Palliative Prognostic Index (PPI) calculator for pain & palliative oncologists
Use the Palliative Prognostic Index calculator to estimate 3–6 week survival in terminal cancer, support hospice and treatment decisions, and communicate prognosis with confidence. Get transparent, guideline‑aligned results in seconds.

1. Introduction
Prognostication in terminal cancer is central to high‑quality palliative care but remains clinically challenging, especially in the last weeks of life when decisions about hospice, deprescribing, and hospital use must be made quickly. Accurate short‑term survival estimates help align care with patient goals, avoid non‑beneficial interventions, and facilitate timely advance care planning. At OncoToolkit, we’ve built a Palliative Prognostic Index (PPI) calculator to give pain and palliative oncologists a fast, evidence‑based way to estimate 3‑ and 6‑week survival for terminally ill cancer patients, directly at the bedside or in MDT meetings.1, 2, 3, 4, 5
Instead of relying solely on unaided clinician predictions—which are consistently optimistic and variable across physicians—the PPI uses five observable bedside variables to generate a reproducible, point‑based score linked to well‑studied survival thresholds. On our platform, this calculator streamlines data entry into a single, mobile‑responsive view and displays a transparent risk band, reducing “calculator fatigue” and supporting clear communication with patients, families, and the wider team.2, 6, 7
2. What is the Palliative Prognostic Index?
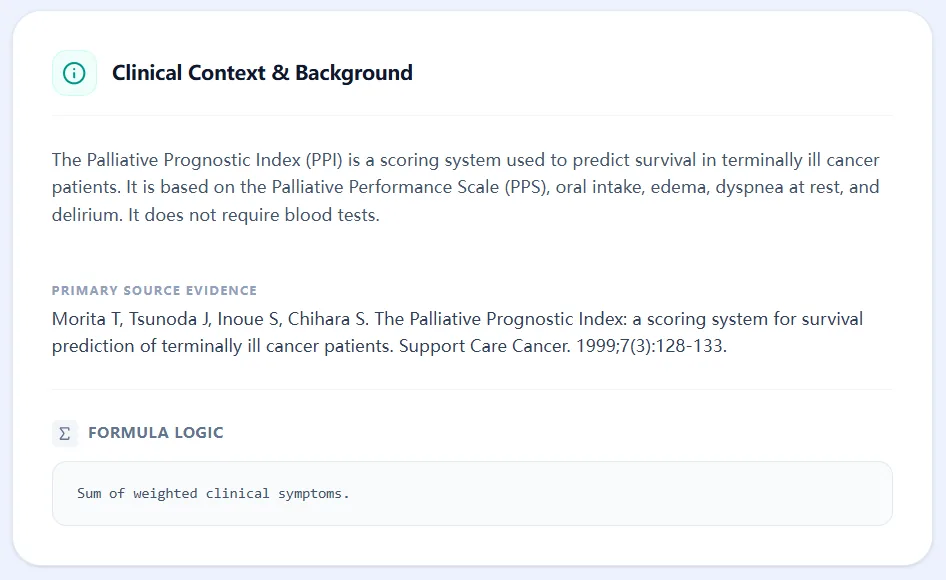
The Palliative Prognostic Index is a bedside scoring system developed by Morita and colleagues in terminally ill cancer patients cared for in Japanese palliative care units. It combines the Palliative Performance Scale (PPS), oral intake, presence of edema, dyspnea at rest, and delirium into a 0–15 point index designed to predict survival over short time horizons (3 and 6 weeks).6, 8, 9, 10
Each component is categorized and weighted according to its independent association with time to death identified in Cox proportional hazards models during the original development study. Scores above 6 indicate a high likelihood of survival less than 3 weeks, while scores 4–6 identify patients at increased risk of death within 6 weeks; scores 0–4 are associated with survival beyond six weeks in many cohorts. Importantly, the PPI requires no laboratory data and can be applied wherever performance status and simple clinical observations can be obtained.11, 12, 4, 6
Historically, the PPI was one of the first purely bedside prognostic indices widely tested in palliative oncology and has since been validated across inpatient palliative units, hospice wards, and home‑hospice programs, making it a familiar tool in many palliative care curricula and reference texts.9, 13, 4
3. Why the PPI score matters in practice
3.1 Clinical decision‑making in the last months of life
The 2023 ESMO Clinical Practice Guideline on prognostic evaluation in advanced cancer emphasizes that structured prognostic models should complement, not replace, clinician judgment when survival is measured in weeks to months. In this framework, the PPI is highlighted as a validated tool specifically developed to predict 3‑ and 6‑week survival in advanced cancer; it is cited as one of several recommended models (alongside PaP and PiPS) for patients with an expected survival of weeks to a few months.14, 2
Accurate short‑term prognostication is clinically relevant for:
- •Hospice referral and setting of care. Hospice and home‑hospice eligibility criteria often reference an expected prognosis of 6 months or less, but many programs use shorter windows (e.g., weeks) to prioritize resources.
- •Decisions about systemic therapy and hospitalization. ESMO guidance recommends against starting or continuing disease‑modifying systemic anticancer therapy when life expectancy is very short.
- •Timing of advance care planning and family meetings. Explicit use of PPI and related tools can trigger earlier advance care planning, resulting in care that matches patient preferences.
3.2 Pain points without digital support
Calculating the PPI manually requires memorizing PPS ranges, multiple cut‑points for oral intake, and the presence or absence of three additional symptoms, plus remembering the survival thresholds for interpretation.4, 10
OncoToolkit’s PPI calculator addresses these pain points by:
Presenting all five variables in one scrollable view.
Encoding scoring weights directly into the interface.
Automatically mapping the total score to color-coded risk bands.
Displaying component‑by‑component logic for transparency.
Clinical Insight: Digital adoption reduces cognitive load and “calculator fatigue,” helping teams adopt the tool consistently rather than abandoning it after the initial training phase.
4. Clinical evidence, validation, and guideline alignment
4.1 The math behind the PPI
The original PPI was derived in terminally ill cancer patients using multivariable Cox regression models with time to death as the outcome. Five independent predictors—PPS, oral intake, edema, dyspnea at rest, and delirium—were identified and converted into integer point weights.6, 11
On our platform, this calculation is implemented as a straightforward additive model. The result screen explicitly lists each variable, its assigned category, and the corresponding partial score, followed by the sum total.
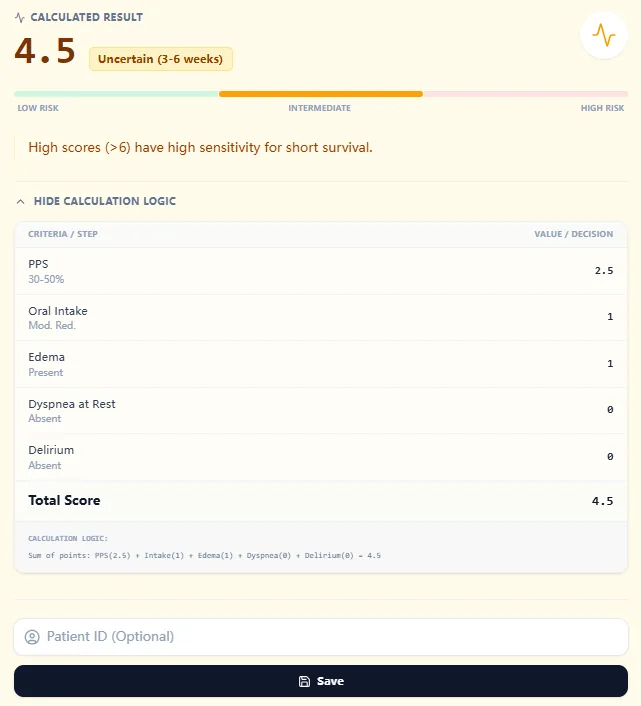
Figure 2. The calculator output displays the total PPI score, mapped risk category (e.g., uncertain 3–6‑week survival), and a full breakdown of component points, supporting transparency, education, and documentation.
4.2 Validation in terminal cancer populations
Multiple prospective and retrospective studies have validated the PPI in advanced cancer:
Original and early validations. Morita’s initial work showed that PPI >6 predicts survival <3 weeks and PPI >4 predicts survival <6 weeks with good sensitivity.16, 7, 6
Systematic reviews and meta-analyses. A 2023 meta-analysis including more than 19,000 advanced cancer patients confirmed these findings.12, 17, 18
4.3 Limitations and caveats
Guideline‑aligned use requires attention to the PPI’s limitations:
Population specificity. The PPI was developed for terminally ill cancer patients; ESMO advises against extrapolating to earlier stages without caution.18, 14, 2
Dependence on clinical assessment. Accurate PPS and delirium assessment is essential; misclassification can significantly alter PPI scores.23, 24
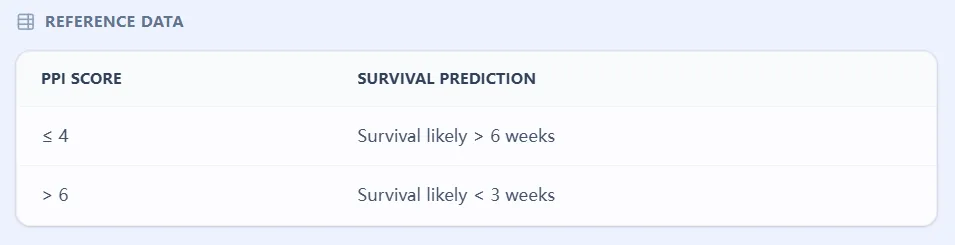
Figure 3. The reference table on OncoToolkit maps total PPI scores to approximate survival categories (e.g., likely >6 weeks vs <3 weeks), consistent with cut-offs used in validation studies and referenced in palliative care guidelines.5, 12, 4
5. Specific use cases and applications in clinical practice
5.1 Hospice referral and level of care
Several hospice and palliative care reference documents recommend structured prognostic tools—including PPI—to support decisions about hospice eligibility and timing.13, 5, 106. How our calculator works
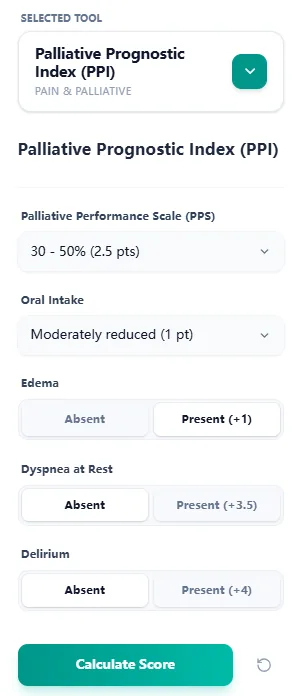
Figure 4. The streamlined input form allows clinicians to capture PPS band, oral intake, edema, dyspnea at rest, and delirium in a few taps, minimizing cognitive load and enabling use at the point of care.
Using the OncoToolkit PPI calculator (/calculator/palliative-prognostic-index-ppi) is straightforward:4
Select PPS band. Choose the PPS range using standard descriptors.
Record oral intake. Select “normal,” “moderately reduced,” or “severely reduced.”
Assess edema, dyspnea, and delirium. Indicate presence or absence based on physical exam.
Calculate score. Click “Calculate Score” to obtain the PPI total and risk band.
7. Recent expansions, modifications, and updates to the PPI
7.1 Simplified Palliative Prognostic Index (sPPI)
To address challenges in reliably diagnosing delirium, a simplified PPI (sPPI) has been proposed, substituting the delirium item with a communication‑capacity question.26, 197.2 Alternative cut‑offs and 21‑day mortality
Some recent studies have explored alternative cut‑offs (e.g., PPI ≥6.5) to optimize short‑term mortality prediction within 21 days.278. Clinical FAQ for the PPI calculator
When should you not use the Palliative Prognostic Index? The PPI should not be used as the sole determinant of treatment or hospice eligibility and is not validated in early‑stage or potentially curable cancer.15, 18, 14, 2
9. Call to action: integrate the PPI into guideline‑aligned care
For palliative oncologists caring for terminally ill cancer patients, the Palliative Prognostic Index offers a pragmatic, guideline‑endorsed way to strengthen prognostic assessment in the last weeks of life. The OncoToolkit PPI calculator at /calculator/palliative-prognostic-index-ppi is built around the original, validated scoring system and cut‑offs recommended in current practice guidance.5, 4, 14
Ready to Simplify Your Prognostic Assessments?
Access the Palliative Prognostic Index calculator and get evidence-based results in seconds.
Use the PPI Calculator
Free to use. No registration required.