MELD Score Calculator for Liver Transplant and TIPS
Accurately estimate 3-month mortality in cirrhosis patients using the original MELD Score model to guide transplant and TIPS decisions.

Quick Navigation
Managing decompensated cirrhosis and hepatocellular carcinoma (HCC) requires difficult conversations about prognosis, transplant timing, and procedural risk. Even for experienced hepatologists and HCC oncologists, integrating renal function, synthetic failure, portal hypertension, and tumor status into a single, consistent risk estimate can be challenging in real time.
The Model for End‑Stage Liver Disease (MELD) Score offers a standardized, quantitative way to estimate short‑term mortality in patients with advanced liver disease, and it underpins many modern liver transplant allocation systems worldwide. At OncoToolkit, we’ve built an original MELD Score calculator that implements the classic formula, exposes the full calculation logic, and instantly maps scores to 3‑month mortality estimates—reducing cognitive load in busy clinics, transplant assessments, and multidisciplinary team (MDT) meetings.1

Figure 1. Clinical background card summarizing MELD as a tool to predict short‑term mortality in end‑stage liver disease.
1. Understanding the MELD Score and Its Clinical Significance
The MELD Score is a continuous risk model developed to predict 3‑month mortality in patients with cirrhosis and end‑stage liver disease. It was first described by Kamath and colleagues in 2001 in a cohort of cirrhotic patients undergoing transjugular intrahepatic portosystemic shunt (TIPS), where it outperformed several alternative models for peri‑procedural survival prediction. The same model was subsequently validated in broader end‑stage liver disease populations and adopted as a cornerstone of liver transplant allocation policies, including in the United States. [2], [3], [4], [1]
The original MELD model uses three routinely available laboratory values—serum creatinine, total bilirubin, and international normalized ratio (INR)—to generate a score typically ranging from 6 to 40. Higher scores correspond to greater short‑term mortality risk and greater expected survival benefit from liver transplantation. [5], [1]
1.1 Components and the Original MELD Formula
For patients ≥12 years with chronic liver disease or cirrhosis, the original MELD Score is constructed from: [6], [1]
- Serum creatinine (mg/dL), with values capped (e.g., at 4.0 mg/dL) and special handling for dialysis
- Total bilirubin (mg/dL)
- INR
Kamath et al. derived the coefficients using Cox proportional hazards regression, identifying log‑transformed creatinine, bilirubin, and INR as independent predictors of 3‑month mortality. The linear predictor was then scaled to improve interpretability, producing the widely used expression: [7], [2]
MELD = 10 x [0.957 x ln(creatinine) + 0.378 x ln(bilirubin) + 1.12 x ln(INR) + 0.643]
On our platform, the MELD calculator faithfully implements this original formulation, including standard caps and floors for extreme lab values and explicit handling of dialysis, mirroring widely used clinical calculators and transplant program conventions. [6]
1.2 Intended Patient Population for MELD Assessment
The original MELD Score is most appropriate for: [8], [1], [6]
- Patients ≥12 years with cirrhosis or end‑stage chronic liver disease
- Decompensated cirrhosis where short‑term prognosis (≈3 months) is clinically relevant
- Candidates for TIPS or liver transplantation, including those with HCC meeting transplant criteria
OncoToolkit surfaces this applicability in the calculator’s clinical context panel, reminding clinicians to confirm that MELD is the right tool for the patient in front of them.
2. Why the MELD Score Calculator is Essential in Hepatology and HCC
For hepatologists and HCC oncologists, MELD has become central to discussions about transplant referral, listing, and timing. The score offers several practical advantages: [9], [5], [1]
- Objective risk stratification: MELD provides a continuous, reproducible estimate of short‑term mortality that is less subjective than clinical gestalt or semi‑quantitative scores.
- Alignment with transplant benefit: Higher MELD scores correlate with greater survival benefit from liver transplantation, supporting prioritization of patients at greatest risk. [5]
- Utility across scenarios: MELD informs decisions about TIPS, intensive care escalation, surgical risk, and broader cirrhosis management, not just transplant waiting lists. [9]
Clinical Pearl: Digital tools like the MELD Score calculator reduce cognitive load during MDT discussions, allowing clinicians to focus on patient care rather than complex logarithmic math.
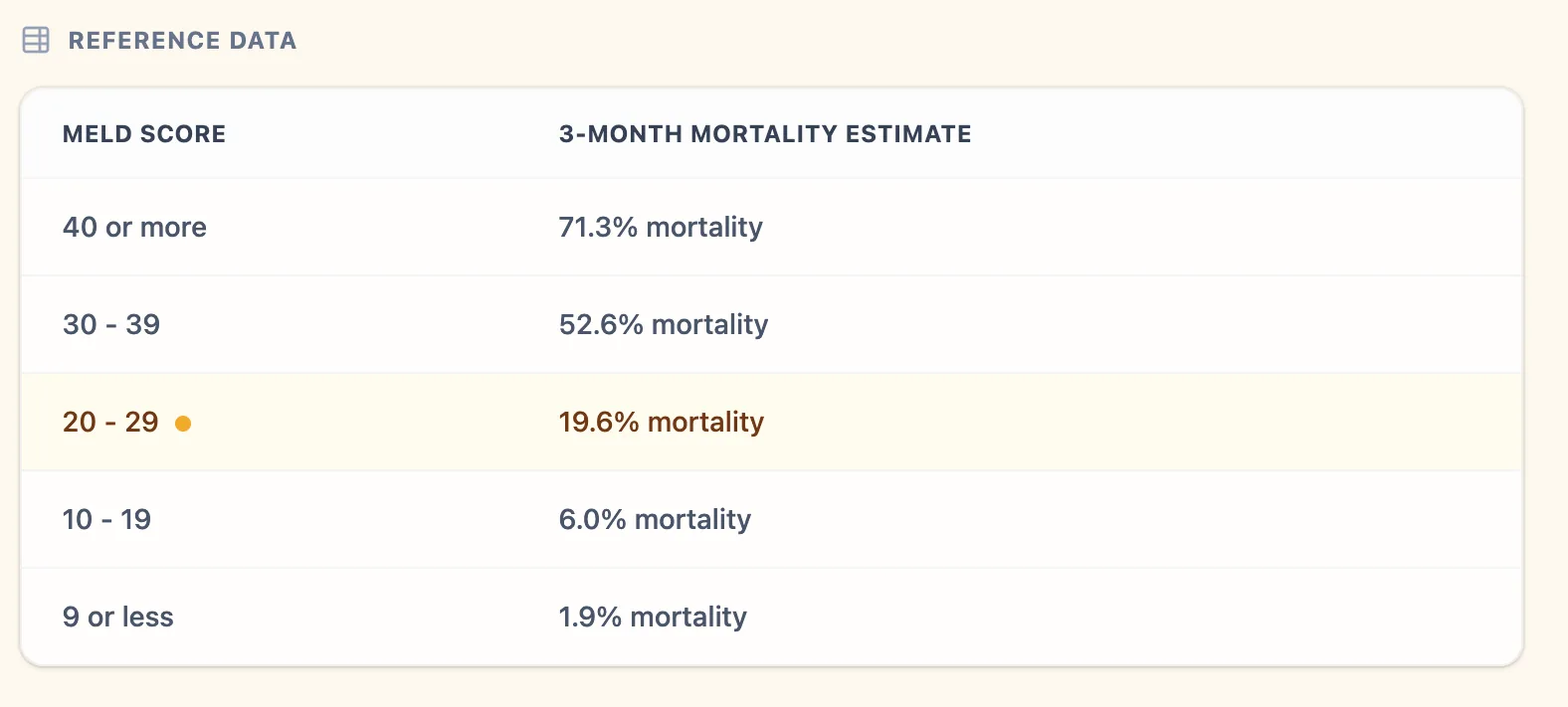
Figure 2. Reference table mapping MELD Score bands to approximate 3‑month mortality estimates.
3. Clinical Evidence, Validation, and the Mathematics of the MELD Score
3.1 Initial Development and Validation in TIPS Cohorts
The original MELD model was derived from a multicenter cohort of patients with cirrhosis undergoing TIPS, where the goal was to identify predictors of 3‑month survival after the procedure. In this study, creatinine, bilirubin, and INR remained independently associated with mortality in multivariable Cox models. [3], [10], [2], [7]
3.2 Evolution of MELD into a Global Transplant Allocation Tool
Recognizing its performance and objectivity, policy makers incorporated MELD into the United Network for Organ Sharing (UNOS) adult liver allocation system beginning in 2002. This shift moved allocation from time‑on‑list to disease severity, with priority largely determined by MELD. [4], [11], [8], [5]
International guidelines and expert reviews from societies such as AASLD and EASL endorse MELD as the preferred tool for assessing severity of end‑stage liver disease and guiding transplant referral decisions. [12], [8], [9]
3.3 Validation Across Broader Cirrhosis Populations
Beyond TIPS, MELD has been validated in multiple settings: [8], [1], [9]
- Wait‑listed transplant candidates, where MELD strongly predicts wait‑list mortality.
- Hospitalized decompensated cirrhosis, where rising MELD correlates with mortality.
- Post‑transplant outcomes, showing associations between pre‑transplant MELD and perioperative risk. [13], [14]
Across these cohorts, MELD often equals or surpasses Child‑Pugh in predictive performance for short‑term mortality. [1], [9]
3.4 MELD Mortality Risk Categories and Clinical Interpretation
To support bedside decision‑making, many programs interpret MELD in terms of mortality bands:
- MELD ≤9: 3‑month mortality around 1–2%
- MELD 10–19: roughly 6% 3‑month mortality
- MELD 20–29: approximately 20% 3‑month mortality
- MELD 30–39: around 50% 3‑month mortality
- MELD ≥40: 3‑month mortality exceeding 70% [15], [6]
3.5 Known Limitations and Special Clinical Populations
Thoughtful clinicians recognize that MELD is powerful but not perfect: [8], [9], [1]
- Designed for chronic end‑stage liver disease, not acute liver failure.
- Creatinine can underestimate renal dysfunction in sarcopenic patients.
- Does not fully capture complications like refractory ascites or tumor burden for HCC. [16], [17]
4. MELD Score Nuances for HCC and TIPS Decision-Making
4.1 Navigating MELD and HCC Transplant Pathways
In HCC, MELD provides an objective measure of liver dysfunction but does not incorporate tumor size or number. To address this, allocation systems use MELD exception points for HCC patients meeting criteria such as Milan. [18], [19], [9]
Studies have explored HCC‑specific derivatives like HCC‑MELD, though standard MELD plus exception policies remain the primary framework for prioritizing HCC patients. [20], [21]
4.2 Using MELD for TIPS Candidacy Decisions
MELD remains central to evaluating TIPS candidacy. Patients with MELD scores above thresholds (often around 18–20) face substantially higher post‑TIPS mortality, necessitating careful risk–benefit assessment. [22], [23]
5. How to Use the OncoToolkit MELD Score Calculator
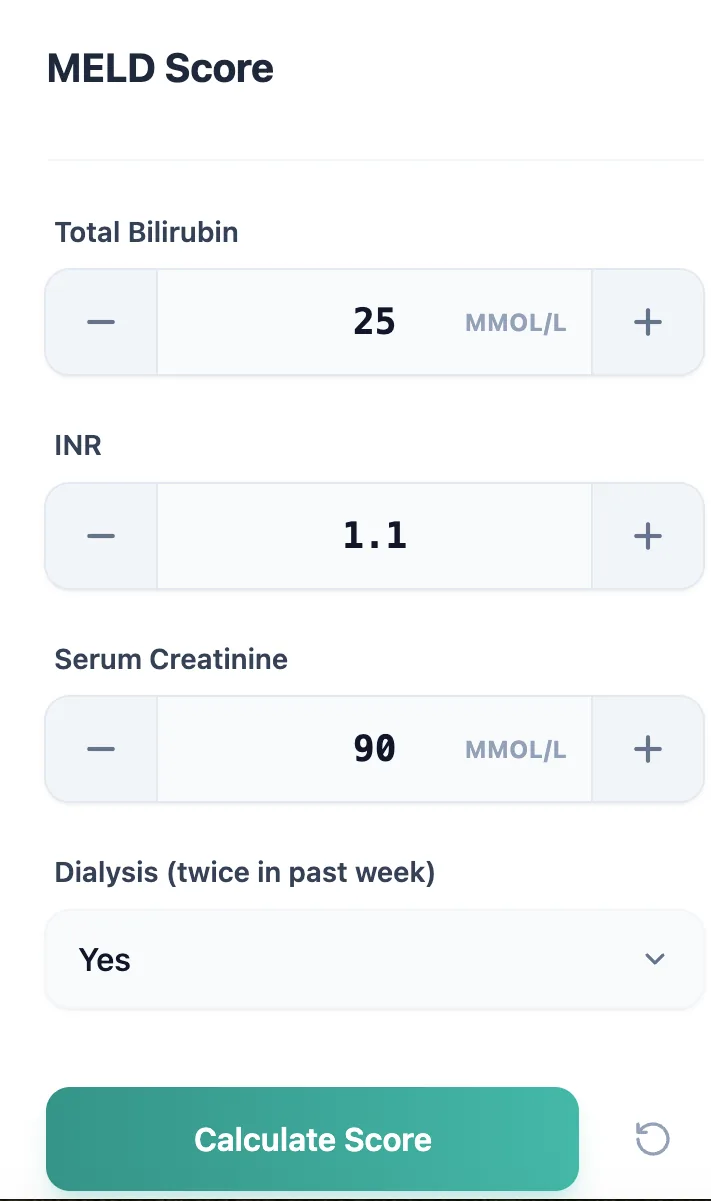
Figure 3. Input form capturing total bilirubin, INR, creatinine, and dialysis status.
5.1 A Step-by-Step Guide: From Labs to Risk Assessment
- Enter bilirubin, INR, and creatinine: Input laboratory values with provided unit hints.
- Specify dialysis status: Toggle if the patient required dialysis at least twice in the previous week.
- Calculate MELD: The system applies the natural logarithm transformation and scaling.
- Interpret score and risk band: View the color-coded results and 3-month mortality estimate.
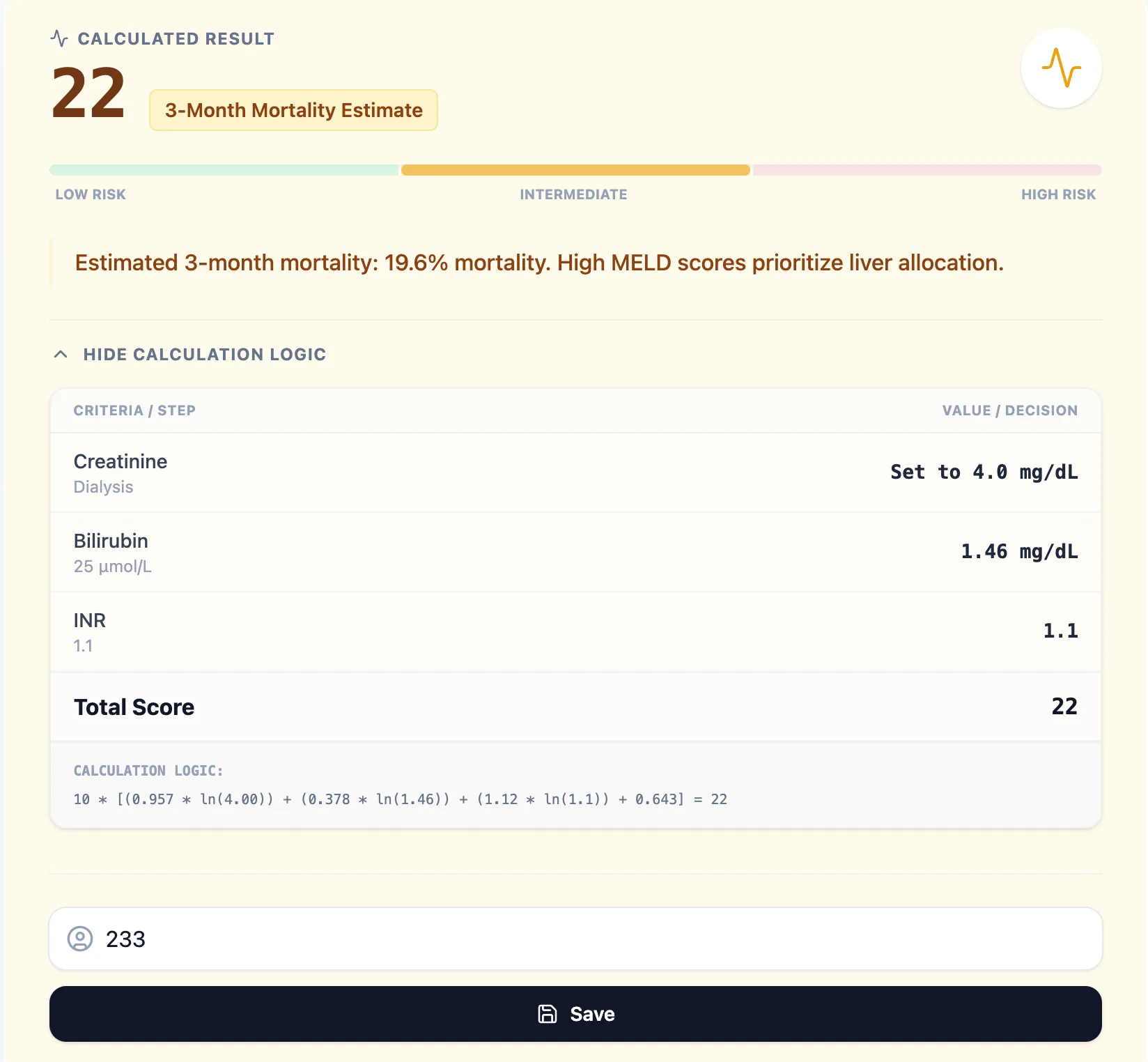
Figure 4. Example result showing a MELD Score of 22 with an intermediate‑risk band and calculation logic.
5.2 Understanding the Transparent Formula Logic
OncoToolkit displays the step‑by‑step calculation including capped lab values and coefficients, facilitating trust, teaching, and clinical auditability. [6]
6. Implementing MELD in Clinical Care, Education, and Research
6.1 Enhancing Routine Clinical Decision Support
- Transplant referral timing: Trajectories and thresholds (e.g., ≥15) prompt formal evaluation. [15], [9]
- TIPS selection: Assessing whether procedural risk is acceptable. [23], [22]
- Counseling: Communicating prognosis to families with objective data.
6.2 Clinical Education and Trainee Simulation
The platform supports education by showing full logic and allowing “what‑if” simulations to demonstrate how renal dysfunction or cholestasis drives risk. [24], [4], [5]
6.3 Support for Outcomes Research and Quality Improvement
Standardized calculation ensures rigorous data for QI projects, helping maintain consistent documentation in MDT summaries and clinical notes. [14], [13], [8]
7. Clinical FAQ: Expert Answers on the MELD Score Calculator
When should you not rely solely on the MELD Score?
MELD should be combined with clinical assessment in cases of severe encephalopathy, refractory ascites with preserved labs, or rapidly progressive HCC. [9], [8]
How does MELD compare with Child‑Pugh and ALBI?
MELD is preferred for transplant and TIPS decisions due to its objective scaling; Child‑Pugh and ALBI remain useful for broader staging and surgical risk. [16], [8], [9]
Is the original MELD Score applicable to HCC patients?
Yes, for assessing underlying liver function, but it must be paired with exception scores and tumor-based criteria (Milan/UCSF). [19], [18], [9]
8. Action Plan: Integrating the MELD Score Calculator into Your Workflow
To integrate MELD seamlessly into your practice, open the calculator now at /calculator/meld-liver-transpplant. Try it on several representative cases to appreciate how changes in lab values translate into different risk bands.
As you adopt MELD, consider using related tools such as Child‑Pugh, ALBI grade, and BCLC staging to build a consistent, evidence‑based framework for managing complex liver disease.
Ready to Simplify Your Liver Risk Assessments?
Calculate 3-month mortality and prioritize transplant care in seconds with our MELD tool.
Use the MELD Calculator Now
Free to use. No registration required.
References
- Wiesner R, et al. Model for End-stage Liver Disease (MELD) and allocation of donor livers. Gastroenterology. 2003. Source
- Kamath PS, et al. A model to predict survival in patients with end-stage liver disease. Hepatology. 2001. Source
- Kamath PS, et al. MELD Score Development. Hepatology. 2001. Source
- Brown RS Jr. MELD and the future of liver allocation. Am J Transplant. 2007. Source
- Hoppe L, et al. MELD-Na and Transplant Benefit. PMC 2022. Source
- University of Washington. Clinical Calculators: MELD. Hepatitis B Online. Source
- Kamath PS, Kim WR. The model for end-stage liver disease (MELD). Hepatology. 2007. Source
- Sacleux SC, Samuel D. A Critical Review of MELD as a Reliability Tool. PMC 2023. Source
- Chowdhury S, et al. Clinical Utility of MELD. PMC 2014. Source
- 2 Minute Medicine. The MELD Score: Predicting Survival Classics Series. Source
- Wiesner RH, et al. Liver Transpl. 2002. Source
- AASLD. Why do we use the MELD Score? Liver Fellow Network. Source
- PLOS ONE. MELD Trajectories and Survival Analysis. 2019. Source
- Gentry SE, et al. Pre-transplant MELD and Post-transplant Outcomes. PMC 2013. Source
- Mayo Clinic. MELD Score for Liver Disease: About. Source
- Journal of Hepatology. MELD vs Child-Pugh vs ALBI. Source
- UKELD Score and Clinical Staging. PMC 2017. Source
- HCC MELD Exception Policies. PMC 2015. Source
- OPTN. Improving Liver Allocation MELD/PELD. Source
- HCC-MELD Scoring Refinements. PubMed 2017. Source
- Validation in Asian Populations. PMC 2022. Source
- TIPS Outcomes and MELD Thresholds. PMC 2014. Source
- MELD in Refractory Ascites/TIPS. PMC 2021. Source
- AASLD. Why Series: MELD Education. Source