- Introduction: Risk Stratification in MDS
Myelodysplastic syndromes (MDS) present a wide spectrum of clinical behavior, from indolent cytopenias to rapidly progressive disease with high risk of acute myeloid leukemia (AML) transformation. This heterogeneity makes prognosis estimation and treatment selection challenging in everyday hematology practice. [1], [2], [3]
The IPSS-R for MDS calculator on our platform translates the Revised International Prognostic Scoring System (IPSS-R) into a fast, mobile-friendly tool that delivers clear risk groups and estimated survival in seconds. At OncoToolkit, we’ve designed this implementation to reduce cognitive load, minimize “calculator fatigue,” and support hematologists and MDS oncologists at the bedside, in the clinic, and during MDT discussions.
- Understanding the IPSS-R for MDS
The IPSS-R (Revised International Prognostic Scoring System) is a prognostic model developed by the International Working Group for Prognosis in MDS using a large international cohort of untreated primary MDS patients. It stratifies patients into five risk categories—Very Low, Low, Intermediate, High, and Very High—based on a weighted sum of disease features. [2], [1]
IPSS-R integrates five key variables:
Each variable is assigned a numeric point value according to severity, and the total score predicts overall survival and risk of progression to AML. Historically, IPSS-R has become the standard reference in guidelines and clinical trials for risk-adapted treatment strategies in MDS, and it remains widely used even as newer molecular models such as IPSS-M emerge. [3], [5], [6], [1], [4]
- The Importance of IPSS-R Risk Stratification in Clinical Practice
IPSS-R risk category is central to multiple clinical decisions in MDS:
- Determining whether the disease is “lower-risk” or “higher-risk” for purposes of treatment intensity and monitoring. [7], [8]
- Guiding the use of hypomethylating agents, transplant referral, and supportive care–focused versus disease-modifying approaches. [9], [3]
- Informing patient counseling about expected survival and likelihood of AML evolution. [1], [3]
Without digital support, applying IPSS-R often requires navigating tables of cytogenetic risk groups, multiple laboratory cut points for marrow blasts and cytopenias, and distinct scoring bands for each variable. For busy clinicians, manually summing points and cross-referencing survival tables introduces friction, increases error risk, and can discourage consistent use, especially in MDT meetings or high-throughput clinics. [4], [1]
On our platform, the IPSS-R for MDS calculator streamlines this workflow into a single responsive interface optimized for desktop, tablet, and mobile. At OncoToolkit, we’ve built the tool so that you can input cytogenetics and key blood counts, tap “Calculate Score,” and immediately see the total IPSS-R score, risk group, and estimated median survival—ready to document or discuss with the team.
- Clinical Evidence, Validation, and Regional Data
4.1 The Logic and Math Behind IPSS-R
The original IPSS-R model was derived from data on more than 7,000 untreated primary MDS patients contributed by international centers under the aegis of the MDS Foundation. Using multivariable Cox proportional hazards modeling, Greenberg et al. assigned weights to each variable based on their independent association with overall survival and AML transformation. [2], [1], [4]
4.2 Global Validation: Western and Asian Cohorts
4.3 Guideline Endorsement and Clinical Practice Recommendations
Major guidelines and consensus documents incorporate IPSS-R into risk assessment for MDS:
- NCCN Guidelines (2025): Emphasize IPSS-R for initial stratification and guiding treatment algorithms for supportive care and HMAs. [15]
- ESMO Guidelines: Recommend IPSS-R as a standard tool for everyday risk-adapted therapy. [9]
- Nordic MDS Group: Use IPSS-R as the backbone for transplant decision making. [17]
4.4 Limitations and Evolving Landscape
Performance may be less precise in therapy-related or secondary cases. It does not incorporate somatic mutations (e.g., TP53, ASXL1), which are now addressed by the complementary IPSS-M system. [18], [19]
- How the OncoToolkit IPSS-R for MDS Calculator Works
5.1 Step-by-Step User Workflow and Clinical Use Cases
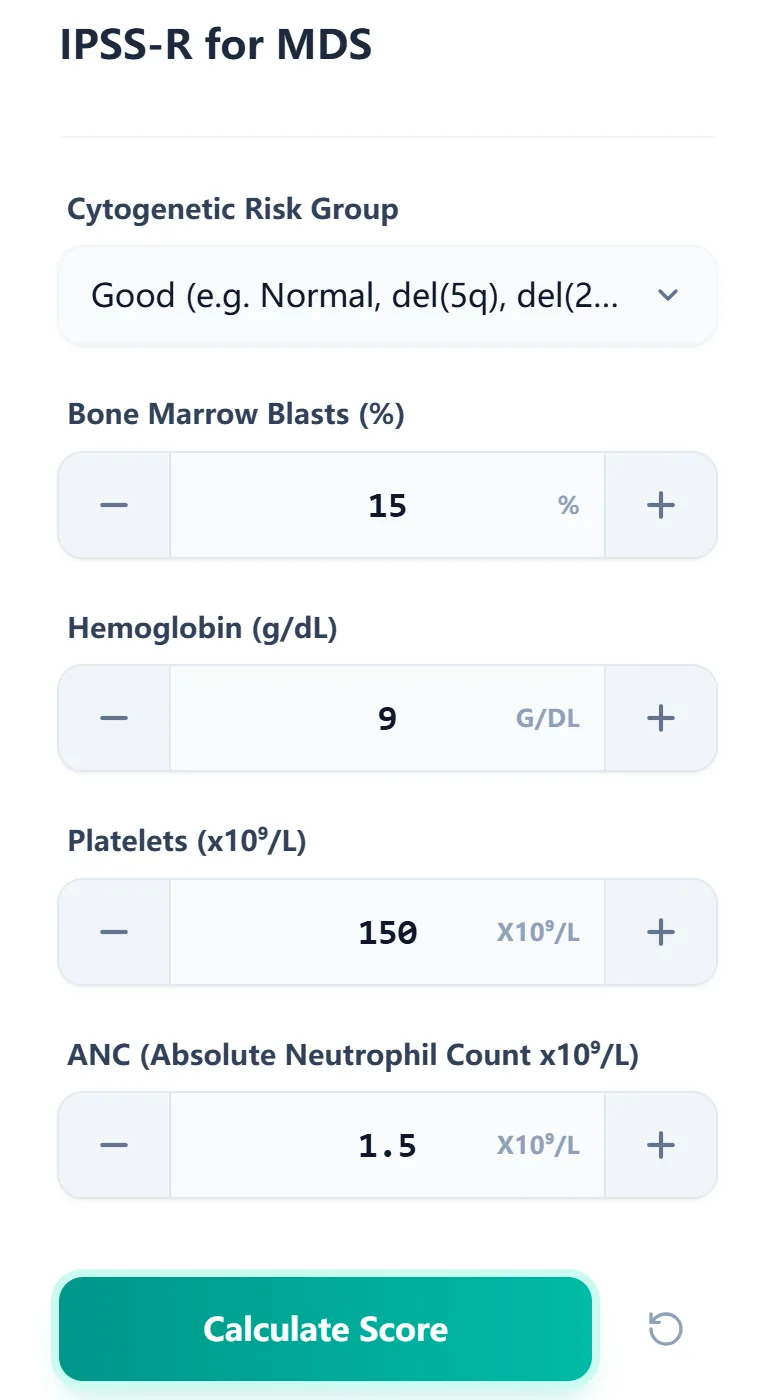
Figure 1. The input form allows you to select cytogenetic risk group and enter bone marrow blasts, hemoglobin, platelets, and ANC using intuitive controls.
5.2 From Score to Risk Group and Survival
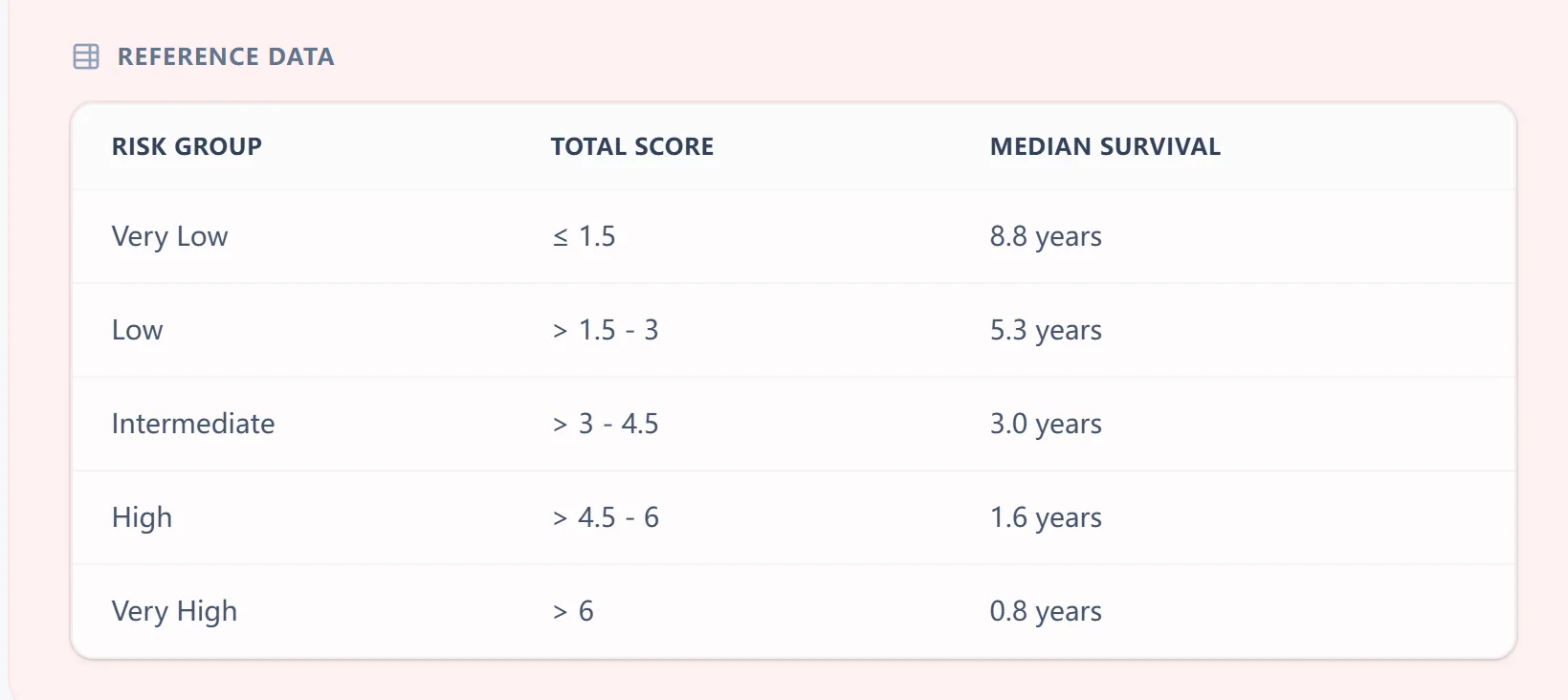
Figure 2. Reference table showing how IPSS-R total scores correspond to Very Low through Very High risk groups.
| Risk group | IPSS-R total score | Approximate median survival* |
|---|---|---|
| Very Low | ≤ 1.5 | 8.8–11 years |
| Low | > 1.5–3 | 5–6 years |
| Intermediate | > 3–4.5 | ~3 years |
| High | > 4.5–6 | ~1.5–2 years |
| Very High | > 6 | <1–1.5 years |
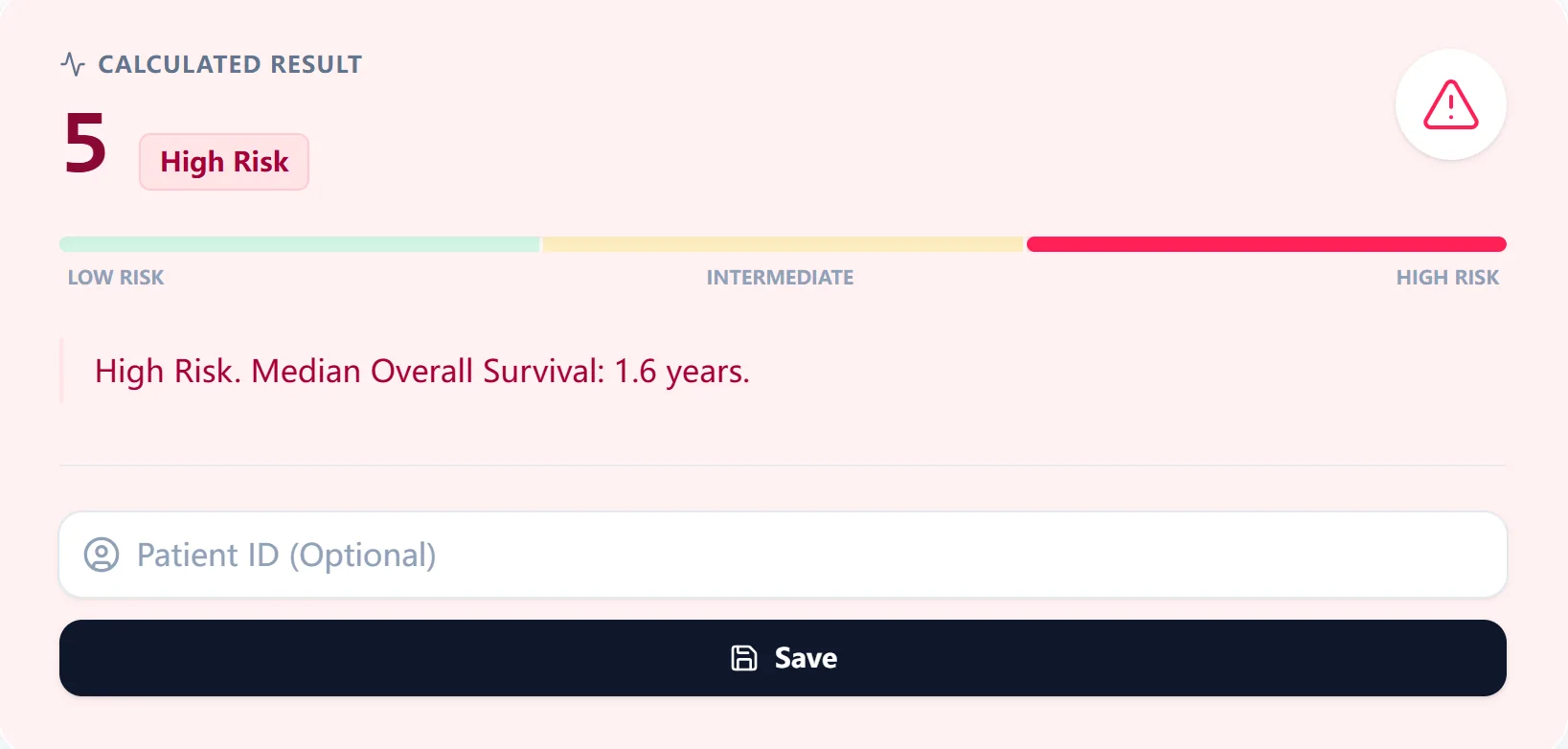
Figure 3. Example output displaying an IPSS-R total score and risk group highlighted along a colored risk bar.
- Clinical Context, Background, and Teaching Value
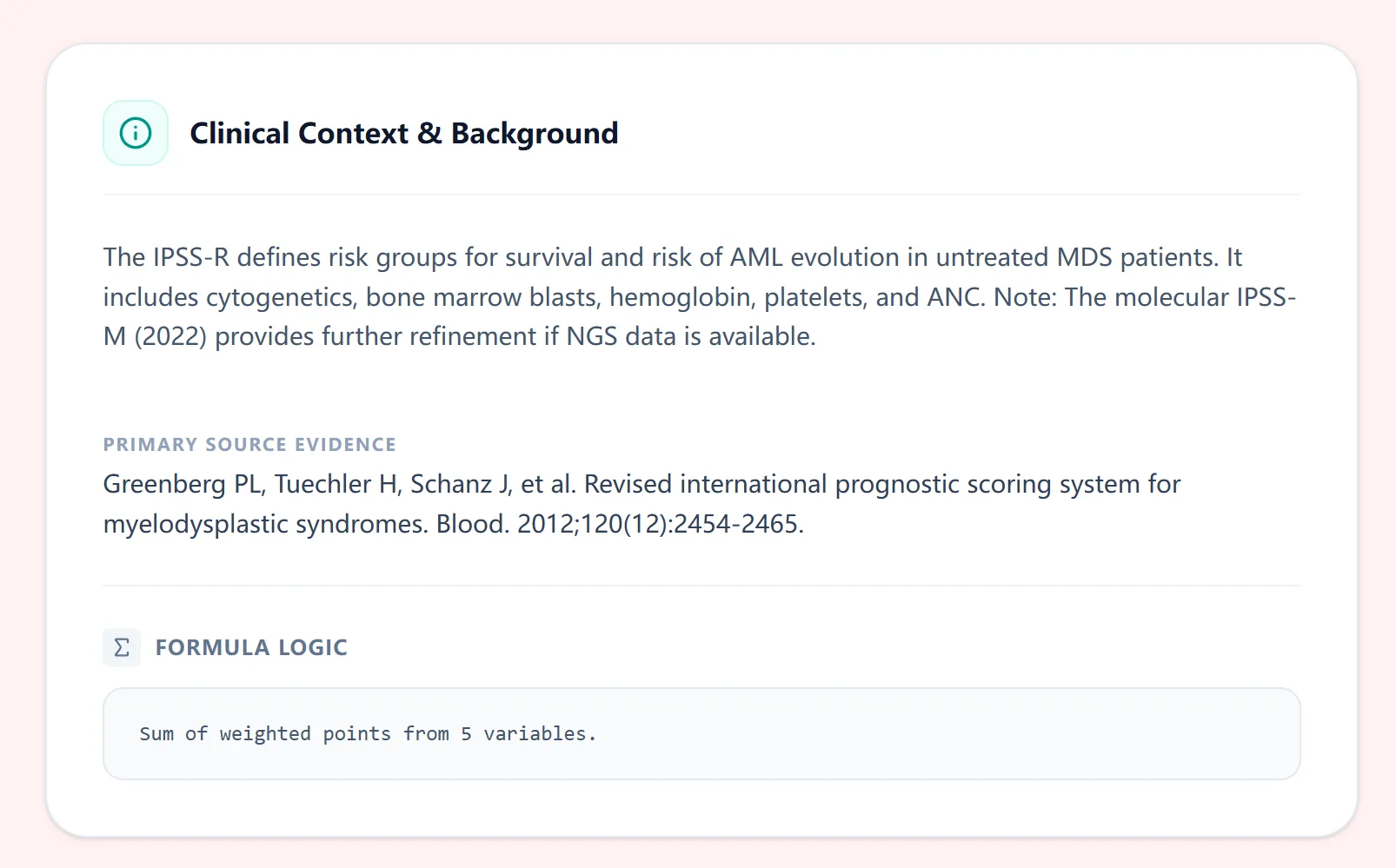
Figure 4. Background panel summarizing the clinical role of IPSS-R in MDS and citing the original validation study.
- How Our IPSS-R Calculator Supports Care, Education, and Research
Clinical Support
Stage at diagnosis and prepare for MDT meetings with standardized risk reporting.
Education
Run "what-if" simulations with trainees to explore variable weight and prognosis shifts.
Research/QI
Standardize risk classification across datasets for high-quality outcome analysis.
- IPSS-R, IPSS-M, and Recent Updates to Prognostic Scoring
8.1 How IPSS-M Builds on IPSS-R
The Molecular International Prognostic Scoring System (IPSS-M) represents a major update to risk assessment in MDS by integrating somatic mutation data with clinical and cytogenetic features. [6], [18], [5]
- Clinical FAQ
Can the IPSS-R score be used in patients with prior therapy or secondary MDS?
IPSS-R was derived primarily in untreated, de novo MDS. Performance may be less accurate in therapy-related or heavily pretreated disease. [2]
- Call to Action: Start Using the IPSS-R for MDS Calculator Today
To integrate structured risk assessment into your MDS practice, open the calculator at: https://oncotoolkit.com/calculator/ipss-r-AML-Prognostic-MDS.
Ready to Simplify Your MDS Risk Stratification?
Calculate IPSS-R scores instantly and support evidence-based decisions at the point of care.
Open IPSS-R Calculator
Free to use • No registration required • Clinically Validated
References
- MDS Foundation. IPSS-R Document. Source
- Greenberg PL, et al. Revised international prognostic scoring system for myelodysplastic syndromes. Blood. 2012. Source
- American Cancer Society. Staging Myelodysplastic Syndromes. Source
- Pfeilstöcker M, et al. The International Prognostic Scoring System-Revised: Clinician’s Application Manual. Source
- Molecular prognostic systems in MDS. Source
- Bernard E, et al. Molecular International Prognostic Scoring System for Myelodysplastic Syndromes. JCO. 2022. Source
- Spotlight on Anemia. Risk Stratification in MDS. Source
- Blood Cancer UK. MDS Prognosis. Source
- HealthHelp Clinical Guidelines. Source
- Della Porta MG, et al. Validation of IPSS-R in a large series of MDS patients. Source
- MDS Knowledge is Power. Know Your Score. Source
- Lin CC, et al. Validation of IPSS-R in Taiwanese patients with MDS. AJH. Source
- Asian cohort analysis in MDS. Source
- Characteristics of East Asian MDS patients. Source
- NCCN Guidelines Mar 2025. Source
- MDS Management Guidelines. Source
- Nordic MDS Group Guidelines. Source
- Molecular reclassification of MDS risk. Source
- Heterogeneity in intermediate-risk MDS. Source
- MDS Hub. Understanding IPSS-R and IPSS-M. Source
- Validation of IPSS-M in international cohorts. Source
