Mirels Score Calculator: Pathologic Fracture Risk Assessment
Estimate fracture risk in long bone metastases using the Mirels Score. Guide decisions on prophylactic fixation vs. radiotherapy with this evidence-based tool.

Quick Navigation
- 1. Introduction to the Mirels Score Calculator
- 2. What Is the Mirels Score?
- 3. Why the Mirels Score Matters
- 4. Clinical Evidence & Methodology
- 5. Specific Clinical Use Cases
- 6. How the Calculator Works
- 7. Guideline Alignment
- 8. Recent Advances & Alternatives
- 9. Platform Support & Research
- 10. Clinical FAQ
- 11. Integrate Into Your Workflow
- 12. References
1. Introduction to the Mirels Score Calculator
Metastatic involvement of long bones is common in advanced solid tumors and hematologic malignancies, and pathologic fractures in these bones can be catastrophic for patients’ function, pain, and overall quality of life. Deciding when to recommend prophylactic fixation versus radiotherapy or systemic therapy alone is clinically complex and often time‑critical, especially for bone and spine oncologists managing heavy caseloads.1, 2, 3, 4
The Mirels Score is a widely adopted, point‑based system that estimates fracture risk in long‑bone metastases and guides whether prophylactic internal fixation is warranted before radiotherapy. At OncoToolkit, we’ve built a streamlined, mobile‑friendly Mirels Score (Fracture Risk) calculator that translates four key clinical and radiographic variables into an interpretable risk category and treatment suggestion, reducing cognitive load and “calculator fatigue” in everyday practice.5, 6, 7, 1
2. What Is the Mirels Score?
The Mirels Score is a 4‑factor clinical tool designed to predict impending pathologic fracture in long bones affected by metastatic disease. It assigns 1–3 points to each of four domains—pain, lesion site, lesion type, and lesion size (cortical involvement)—for a total score between 4 and 12.6, 1, 5
- Pain: mild, moderate, or functional (pain with normal activity or at rest).1, 6
- Site: upper limb, lower limb (excluding peritrochanteric region), peritrochanteric region.7, 1
- Lesion type (radiographic): blastic, mixed, or lytic.6, 1
- Lesion size: <1/3, 1/3-2/3, or >2/3 of the cortical diameter involved.5, 6
Higher scores reflect more dangerous biomechanical situations: functional pain, weight‑bearing sites (especially peritrochanteric femur), lytic lesions, and extensive cortical destruction. In Mirels’ original 1989 series of 78 irradiated long‑bone lesions, fractures occurred almost exclusively in lesions scoring 9 or more, while lesions with scores ≤7 rarely fractured.7, 1, 5
Clinical Pearl: The Mirels Score predicts fracture risk over the subsequent months and serves as a decision‑support framework for whether to proceed with prophylactic fixation prior to radiotherapy, radiotherapy alone, or observation.
Clinically, it remains one of the most cited tools in orthopedic oncology for impending pathologic fracture risk.4, 8, 1
3. Why the Mirels Score Matters in Contemporary Bone & Spine Metastases Care
Pathologic fractures in long bones can lead to sudden immobility, uncontrolled pain, prolonged hospitalization, and technically demanding salvage surgery in often frail patients. Elective prophylactic fixation, performed before a fracture occurs, is associated with better functional outcomes, shorter hospital stays, and fewer complications compared with fixation after fracture.2, 4, 4
Overuse of prophylactic surgery, however, can expose patients to operative risk without clear benefit, particularly when life expectancy is limited or fracture risk is low. The Mirels Score offers a structured way to balance these trade‑offs, ensuring that decisions about fixation versus radiotherapy or conservative care are anchored in reproducible criteria rather than purely subjective judgment.3, 8, 10, 1
Without digital support, applying Mirels in real time is cognitively taxing: clinicians must remember four domains, point allocations, and threshold values, often while juggling imaging, systemic therapy plans, and patient preferences. On our platform, the Mirels Score calculator collapses these steps into a few intuitive selections and presents an immediately interpretable risk and recommendation, freeing the clinician’s attention to focus on nuanced, patient‑specific factors.1, 6, 7
4. Clinical Evidence, Guideline Alignment, and the Math Behind the Tool
4.1 Scoring logic and fracture‑risk thresholds
Mathematically, the Mirels Score is an additive model:
Total score = Pain (1-3) + Site (1-3) + Lesion type (1-3) + Size (1-3)
In the original and subsequent evaluations:
- Score <=7
- Score = 8
- Score >=9

Figure 1. The built‑in reference table maps Mirels Score ranges to estimated fracture risk and typical management, helping clinicians quickly translate a numeric score into a treatment plan.
5. Specific Use Cases and Applications in Clinical Practice
5.1 Pre‑radiotherapy planning for femoral metastases
For patients with femoral metastases undergoing palliative radiotherapy, the Mirels Score is frequently used to flag lesions that should be stabilized before radiation to avoid fracture through irradiated bone.2, 3, 1
Typical workflow:
- An orthopedic oncologist or radiation oncologist scores each femoral lesion using pain, site, type, and size.
- Lesions with scores >=9 are generally referred for prophylactic nailing or endoprosthetic replacement before radiotherapy, assuming reasonable performance status and life expectancy.9, 4, 1
- Lesions with scores <=7 usually receive radiotherapy alone, with continued surveillance.1, 6
5.2 MDT and tumor board triage of long‑bone metastases
Multidisciplinary tumor boards often review multiple patients with complex skeletal disease in a single session. For each long‑bone metastasis, the Mirels Score provides a common language between orthopedic surgeons, radiation oncologists, and medical oncologists.13, 7
Using the calculator live during MDT:
- The presenting clinician enters lesion characteristics while images are displayed.
- The numeric score and risk category appear instantly, guiding discussion (e.g., “This proximal femur lesion is Mirels 10—let’s prioritize surgical referral.”).4, 1
- The visual risk bar supports consensus building and ensures that borderline lesions (score 8) are recognized and discussed explicitly.14, 13
5.3 On‑call orthopedic and spine consultations
On‑call teams frequently receive referrals for patients with metastatic bone pain or incidental lesions on imaging. In these scenarios, our mobile‑optimized calculator helps clinicians:
- Estimate fracture risk at the bedside or in the emergency department.
- Decide whether to recommend strict non‑weight‑bearing, urgent surgery, or outpatient follow‑up.9, 7
- Document the score and rationale in the record, enhancing communication between specialist teams.7
5.4 Upper‑limb metastatic lesions
Upper-limb metastases, especially in the humerus, present different biomechanical challenges compared with the lower limb. A dedicated analysis of upper-limb lesions found that a threshold of >=7 may better balance sensitivity and specificity for humeral fractures.15, 16
5.5 Longitudinal monitoring of lesions at risk
Mirels scoring is also useful for tracking lesions over time: as pain worsens, lesions grow, or radiographic appearance shifts from mixed to lytic, the score may cross important thresholds.3, 4, 1
6. How the OncoToolkit Mirels Score Calculator Works
6.1 Input workflow: mirroring clinical reasoning
On our platform, the Mirels Score (Fracture Risk) calculator presents each domain as a clean, labeled input that matches real‑world documentation:
- Site of lesion: options labeled with anatomical location and point value (e.g., “Lower limb (2 pts)”).
- Pain severity: mild, moderate, or functional, aligned with Mirels’ original definitions.
- Lesion type: blastic, mixed, or lytic, reflecting radiographic morphology.
- Size (cortical involvement): <1/3, 1/3-2/3, >2/3 of the cortical diameter.
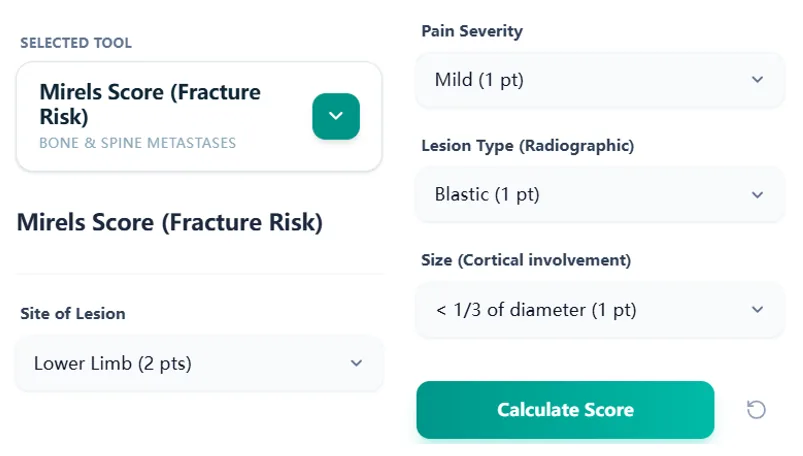
Figure 2. The input form presents each Mirels domain with clear clinical labels and point values, reducing memory burden during busy clinics.
6.2 Output and interpretation
The results pane shows:
- Numeric Mirels Score and risk category (Low Risk, Borderline, High Risk).19, 4, 1
- A brief interpretive statement and management recommendation.
- A color‑coded risk bar for visual context.

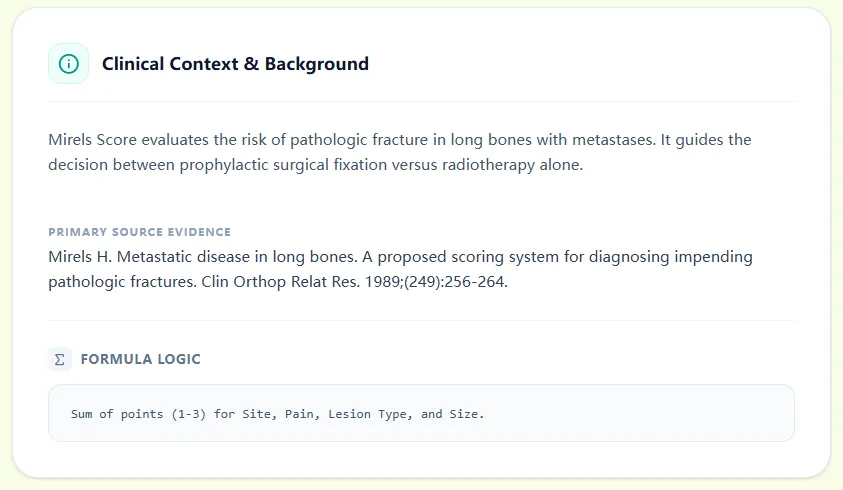
Figures 3 & 4. The results view translates numeric data into clinical actionable insights with evidence-based background summaries.
7. Guideline Alignment and Current Recommendations
Several orthopedic oncology and cancer care guidance documents reference the score:
- Orthopedic Oncology Materials: recommend prophylactic fixation for long bone metastases with Mirels Score ≥9.20, 7, 1
- ESMO Guidelines: recognize tools like Mirels to identify lesions at high risk that warrant stabilization.14
- Regional Consensus Documents: endorse Mirels as a practical framework for triaging metastatic long bone lesions.21
8. Recent Advances, Modifications, and Alternatives
8.1 Upper‑limb–specific thresholds
Experts recommend a lower decision threshold (>=7) for upper-limb lesions due to different load-bearing characteristics.15, 16
9. How the Platform Supports Clinical Care, Education, and Research
By digitizing this assessment, OncoToolkit provides:
- Point‑of‑care decision support: minimizing errors in assignment and threshold interpretation.
- Education: making it easy for trainees to explore how altering variables shifts management recommendations.
- Research: supporting institutional audits of adherence to prophylactic fixation policies.
10. Clinical FAQ on the Mirels Score Calculator
When should you not rely solely on the Mirels Score?
The Mirels Score should not be used in isolation for highly complex lesions with extensive soft-tissue mass or prior radiation.8, 18
11. Integrate the Mirels Score Calculator Into Your Workflow
To start using the Mirels Score (Fracture Risk) calculator, visit the link below to access our mobile-optimized tool.
Ready to Simplify Your Fracture Risk Assessment?
Quickly estimate risk and guide treatment decisions for long bone metastases at the point of care.
Use the Calculator Now
Free to use. No registration required.
At OncoToolkit, our goal is to turn complex oncology decision structures into intuitive, transparent calculators that reduce cognitive load and support high‑quality, guideline‑aligned care.
12. References
- Jawad MU, Scully SP. Mirels’ Classification: Metastatic Disease in Long Bones and Impending Pathologic Fracture. Clin Orthop Relat Res. 2010. Source
- Crenn V, Kolb F, Biau DJ, et al. High rate of fracture in long‑bone metastasis. Orthop Traumatol Surg Res. 2020. Source
- Are we underestimating pathological fracture risk in malignant bone disease? Orthop Traumatol Surg Res. 2025. Source
- Ramsey DC, Lindskog DM, Wojcik J, et al. Mirels Scores in Patients Undergoing Prophylactic Stabilization for Femoral Metastases. J Orthop Surg Res. 2020. Source
- Mirels H. Metastatic disease in long bones: A proposed scoring system for diagnosing impending pathologic fractures. Clin Orthop Relat Res. 1989. Source
- MDApp. Mirels Score – Criteria for Prophylactic Fixation (Calculator). 2020. Source
- Orthobullets. Impending Fracture & Prophylactic Fixation – Pathology. 2021. Source
- Advancements in Assessing Pathological Fracture Risk in Metastatic Bone Disease. 2025. Source
- Prophylactic Stabilization of Impending Fracture in Bone Metastasis – Mass General Advances in Motion. 2022. Source
- Kaupp SM, et al. Predicting Fracture Risk in Patients with Metastatic Bone Disease. Curr Osteoporos Rep. 2021. Source
- OncoToolkit internal reference table (Figure 1 data). 2026.
- OncoToolkit User Interface Design Documentation (Mirels Input Form). 2026.
- Hashimoto RE, et al. Using guideline‑based clinical decision support in oncological practice and MDT meetings. Int J Qual Health Care. 2022. Source
- ESMO Clinical Practice Guidelines: Bone Health in Cancer Patients. 2014. Source
- van der Wal BCH, Falke THM, Schaap GR, et al. Mirels’ score for upper limb metastatic lesions. J Shoulder Elbow Surg. 2022. Source
- Additional humeral-specific threshold analysis. J Shoulder Elbow Surg. 2022. Source
- OncoToolkit Clinical Background Panel for MS Score. 2026.
- Predicting the Risk for Pathological Fracture in Bone Metastases. Cancers (Basel). 2025. Source
- OncoToolkit Results Interpretation Pane and Logic. 2026.
- Primary Care Notebook. Mirels classification to predict possible pathological fracture. 2021. Source
- Chinese expert consensus on the diagnosis and treatment of malignant bone tumors. Orthop Surg. 2023. Source
- Modification to Mirels scoring system location component improves fracture prediction. 2023. Source
- Mah SJ, McDonald DJ, Damron TA. Internal validation of modified Mirels’ scoring system. 2024. Source
- Derikx LC, van Aken JB, Janssen SJ, et al. Finite element models for fracture prevention. Bone Rep. 2020. Source
- Eggermont F, Derikx LC, et al. Simulating activities of daily living with finite element analysis. J Orthop Res. 2015. Source
- Biomechanical analysis of femoral fracture prediction. J Eng Med. 2022. Source
- Structural rigidity analysis for skeletal lesions. J Orthop Res. 2015. Source
- O’Rourke DM, Eggermont F, et al. Agreement between finite element modelling methodologies. 2023. Source
- Ramsey DC, et al. Mirels Scores in Patients Undergoing Prophylactic Stabilization. J Orthop Surg Res. 2020. Source
- Transitioning Cognitive Aids into Decision Support Platforms. 2023. Source
- A Systematic Review of AI-Based Clinical Decision Support in Oncology. 2025. Source
- Using computerised decision support to improve MDT compliance. BMJ Open. 2012. Source
- CancerCalc. Mirels’ score: Pathological fracture risk. 2016. Source
- Medical-data-models.org. Mirels Score of Pathologic Fracture Risk. 2018. Source