Comprehensive Nottingham Prognostic Index (NPI) Breast Cancer Calculator
Master the Nottingham Prognostic Index (NPI) to stratify breast cancer prognosis. Learn the formula, validation studies, and how to use our digital calculator for MDT decisions.

Quick Navigation
1. Introduction
From initial diagnosis through long-term survivorship, breast surgeons must repeatedly synthesize pathology, biomarkers, imaging, and patient factors into a cohesive prognostic storyline. The cognitive load is high: TNM stage, grade, nodal burden, receptor status, genomic assays, comorbidities, and patient preferences all interact, often during time-pressured clinics or multidisciplinary team (MDT) meetings.
The Nottingham Prognostic Index (NPI) remains one of the most robust and widely validated pathology-based tools for operable primary breast cancer, integrating tumor size, lymph node status, and histologic grade into a single continuous score that correlates with 5- and 10-year outcomes. At OncoToolkit, we've built an NPI calculator, available at /calculator/nottingham-prognostic-index-breast-cancer, that modernizes this classic index with dynamic survival estimates, decision prompts, and workflow features designed specifically for breast surgical oncologists and breast surgeons.1, 2, 3, 4
2. What Is the Nottingham Prognostic Index?
2.1 Historical development
The concept of a composite prognostic index for breast cancer was first articulated by Haybittle, Blamey, Elston, and colleagues in Nottingham in the early 1980s. In an initial cohort of several hundred women with primary operable invasive breast cancer, they used multivariable analyses to identify tumor size, lymph node status, and histologic grade as independent predictors of long-term survival. The Nottingham group then combined these variables into a simple linear index, the Nottingham Prognostic Index, which has since been validated in multiple external series and screening populations.2, 5, 6, 7, 8, 9
The index was designed to be practical for routine pathology: it relies on tumor size measured in centimetres, qualitative grading using the Nottingham/Elston-Ellis system, and categorized nodal involvement from standard axillary surgery. This simplicity allowed rapid uptake across UK centers and later internationally, long before molecular subtyping and genomic assays were available.6, 10
2.2 Components and formula
NPI uses three routinely reported parameters:
- Tumor size (invasive component) in centimetres
- Axillary nodal status, categorized as node-negative, 1-3 positive nodes, or >=4 positive nodes
- Histologic grade (Nottingham grade I-III)
The original and still widely used formula is:
NPI = 0.2 x Tumor size (cm) + Nodal stage (1-3) + Grade (1-3)where nodal stage is scored as 1 for node-negative, 2 for 1-3 positive nodes, and 3 for >=4 positive nodes, while grade is scored 1, 2, or 3 according to differentiation. The 0.2 coefficient for size balances the influence of tumor diameter against nodal and grade factors so that a 5-cm increase contributes roughly the same magnitude as moving one category in nodal status.5, 8, 1, 6
2.3 What the index predicts
The NPI was initially calibrated against overall and breast cancer-specific survival over 10-15 years, demonstrating clear separation of outcome curves across score bands. It has since been applied to:2, 5
- All-cause and breast cancer-specific survival in symptomatic and screen-detected populations9, 11, 2
- Distant metastasis risk in ER-positive, HER2-negative disease when combined with biomarkers (NPI+ and NPx)12, 13, 14
- Outcome prediction in specific subtypes such as triple-negative breast cancer, where higher NPI strongly correlates with poor prognosis.15
In modern practice, NPI sits alongside TNM staging, intrinsic subtype, and genomic assays as a core clinicopathologic baseline, particularly important in settings where multigene tests are unavailable or selectively used.16, 17
3. Why NPI Still Matters Across the Full Course of Breast Cancer Care
3.1 Early post-diagnosis and surgical decision-making
At diagnosis, surgeons must rapidly triage patients into appropriate pathways: primary surgery, neoadjuvant systemic therapy, or additional staging. While NPI itself is traditionally applied to post-operative pathology, understanding the eventual NPI range can inform the expected risk trajectory even before surgery. A large, high-grade tumor with clinically positive nodes will almost certainly yield a high NPI, flagging the need for robust systemic planning and potentially clinical trial discussions.18, 19
Post-operatively, the NPI formalizes what many surgeons intuit: small, low-grade, node-negative tumors have excellent outcomes; larger, higher-grade, node-positive tumors fare worse. By turning this into a reproducible score with survival bands, NPI:
- Supports structured post-operative consultations, offering patients a quantified yet understandable risk estimate.
- Provides a common language across surgeons, medical oncologists, and radiation oncologists in MDTs.
- Helps determine whether genomic assays or additional imaging are likely to change management in borderline cases, especially in ER-positive, HER2-negative disease.
3.2 Adjuvant systemic therapy and MDT planning
In modern guidelines, genomic signatures and subtype-specific factors increasingly guide adjuvant chemotherapy decisions, but NPI still influences how MDTs interpret borderline scenarios. Examples include:17, 16
- A patient with ER-positive, HER2-negative, node-negative disease and a low genomic risk but borderline-high NPI due to size or grade may prompt more careful discussion of chemotherapy benefit.
- Conversely, a patient with low NPI and intermediate genomic risk may be viewed more conservatively, particularly if comorbidities or toxicity risks are significant.
NPI also remains central to audit and service evaluation, offering a standardized way to adjust for case mix when comparing systemic therapy utilization or outcomes over time.19, 18
3.3 Long-term follow-up, survivorship, and late events
The prognostic signal of NPI extends beyond 5 years. Long-term data from screened populations and institutional cohorts show persistent differences in 10-year survival across NPI categories. For ER-positive disease, where late recurrences remain a concern, NPI complements tools such as CTS5 when assessing the value of extended endocrine therapy.11, 9, 2
In survivorship clinics, a documented NPI score helps:
- Stratify follow-up intensity and imaging frequency in line with local pathways.
- Provide context for late counselling, for example, explaining why extended endocrine therapy or closer surveillance was initially recommended.
- Facilitate second opinions by summarizing baseline risk in a single number that can be quickly understood across institutions.
Throughout the full course of care, NPI acts as a continuous thread that anchors evolving clinical decisions, even as additional prognostic data accumulate.
4. Clinical Evidence, Validation, and the Math Behind the Tool
4.1 Key derivation and confirmation studies
The foundational paper by Haybittle and colleagues in 1982 outlined the original prognostic index, showing that combining tumor size, nodal status, and grade yielded better discrimination than any single factor. Subsequent studies in Nottingham and elsewhere confirmed its predictive power in larger cohorts, including confirmatory analyses published in the early 1990s and 2000s.7, 20, 21, 5, 6
Galea et al. validated the index in more than 1,600 patients, demonstrating statistically significant survival differences between score bands and proposing formal cut-offs for prognostic groups. Later work examined NPI in the context of population-based breast screening programmes, showing that the index remained informative even when tumors were detected earlier and were generally smaller and lower grade.8, 6, 9, 11, 2
4.2 Survival bands and multi-group schemas
Beyond the simple 3-group structure, several papers propose more granular schemas:
- A 4-group system (excellent, good, moderate, poor) splits the intermediate range around 3.4-5.4 into two categories to improve clinical discrimination.11, 2
- Some authors describe a 5-group variant, adding "very poor" prognosis for very high NPI scores, particularly relevant before modern HER2-targeted and taxane-based therapies.3, 2
Approximate survival data from large series suggest:
| NPI group (example 4-group schema) | NPI range | 5-year survival | 10-year survival |
|---|---|---|---|
| Excellent | <= 2.4-3.4 | >95% | ~90% |
| Good | ~3.41-4.4 | ~85-90% | ~75-82% |
| Moderate | ~4.41-5.4 | ~70-80% | ~60-70% |
| Poor / Very poor | >5.4 | ~30-50% | ~25-40% |
Exact percentages vary between cohorts, eras, and the use of systemic therapy, but the directionality and separation of curves are consistent. OncoToolkit's calculator allows you to select between 3- and 4-group schemas, with survival ranges derived from published series and clearly labelled as estimates rather than guarantees.22, 3, 2
4.3 Subtype-specific performance and refinements
Several modern studies have examined how NPI interacts with intrinsic subtype and biomarkers:
- In triple-negative breast cancer, NPI retains prognostic significance, with high scores associated with particularly poor outcomes and early relapse.15
- NPI has been integrated into composite tools such as NPI+, which combines the index with immunohistochemical surrogates for molecular subtypes to refine risk stratification, especially in ER-positive, HER2-negative disease.23, 24, 12
- More recent work (e.g., NPx) uses NPI alongside gene expression classifiers to stratify risk of distant metastasis in hormone receptor-positive cohorts.13, 14, 25
These developments reinforce NPI's role as a building block in modern prognostic modeling rather than an obsolete relic.
4.4 Limitations and contemporary interpretation
Despite its strengths, NPI has well-recognized limitations:
- It predates routine HER2 testing, Ki-67 assessment, and modern genomic signatures, so it cannot fully capture aggressive biology in small tumors or low-burden disease.25, 12, 23
- Most early validation cohorts were Western and treated before the routine use of taxanes, trastuzumab, and contemporary endocrine strategies, making absolute survival figures historical rather than directly transferable to today's patients.26, 3, 2
- Its performance may be less reliable when applied to post-neoadjuvant pathology, inflammatory breast cancer, or rare histologies that behave differently from typical invasive ductal or lobular carcinomas.16, 16
OncoToolkit explicitly surfaces these caveats in the clinical background panel so users understand what the calculator can and cannot tell them.
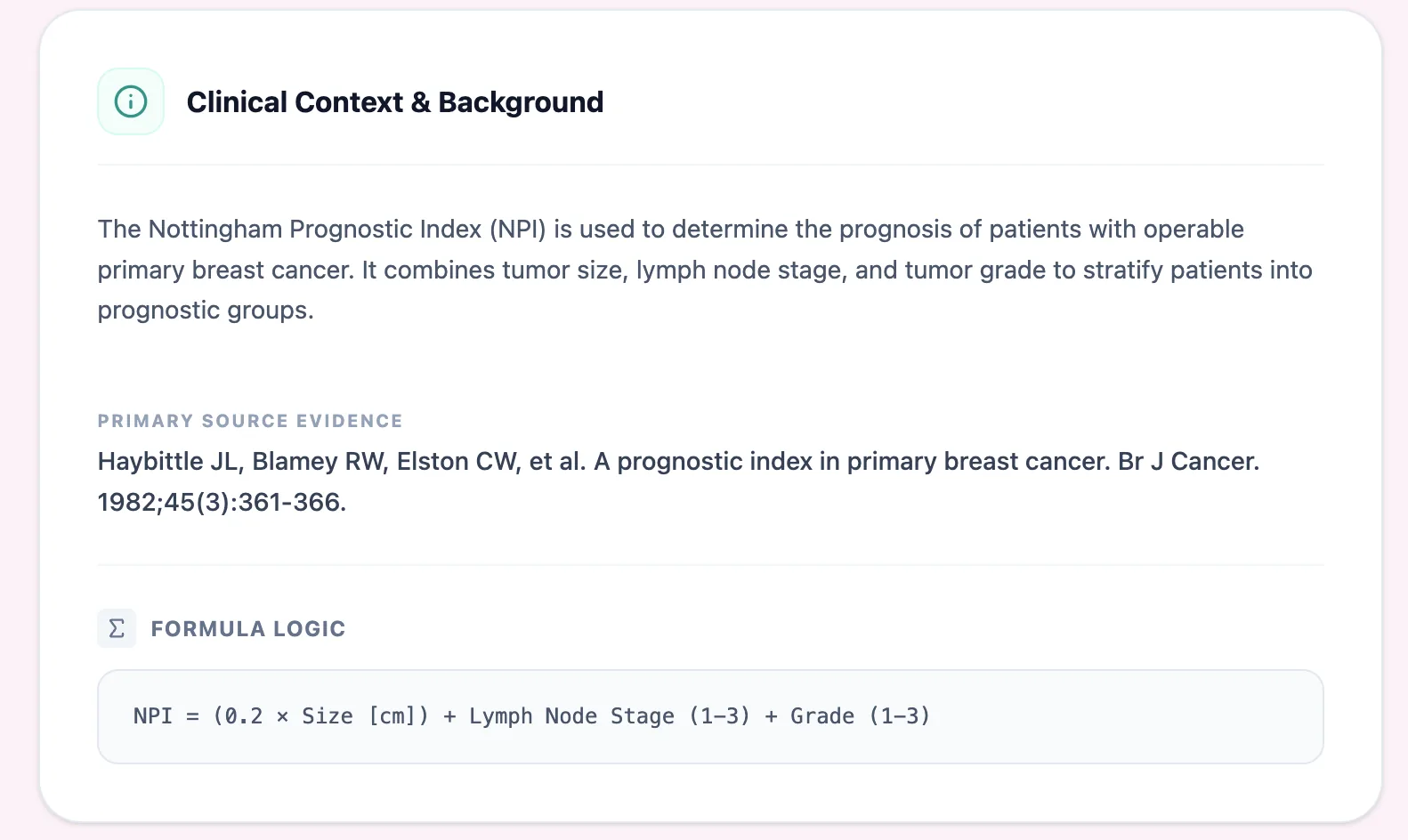
Figure 1. The clinical background panel summarizes the historical development, evidence base, and exact formula used in the NPI.
5. How the OncoToolkit NPI Calculator Works in Detail
5.1 Intuitive data entry tailored to breast surgery workflows
The OncoToolkit NPI calculator mirrors the structure of a typical pathology report and MDT proforma:
- Tumor size is entered as a continuous value in centimetres (e.g., 2.3), with the option to align with invasive size alone or include in situ components according to local practice notes displayed on the page.
- Nodal status is selected from simple, clinically meaningful categories, "0 nodes involved," "1-3 nodes involved," or ">=4 nodes involved," which map internally to nodal stages 1, 2, and 3 for the index.1, 8
- Tumor grade options (Grade I, II, III) map directly onto the numerical scale used in the NPI formula.
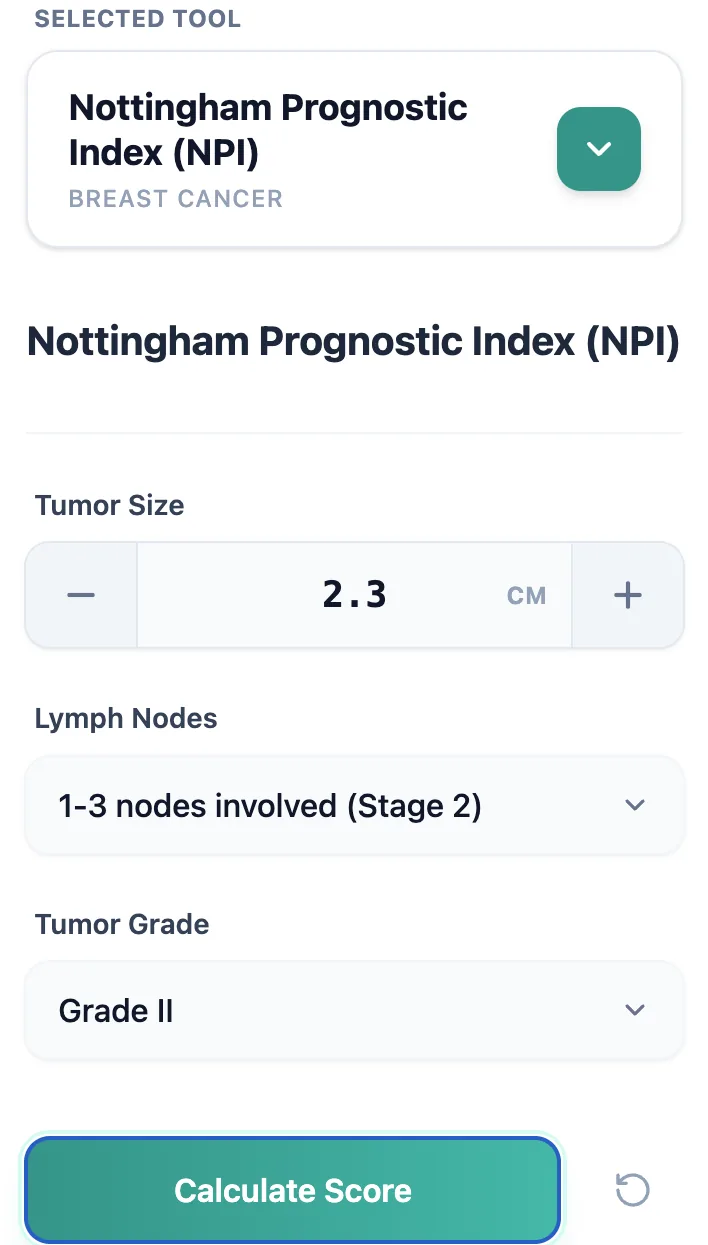
Figure 2. The input view uses numeric fields and dropdown menus that match common pathology report structures.
Hover tips and inline notes remind users about nuances such as excluding pure DCIS, using the largest invasive focus, or aligning nodal category with axillary dissection vs sentinel node biopsy findings. This reduces silent variability and supports consistent data entry across surgeons.
5.2 Transparent calculation and result presentation
After clicking Calculate Score, the tool:
- Multiplies tumor size by 0.2, preserving decimal precision.
- Converts nodal and grade selections into their respective numeric values.
- Sums the components to generate the continuous NPI score.
- Assigns a prognostic group according to the selected schema (3-group or 4-group).
- Displays color-coded risk bands along with 5-year and 10-year survival estimates.
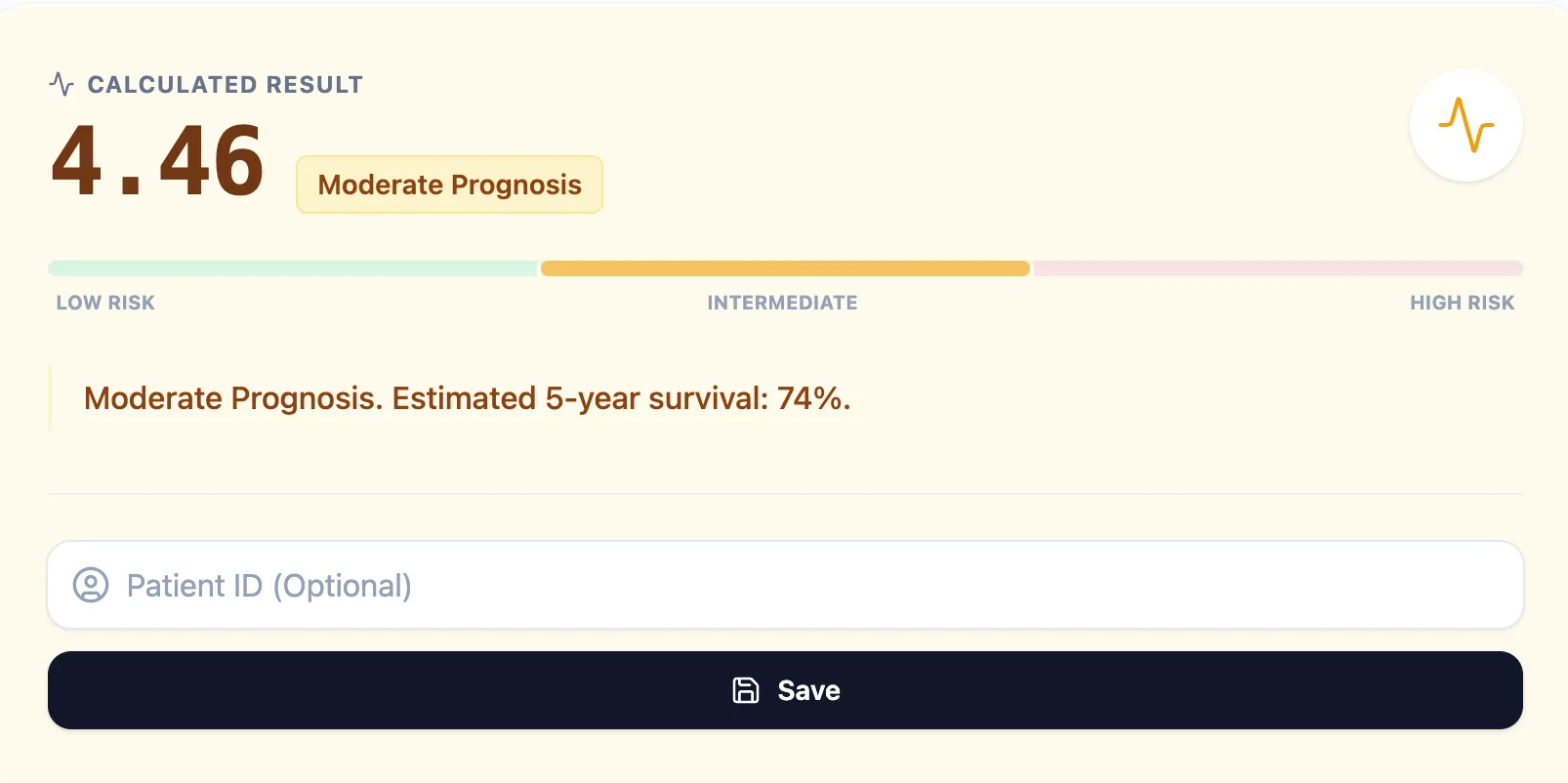
Figure 3. The result screen presents the NPI score, prognostic band, and estimated survival ranges.
The horizontal risk bar spans low, intermediate, and high-risk zones; the specific band corresponding to the patient is highlighted, allowing the MDT to appreciate the patient's position within the full risk spectrum at a glance.
5.3 Advanced workflow features: saving, exporting, and decision prompts
To support real-world practice, the OncoToolkit NPI calculator includes:
- Patient-level saving: Each calculation can be linked to a patient identifier, enabling retrieval during subsequent MDTs.
- Export functionality: Results can be exported as CSV or PDF, or copied into EMR notes for structured documentation.
- Decision-support signals: For high-risk bands, the interface can surface non-directive prompts such as "Discuss adjuvant chemotherapy in MDT."
- Configurable cut-offs: Institutions can elect whether to use 3- or 4-group cut-offs.
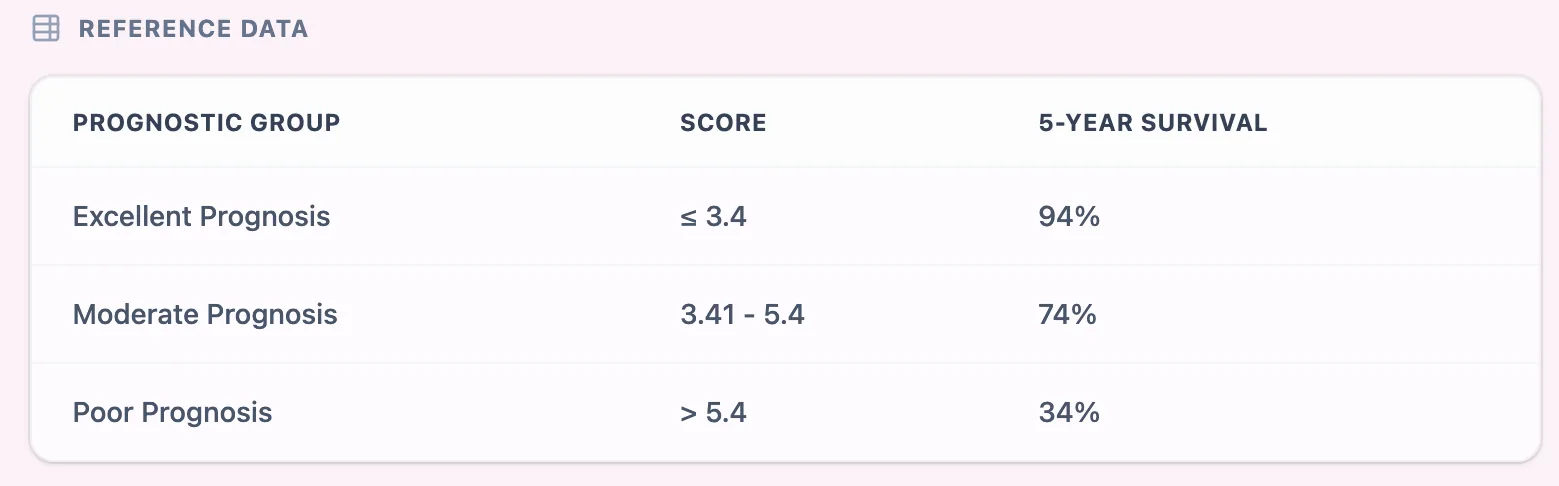
Figure 4. The integrated reference table shows NPI cut-offs and corresponding survival ranges.
6. Integrating NPI With Other OncoToolkit Calculators
Because NPI focuses on tumor size, nodal status, and grade, it interacts naturally with other decision tools:
- A breast TNM staging calculator can be used in parallel, allowing surgeons to present both anatomical stage (e.g., pT2N1M0) and NPI-based risk in MDTs.
- Genomic assay decision tools (Oncotype-like or PAM50-like calculators) can be launched from within the same session, letting users see how genomic risk categories compare with the NPI band for ER-positive, HER2-negative disease.17, 25
- Recurrence risk / CTS5-style calculators extend prognostic assessment into the late period (5-10 years), complementing NPI when discussing extended endocrine therapy.
- Chemotherapy toxicity and comorbidity scores help balance the absolute benefit implied by high NPI against potential treatment risks in older or frailer patients.
Using consistent anchor text such as "breast cancer TNM staging calculator," "adjuvant chemotherapy risk-benefit tool," or "breast cancer recurrence prediction model" allows seamless navigation and internal linking across the platform.
7. How the Platform Supports Clinical Care, Teaching, and Research
7.1 Routine clinical care in high-income and global settings
For high-income centers where genomic assays and advanced imaging are widely available, NPI via OncoToolkit serves as a robust baseline that grounds decision-making in classic pathology. MDTs can use NPI to frame discussions around genomic scores, ensuring that molecular results are interpreted in context rather than in isolation.16, 17
In resource-constrained environments, the same calculator becomes a primary prognostic engine, leveraging universally available histopathology to support equitable care when genomic assays are inaccessible or unaffordable. Because OncoToolkit is browser-based and mobile-responsive, it can be used in tertiary centers, regional hospitals, and outreach clinics alike.28, 18, 26
7.2 Education and trainee development
For residents and fellows, NPI offers a clear introduction to prognostic modeling:
- Supervisors can alter one variable at a time within the calculator to demonstrate how tumor size, nodal status, and grade each contribute to risk.
- The integrated formula and references expose trainees to the logic underpinning prognostic scores, fostering statistical literacy and critical appraisal skills.10, 8
7.3 Clinical research and quality improvement
Standardized, exportable NPI scores support a range of research and QI activities:
- Cohort analyses: Investigators can export NPI data with outcomes to examine local survival curves.3, 2, 11
- Case-mix adjustment: NPI provides a continuous measure for adjusting internal audits according to baseline risk.18, 19
8. Clinical FAQ
Can the Nottingham Prognostic Index be used after neoadjuvant chemotherapy? The original NPI was derived in cohorts undergoing primary surgery without neoadjuvant therapy, and its performance can be distorted when calculated from post-treatment tumor size and nodal status. If used, it should be interpreted with caution.5, 27, 2, 16
How does NPI compare with molecular assays like Oncotype DX or PAM50? NPI is a clinicopathologic index; it captures tumor burden and grade, whereas assays such as Oncotype DX or PAM50 evaluate gene expression and intrinsic subtype. Modern guidelines prioritize genomic signatures, but NPI still provides a low-cost baseline and can highlight discordant cases.14, 12, 25, 16, 17
When should you be cautious about relying on NPI? Caution is warranted in inflammatory breast cancer, de novo metastatic disease, pure in situ lesions, extensive neoadjuvant therapy, and rare histologic subtypes. In these settings, NPI should be complemented by subtype-specific evidence.27, 2, 16
Is NPI validated in non-Western populations? Studies suggest NPI generally retains prognostic discrimination, but absolute survival rates can change with local screening uptake and treatment access. Clinicians should consult regional validation data.13, 26, 28
9. Call to Action and Professional Disclaimer
Ready to Simplify Your NPI Scoring?
Access our clinical-grade calculator to streamline MDT decision-making and patient counseling.
Open NPI Calculator
Free to use. No registration required.
Disclaimer: The Nottingham Prognostic Index calculator on OncoToolkit is intended for use by qualified health professionals as a clinical decision support tool. It is not a substitute for comprehensive clinical assessment. Prognostic estimates are approximate and based on historical cohorts. Final therapeutic decisions must rest with the treating clinical team.
References
- Nottingham Prognostic Index - Wikipedia Source
- The Nottingham Prognostic Index: 35 years on Source
- Validation of the Nottingham Prognostic Index Source
- Breast Cancer Calc NPI Source
- Haybittle et al. (1982) A prognostic index in primary breast cancer Source
- Galea et al. (1992) The Nottingham Prognostic Index Source
- Prognostic factors in primary breast cancer Source
- Validation of NPI in a large series Source
- NPI in screen-detected vs symptomatic populations Source
- Practical pathology for the NPI Source
- NPI validation in UK populations Source
- NPI+ and Biomarkers Source
- NPx: Molecular refinement of NPI Source
- Gene expression classifiers and NPI Source
- NPI in Triple-Negative Breast Cancer Source
- ESMO Guidelines: Early Breast Cancer Source
- NICE Guidance on Genomic Assays Source
- NPI and Surgical Triage Source
- Audit and Service Evaluation using NPI Source
- Statistical power of NPI Source
- Confirmative analysis of NPI Source
- Granular schemas for survival Source
- NPI+ Distant Metastasis Prediction Source
- Risk of Distant Metastases Source
- Gene expression and hormone receptor cohorts Source
- Global validation of NPI Source
- NPI in Neoadjuvant Settings Source
- NPI in Non-Western Populations Source
- Common calculation errors in NPI Source