responsive, it works equally well on desktop, tablet, and smartphone, allowing rapid point‑of‑care use without flipping through printed scoring tables.
4. Clinical Evidence and Validation
4.1. The logic behind the NCCN-IPI
The NCCN‑IPI was derived using multivariable modeling on large DLBCL datasets from the National Comprehensive Cancer Network (NCCN) and an external population‑based cohort. Investigators started from the original IPI variables and treated age and LDH as continuous covariates in Cox proportional hazards models, then defined clinically meaningful cut‑points to assign integer weights that could be implemented at the bedside.6, 3, 1, 2
In broad terms, the tool applies:
- Increasing point weights with older age brackets (e.g., 61–75 and >75 years carry more adverse weight than ≤60).
- Graduated points for LDH ratio (e.g., 1–3× ULN vs >3× ULN).
- Additional points when specific extranodal organs are involved, reflecting their strong association with inferior survival.
- Single‑point contributions from advanced stage (III/IV) and impaired ECOG performance (≥2).
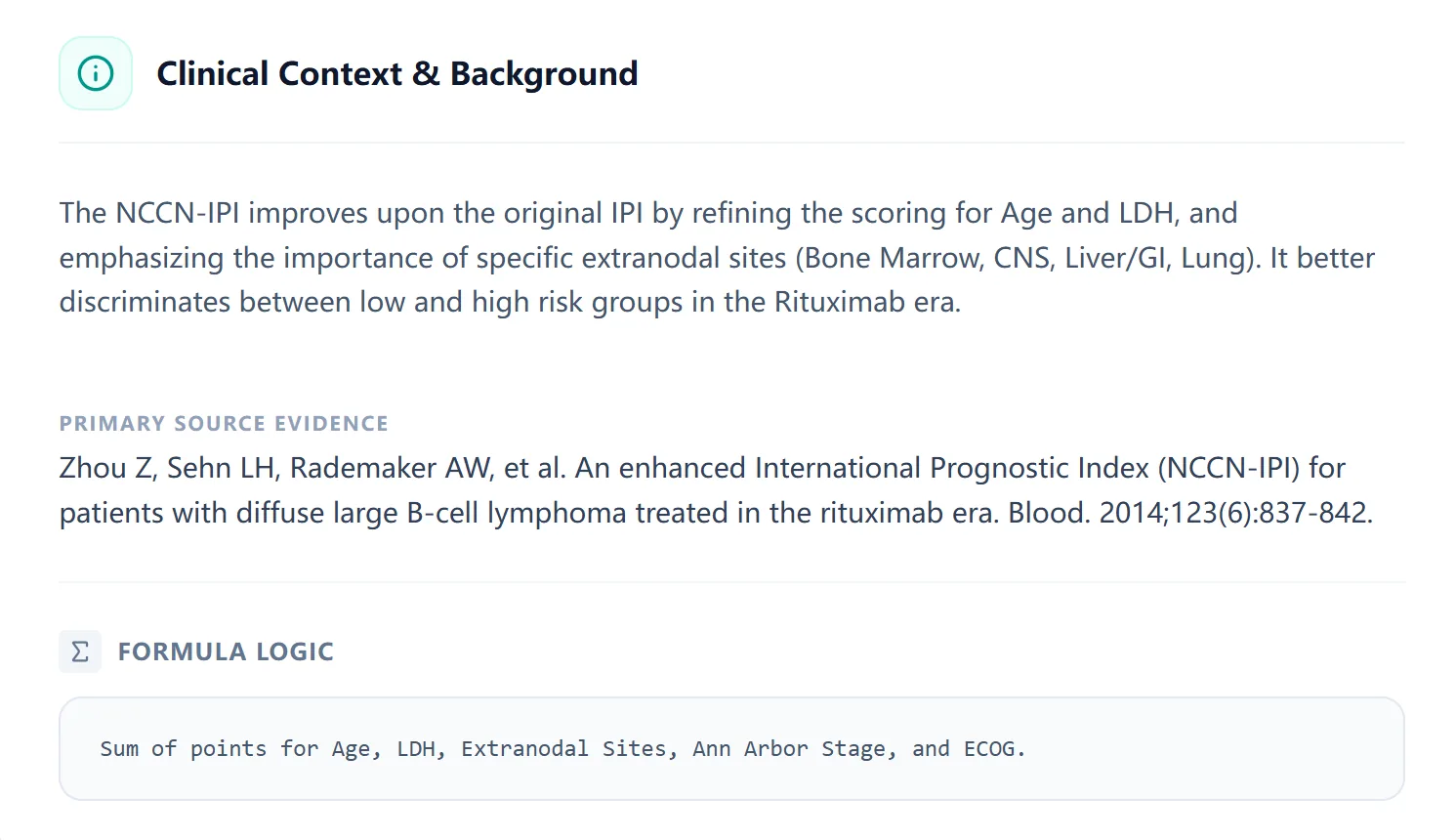
Figure 2. The clinical background panel in our NCCN‑IPI tool summarizes the score’s purpose, derivation, and primary evidence source, ensuring transparent use and easy recall of key concepts for clinicians and trainees.
4.2. Validation and performance
In the original development and validation study, over 1,500 patients with de novo DLBCL treated with rituximab‑based immunochemotherapy were analyzed. Key features include:3, 2
- Endpoints: primarily 5‑year overall survival, with secondary analyses of progression‑free survival.
- Training cohort: NCCN centers; Validation cohort: population‑based British Columbia Cancer Agency registry.
- Four NCCN‑IPI risk groups with 5‑year OS of approximately 96%, 82%, 64%, and 33%, respectively, showing a wider separation between low‑ and high‑risk patients than the standard IPI (90% vs 54%).2, 4
4.3. Limitations and caveats
Thoughtful use of the NCCN‑IPI requires awareness of its boundaries:
- It was developed for newly diagnosed DLBCL in the rituximab era; its application to transformed lymphomas, double‑hit biology, or heavily pretreated disease should be cautious.7, 2
- It does not incorporate molecular features (e.g., cell of origin, double‑expressor status, genetic signatures), which are increasingly relevant for risk stratification and trial design.10, 7
- Estimates of 5‑year OS are population averages and may not fully reflect contemporary outcomes with novel agents or regional differences in supportive care.
Our calculator surfaces these contextual notes in the background panel, and we emphasize that NCCN‑IPI is a decision support tool that complements—but never replaces—individualized clinical judgment.
5. How Our NCCN-IPI Calculator Works
5.1. Step-by-step interaction
On our platform, the NCCN‑IPI (Lymphoma) calculator is designed for rapid, intuitive use by hematologists, medical oncologists, and trainees.
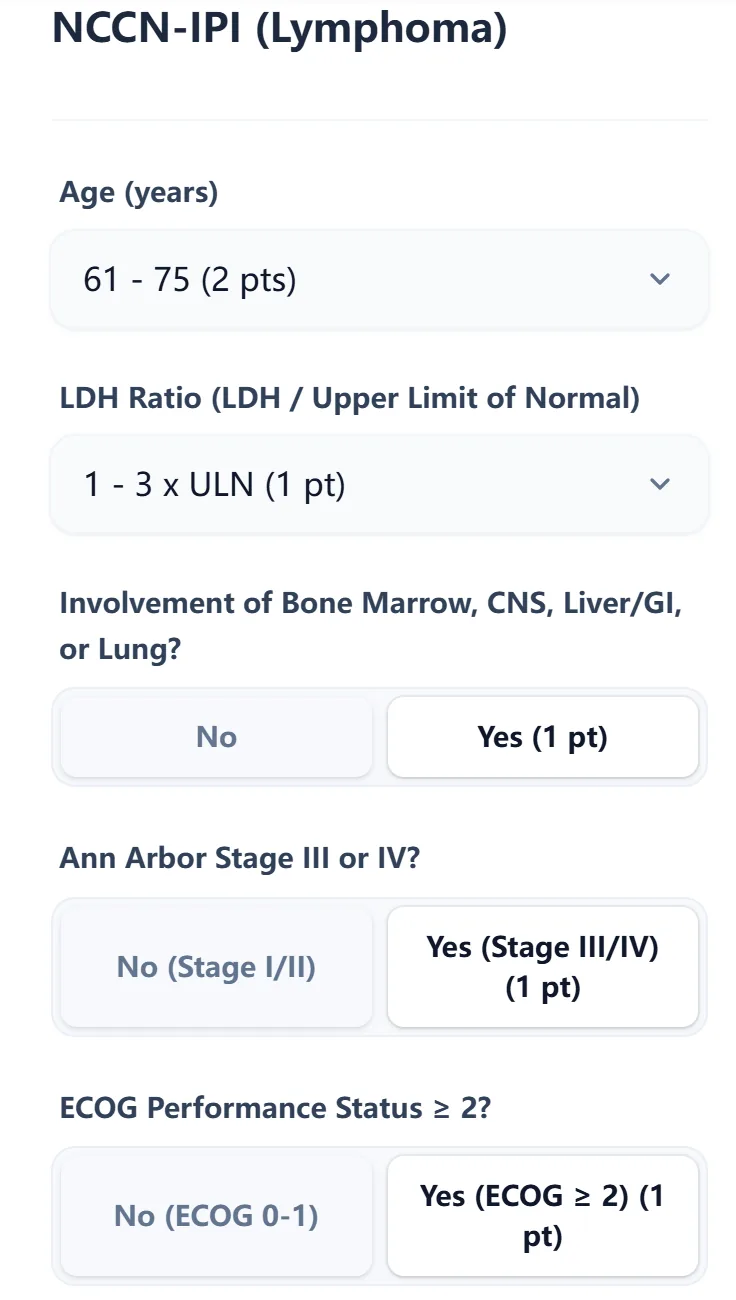
Figure 3. The input form organizes the NCCN‑IPI variables—age bracket, LDH ratio, high‑risk extranodal organ involvement, Ann Arbor stage, and ECOG performance—into a clear, stepwise interface that supports quick, error‑resistant data entry.
The typical workflow is:
- Select age category. Choose the patient’s age bracket (e.g., 61–75 years, which contributes 2 points).
- Enter LDH ratio. Select the LDH band relative to the ULN (e.g., 1–3× ULN, adding 1 point).
- Indicate high‑risk extranodal involvement. Toggle “Yes” if there is involvement of bone marrow, CNS, liver/GI, or lung (1 point).
- Specify Ann Arbor stage. Choose I/II vs III/IV; advanced stage contributes 1 point.
- Record ECOG performance. Select 0–1 vs ≥2; impaired ECOG adds 1 point.
The calculator instantly sums the assigned points to generate the total NCCN‑IPI score. It then:
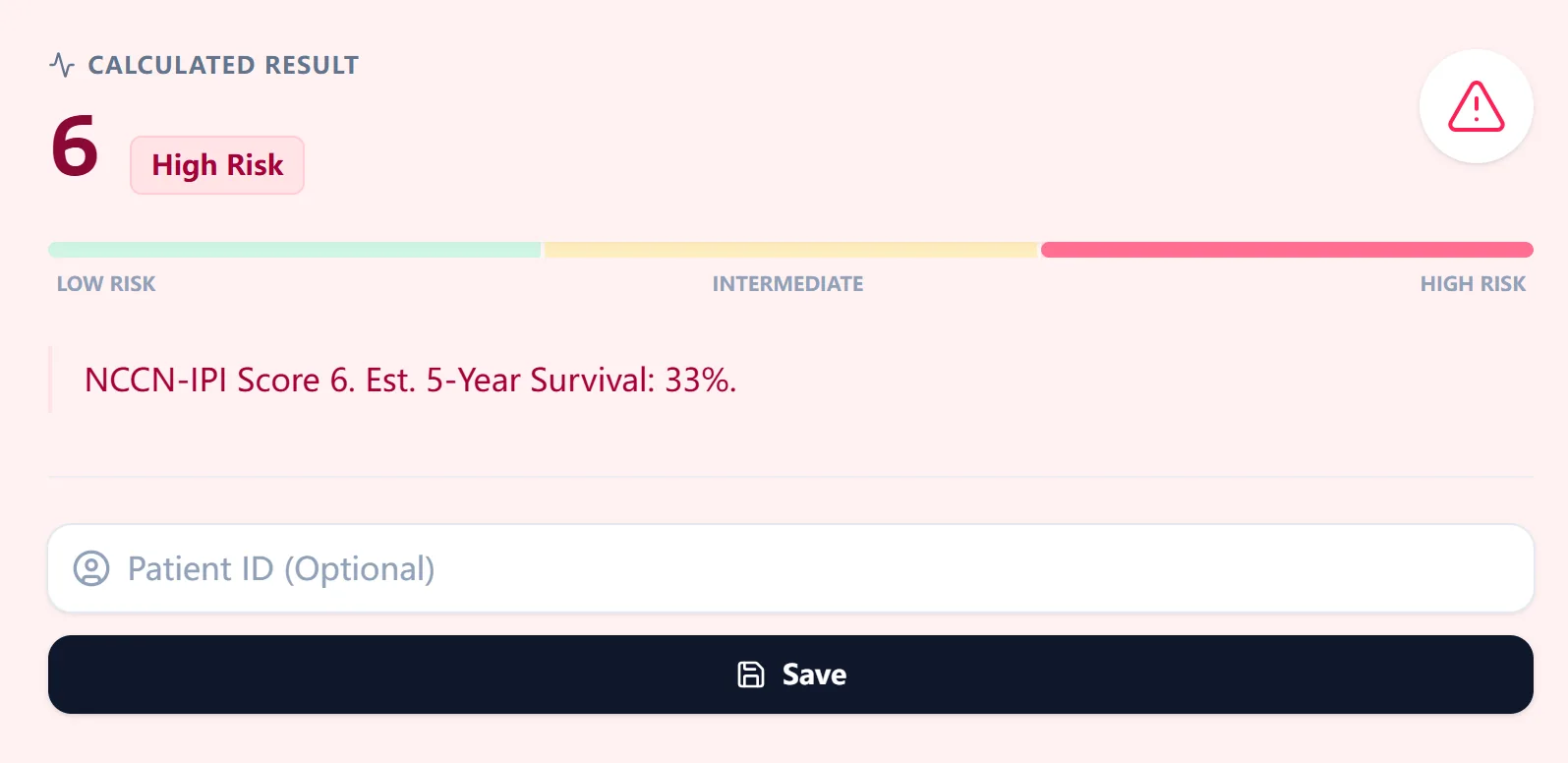
- Places the score on a color‑coded horizontal risk bar spanning low to high risk.
- Labels the corresponding risk group (e.g., “High Risk”).
- Displays the estimated 5‑year OS derived from the original NCCN‑IPI cohorts.

Figure 4. In this example, a total NCCN‑IPI score of 6 maps to the high‑risk group with an estimated 5‑year OS of 33%, visualized on a risk bar and accompanied by a concise interpretive sentence suitable for documentation or patient counseling.
6. How OncoToolkit Supports Clinical Care, Teaching, and Research
6.1. Routine clinical decision support
- Baseline risk assessment at diagnosis, to frame prognosis discussions and tailor follow‑up intensity.
- MDT preparation, providing a standardized risk label and survival estimate for each case discussed.
- Selection and stratification for high‑risk pathways or referral to transplantation or cellular therapy programs, recognizing that many centers use “high‑risk by NCCN‑IPI” as one of several criteria.
6.2. Education and simulation for trainees
- See how changes in age, LDH, or performance status shift patients between risk groups in real time.
- Practice “what‑if” simulations (e.g., comparing a fit 55‑year‑old vs a frail 78‑year‑old with otherwise similar disease).
- Build fluency with the Ann Arbor staging system and ECOG performance scoring.
6.3. Clinical research and quality improvement
- The NCCN‑IPI calculator helps harmonize baseline risk classification across cohorts, reducing variability when comparing survival or relapse patterns over time.
- Saved calculations can be paired with outcomes dashboards or survival curves on the OncoToolkit platform, enabling teams to rapidly explore real‑world outcomes by NCCN‑IPI category.
- Investigators can use NCCN‑IPI as a stratification factor when designing single‑center protocols or observational registries, aligning local work with published evidence.
7. Clinical FAQ
Can the NCCN-IPI be used in lymphomas other than DLBCL?
The NCCN‑IPI was specifically derived and validated in patients with de novo DLBCL treated with rituximab‑based immunochemotherapy. Some studies have explored its use in other aggressive lymphomas—such as peripheral T‑cell lymphoma—not otherwise specified, where it retains some prognostic value, but the predictive performance is generally weaker and should be interpreted cautiously. For non‑DLBCL histologies, disease‑specific indices or trial‑based risk models are usually preferred when available.8, 2, 7
How does the NCCN-IPI differ from the original IPI and R-IPI?
The original IPI assigns 1 point each for age >60, elevated LDH, ECOG ≥2, Ann Arbor III/IV, and >1 extranodal site, producing four risk groups with 5‑year OS of roughly 26–73%. The NCCN‑IPI refines this by using age and LDH as multi‑level variables, focusing on specific high‑risk extranodal organs rather than simply counting sites, and recalibrating risk groups in the rituximab era. As a result, NCCN‑IPI better separates very low‑ and very high‑risk patients compared with the IPI, while R‑IPI (a simplified three‑tier variant) offers easier memorization at the cost of granularity.11, 4, 2, 7
When should you be cautious about using the NCCN-IPI score?
Caution is warranted when:
- The diagnosis is not de novo DLBCL (e.g., transformed indolent lymphoma, primary CNS lymphoma, double‑hit disease).
- Treatment departs significantly from standard R‑CHOP–like regimens, or when novel first‑line combinations and CAR‑T consolidation blur historical outcome benchmarks.9, 7
- Key variables are uncertain or missing (e.g., incomplete staging, uncertain performance status), which can lead to under‑ or overestimation of risk.
What is the most common mistake when calculating the NCCN-IPI manually?
Common pitfalls include misclassifying age into the wrong bracket and using absolute LDH values instead of the ratio to the ULN, both of which can change the score by one or more points. Another frequent error is counting any extranodal disease as high‑risk, whereas NCCN‑IPI specifically highlights bone marrow, CNS, liver/GI, and lung involvement rather than all extranodal sites. By constraining inputs to clearly labeled categories, the OncoToolkit calculator helps prevent these mistakes.5, 1, 4
Is the NCCN-IPI validated in both Western and Asian populations?
The original development and validation cohorts were primarily from North American centers and a Canadian population‑based registry. Since then, several studies from Europe and Asia have evaluated NCCN‑IPI in local DLBCL cohorts, confirming its general prognostic value while noting some regional variation in survival estimates. Clinicians in Asian settings should therefore treat the 5‑year OS percentages as approximate benchmarks.3, 9, 2, 7
8. Call to Action
To incorporate evidence‑based risk stratification into your DLBCL practice, open the NCCN‑IPI (Lymphoma) calculator now at: /calculator/nccn-ipi-lymphoma-prognostic-index. Bookmark it on your clinic workstation and smartphone, and consider making it part of your standard intake workflow for new DLBCL cases and MDT presentations.
We encourage you to test the tool with several example cases, use it as a teaching aid for trainees, and explore other lymphoma‑related calculators on OncoToolkit—such as the classic IPI, age‑adjusted IPI, or treatment‑specific toxicity risk models—using them together to build a coherent, data‑driven approach to prognostication and shared decision making. As always, our calculators are designed to support, not replace, informed clinical judgment tailored to each individual patient.
Ready to Simplify Your NCCN-IPI Risk Assessment?
Access our clinical-grade DLBCL prognostic tool for instant, accurate risk stratification at the point of care.
Open NCCN-IPI Calculator
Free to use. No registration required.
References
- Zhou Z, et al. An enhanced International Prognostic Index (NCCN-IPI) for patients with diffuse large B-cell lymphoma. Source
- Zhou Z, Rademaker A, et al. An enhanced International Prognostic Index (NCCN-IPI) in patients with diffuse large B-cell lymphoma. Source
- NCCN Guidelines. B-Cell Lymphomas. Source
- International prognostic indices in diffuse large B-cell lymphoma. Source
- The Hematologist. NCCN International Prognostic Index. Source
- Zhou et al. Blood 2014 123 837-42. Source
- Clinical relevance of NCCN-IPI in DLBCL cohorts. Source
- Prognostic utility of NCCN-IPI in other histologies. Source
- Regional validation of NCCN-IPI. Source
- Biological signatures and IPI. Source
- JCO. Original and Revised IPI comparisons. Source
- NCCN Evidence Study. Source
- Zhou-Rademaker Enhanced Index. Source
- Clinical Validation Series. Source
- Risk Stratification according to NCCN-IPI. Source