Opioid Rotation & OME Calculator: A Practical Tool for Safer Cancer Pain Management
Standardize equianalgesic dosing, apply cross-tolerance reductions, and plan breakthrough regimens with precision using our OME-based clinical tool.
Quick Navigation
- 1. Introduction to Opioid Rotation & OME
- 2. What is the Opioid Rotation & OME Calculator?
- 3. Why OME-Based Opioid Rotation Matters in Practice
- 4. Clinical Evidence and Calculation Logic
- 4.1 The math behind the tool
- 4.2 Cohorts, endpoints, and guideline context
- 4.3 Limitations and caveats
- 5. Understanding the Equianalgesic Reference Table
- 6. How Our Opioid Rotation & OME Calculator Works
- 7. How OncoToolkit Supports Clinical Care, Education, and Research
- 8. Clinical FAQ
1. Introduction to Opioid Rotation & OME
Managing complex cancer pain with strong opioids is clinically demanding, especially when patients develop neurotoxicity, sedation, or inadequate analgesia on their current regimen. Opioid rotation and careful calculation of oral morphine equivalents (OME) are central to modern pain and palliative oncology practice, but performing these conversions safely at the bedside can be error-prone and time-consuming [1], [2].
At OncoToolkit, we’ve built an Opioid Rotation & OME Calculator to streamline this process, standardize equianalgesic dosing, and reduce “calculator fatigue” for busy pain and palliative oncologists. On our platform, this calculator converts a patient’s current opioid to OME, applies evidence-based cross-tolerance reductions, and proposes a starting dose and breakthrough PRN regimen in seconds [3], [4].
2. What is the Opioid Rotation & OME Calculator?
The Opioid Rotation & OME Calculator is a clinical decision support tool that translates a patient’s existing 24‑hour opioid intake into standardized oral morphine equivalents and then suggests a new opioid regimen after adjusting for incomplete cross-tolerance. It is designed for adult oncology patients requiring opioid rotation because of dose-limiting toxicity, uncontrolled pain, or changes in clinical status [2], [4].
Clinical Standard: The tool incorporates widely used equianalgesic conversion factors (e.g., oral oxycodone OME factor 1.5 relative to oral morphine 1.0) and aligns with contemporary guideline concepts for adult cancer pain.
Instead of manually looking up tables or memorizing ratios, clinicians can rely on the calculator to perform the arithmetic consistently and transparently [1], [2].
3. Why OME-Based Opioid Rotation Matters in Practice
Opioid rotation is frequently needed when patients develop intolerable adverse effects (neurotoxicity, myoclonus, sedation, refractory constipation) or when analgesia is inadequate despite escalating doses. Evidence shows that switching opioids while maintaining equianalgesic total daily OME, with an appropriate safety reduction, can improve pain control and tolerability in cancer populations [4], [2].
Performing these steps manually during inpatient rounds or busy outpatient clinics increases cognitive load. On our platform, the Opioid Rotation & OME Calculator is mobile-responsive, so you can quickly compute standardized OME, apply a predefined cross-tolerance reduction, and generate a suggested starting and breakthrough regimen in real time [5], [3].
4. Clinical Evidence and Calculation Logic
4.1 The math behind the tool
At the core of the calculator is a simple, transparent formula:
Adjusted OME = Total Daily Dose × Conversion Factor × (1 - Cross-Tolerance %)
After rotation, the tool also suggests a breakthrough PRN dose defined as a percentage of the daily OME (commonly in the 10–15 percent range), aligning with widely taught palliative care practices for adult cancer pain [2], [4].
4.2 Cohorts, endpoints, and guideline context
Contemporary oncology and palliative care guidelines recommend:
- Standardizing doses to OME to compare and monitor opioid exposure.
- Applying 25–50 percent reductions when rotating between strong opioids due to incomplete cross-tolerance.
- Using short-acting breakthrough doses based on a fraction of the total daily OME [1], [2].
4.3 Limitations and caveats
Like any decision support tool, OME-based calculators have important limitations:
- Methadone:Highly variable pharmacokinetics; usually excluded from simple tables [2].
- Organ Function:Renal and hepatic impairment significantly alter metabolite accumulation [2].
- Variability:Response is influenced by pharmacogenomics and drug interactions.
5. Understanding the Equianalgesic Reference Table
The calculator incorporates a reference table of commonly used strong opioids with their OME conversion factors and brief clinical pearls.
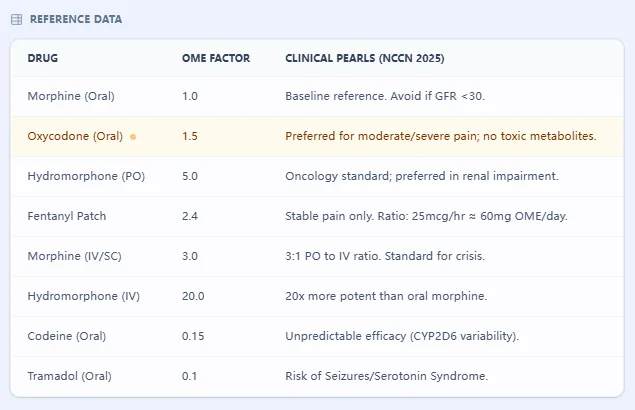
Figure 1. The reference table summarizes common oncology opioids, their OME factors, and clinical pearls such as renal considerations.
6. How Our Opioid Rotation & OME Calculator Works
6.1 Step-by-Step Instructions
- Select the current opioid: Choose the agent from our curated dropdown list [9].
- Enter the total 24‑hour dose: Input the current total daily dose in milligrams.
- Choose the cross-tolerance reduction: Select a default (e.g., 25 percent) or adjust based on clinical frailty.
- Calculate and review: Generate the standardized OME and starting regimen in one click [9], [6].
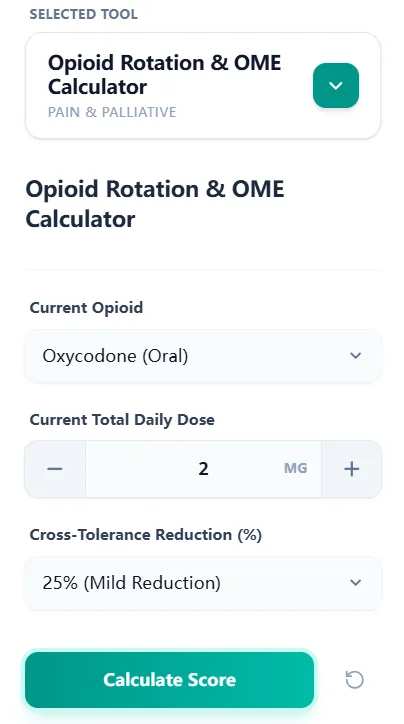
Figure 2. Streamlined input interface designed to minimize clicks and cognitive load.
6.2 Transparent logic and interpretation
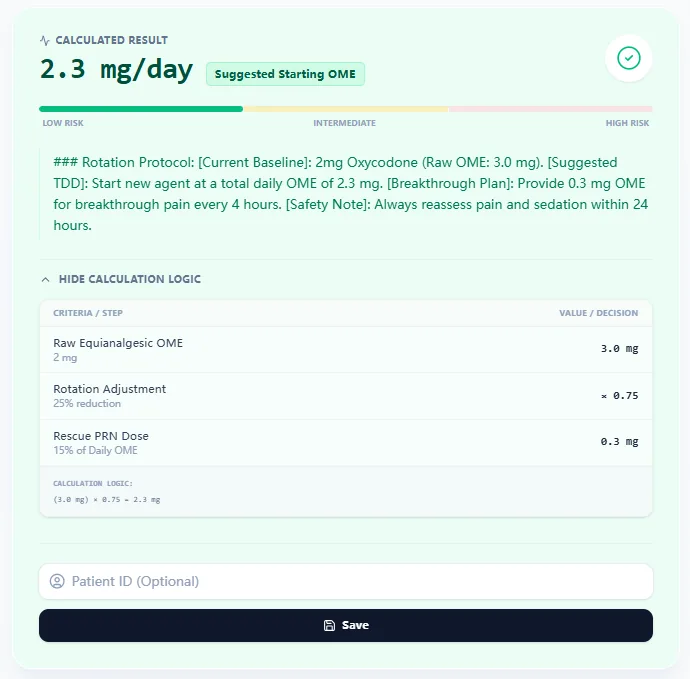
The results panel exposes the intermediate steps: raw OME, rotation adjustment factor, and calculated breakthrough PRN dose [6].

Figure 3. The results pane presents suggested OME and an expandable logic trace for safety verification.
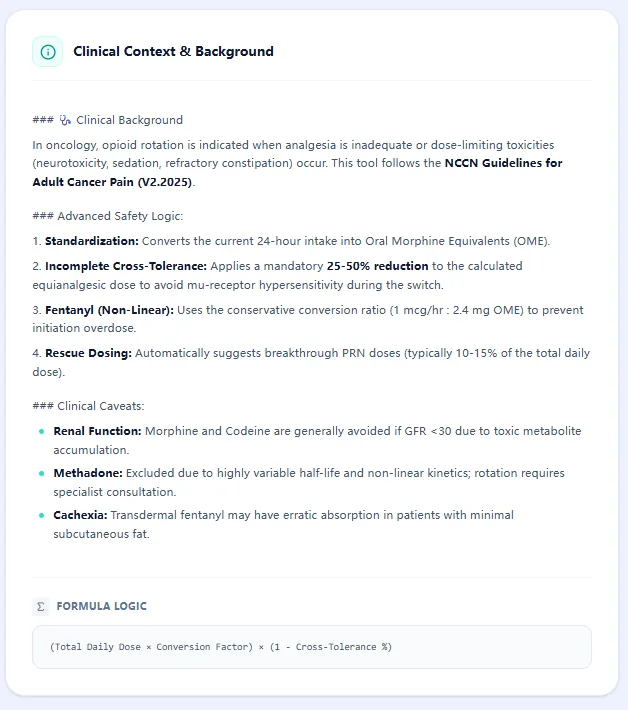
6.3 Clinical background and safety prompts
A dedicated “Clinical Context & Background” section outlines indications, cross-tolerance rationale, and structured safety logic [7], [2].
7. How OncoToolkit Supports Clinical Care, Education, and Research
- Routine Clinical Support: Standardize MDT discussions and ensure case presentations use common OME language [10], [4].
- Education for Trainees: Supervisors can use the calculator as a teaching aid to compare mental estimates with automated logic [7], [8].
- Research & QI: Standardize point-of-care calculations for toxicity studies or survival analyses [3], [2].
8. Clinical FAQ
When should you not use the Opioid Rotation & OME Calculator?
The calculator is not intended for methadone rotation, pediatric dosing, or multi-opioid regimens [2].
References
- 1. Calculator Result Example Reference. Image Source
- 2. Trevino-Villarreal et al. Opioid Rotation in Cancer Pain. PMC9812798. Source
- 3. Clinical Background Data Documentation. Image Source
- 4. Clinical Decision Support Systems in Oncology. JSM Clinical Oncology. Source
- 5. AI and Clinical Decision Support in Oncology. Cancer World. Source
- 6. Reference Table and Arithmetic Logic. Image Source
- 7. Input Data Submission Interface. Image Source
- 8. E-E-A-T and Clinical Content Standards. Source
- 9. EEAT Factors for Medical Web SEO. Source
Ready to Simplify Your Opioid Rotations?
Switch opioids safely and calculate OME instantly with our clinical tool.
Try the OME Calculator Now
Free to use. No registration required.