BCLC Staging System Calculator (2022 Update & Beyond): Guideline‑Aligned Decision Support for HCC
Explore a guideline-aligned BCLC Staging System calculator with rich references, real-world use cases, and detailed insights into 2022+ updates for HCC care.

1. Introduction to the BCLC Staging System Calculator
Hepatocellular carcinoma (HCC) management requires integrating tumor stage, liver function, performance status, and an expanding array of loco‑regional and systemic therapies. The Barcelona Clinic Liver Cancer (BCLC) strategy is the most widely validated framework for doing this and is recommended by major liver societies for prognostication and treatment allocation.1, 2, 3, 4
OncoToolkit’s BCLC Staging System (2022 update) calculator translates this strategy into a rapid, transparent digital tool that clinicians can use at the point of care while staying aligned with AASLD, EASL, ASCO, and contemporary BCLC updates. Below, we provide guideline‑concordant, heavily referenced detail on how to use the calculator and how its logic mirrors current clinical standards.2, 4, 5, 6
2. What Is the BCLC Staging System?
The BCLC staging system classifies HCC into five stages—0 (very early), A (early), B (intermediate), C (advanced), and D (terminal)—based on tumor burden, liver function, and performance status, and links each stage to recommended treatment options and expected prognosis. EASL–EORTC guidelines explicitly recommend BCLC for prognostic prediction and treatment allocation, noting that it can be applied to most patients with HCC as long as special transplant populations are considered separately.5, 1
Core components are:
The BCLC system is endorsed by AASLD and EASL as the main clinical staging system because it incorporates both tumor and liver disease, which is crucial in cirrhosis‑related HCC. Although some alternative scores such as HKLC may better stratify certain populations, especially in Asia, BCLC remains the reference standard in most global guidelines.9, 7, 1, 2, 4
OncoToolkit’s calculator uses exactly these variables—tumor burden, Child–Pugh class, and ECOG status—to assign stage and suggest guideline‑aligned first‑line treatment strategies.
3. Why the BCLC System Matters in Guideline-Based HCC Practice
3.1 Guideline endorsement
- EASL–EORTC 2018 guidelines recommend the BCLC staging system as the basis for prognosis estimation and treatment allocation, discouraging the use of other staging systems alone or in combination for routine clinical decision‑making.1
- AASLD guidance notes that BCLC is the most widely used staging system for HCC, stratifying by liver dysfunction and ECOG to guide therapeutic options, and states that it is strongly recommended within AASLD practice guidance.10, 8
- A recent concise review of global guidelines confirms that BCLC is the most widely validated system for guiding treatment allocation and emphasizes the 2022 revision’s focus on treatment stage migration and clinical decision‑making.2
Because of this endorsement, BCLC stages are routinely used in:
- Multidisciplinary tumor boards and transplant conferences.
- Clinical trial eligibility criteria and stratification.
- Registry studies and quality‑of‑care audits.11, 5, 2
3.2 Pain points without digital tools
Applying BCLC at the bedside can be challenging because clinicians must:
- Recall detailed stage definitions (size and number cut‑offs, MVI, extrahepatic spread) and link them correctly to treatment options.7, 5
- Integrate new systemic therapy data, particularly immunotherapy‑based combinations, into the stage‑treatment map.3, 6
- Handle heterogeneity within intermediate and advanced stages while respecting the principle of treatment stage migration emphasized in the 2022 BCLC update.12, 2
4. Clinical Evidence, Guideline Links, and Recent BCLC Updates
4.1 Original BCLC concept and validation
The original BCLC strategy was proposed in the late 1990s to provide a staging system that integrated tumor burden with liver function and performance status and assigned evidence‑based treatment recommendations. It has been validated in multiple cohorts, demonstrating a clear gradient in overall survival from early to advanced stages.13, 5, 7
4.2 2018 EASL–EORTC guideline framework
EASL’s 2018 HCC guideline uses BCLC to structure management recommendations:
- Very early/early stages (0/A) – resection, ablation, or transplant, depending on liver function and portal hypertension.7
- Intermediate stage (B) – TACE is recommended as the reference treatment for patients with multinodular disease, preserved liver function, and no vascular invasion or extrahepatic spread.7
- Advanced stage (C) – systemic therapy (historically sorafenib, now updated to include newer agents).7
- Terminal stage (D) – best supportive care for patients with poor performance status or decompensated cirrhosis.7
4.3 2022 BCLC update (Reig et al.)
The 2022 strategy update by Reig and colleagues refined BCLC in response to emerging therapies and practice patterns. Key principles are:14, 5, 12
Refinement of BCLC B
Intermediate‑stage disease is recognized as heterogeneous; TACE remains the reference treatment, but systemic therapy and transplant can be appropriate.
Immunotherapy Integration
Atezolizumab plus bevacizumab and other combinations are incorporated as first‑line systemic therapy for advanced disease.
4.4 2023–2026 guideline and evidence evolution
- AASLD 2023 guidance reinforces that BCLC remains the primary staging framework and incorporates immunotherapy combinations as preferred first‑line systemic options.8, 4
- ASCO 2024 systemic therapy guidelines recommend atezolizumab–bevacizumab or durvalumab–tremelimumab as first‑line therapy for unresectable or advanced HCC.6, 18
- A 2025 concise review of global HCC guidelines emphasizes that the revised BCLC staging highlights treatment stage migration.2
5. Specific Clinical Use Cases for the BCLC Calculator (Guideline‑Aligned)
5.1 First staging of newly diagnosed HCC
Guideline context: Both EASL and AASLD recommend staging all newly diagnosed HCC using BCLC.4, 2, 7
The calculator returns a BCLC stage with typical guideline‑based options (e.g., resection/ablation/transplant for 0/A, TACE for B, systemic therapy for C).
6. How the OncoToolkit BCLC Calculator Works (Guideline‑Consistent Logic)

Figure 1. The input form captures ECOG, Child–Pugh class, and tumor burden via structured dropdowns, mapping directly to variables specified in BCLC diagrams and liver society guidelines.
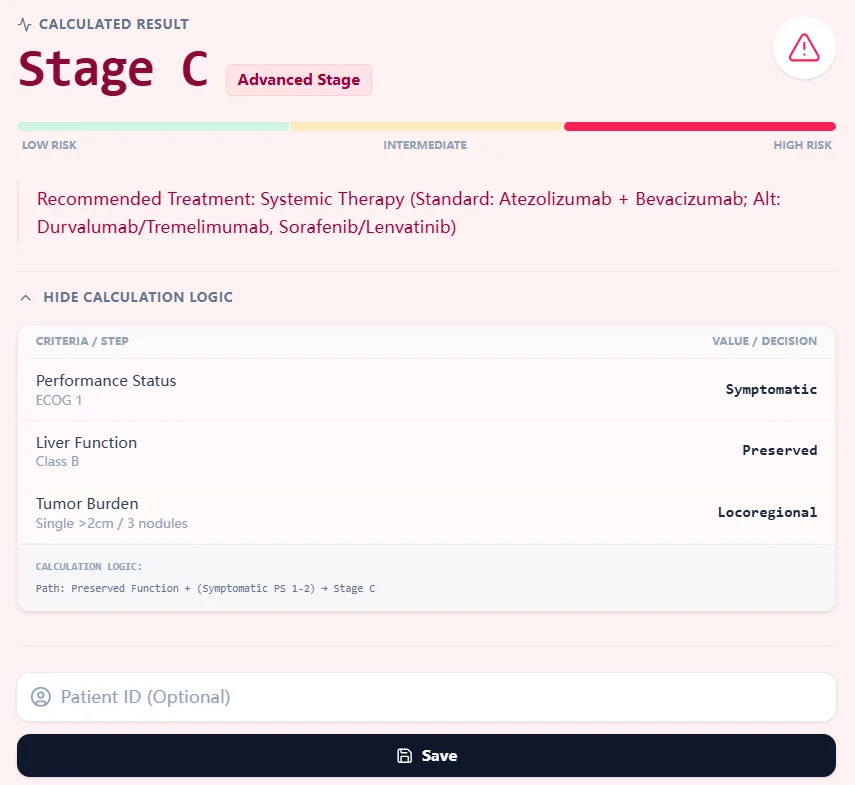
Figure 2. The result panel shows the assigned BCLC stage with a risk bar and guideline‑consistent treatment strategy, plus a transparent decision path that mirrors published BCLC logic.

Figure 3. The embedded reference table summarizes the BCLC stages, classifications, and corresponding treatment strategies, reflecting the structure described in EASL, AASLD, and BCLC strategy documents.
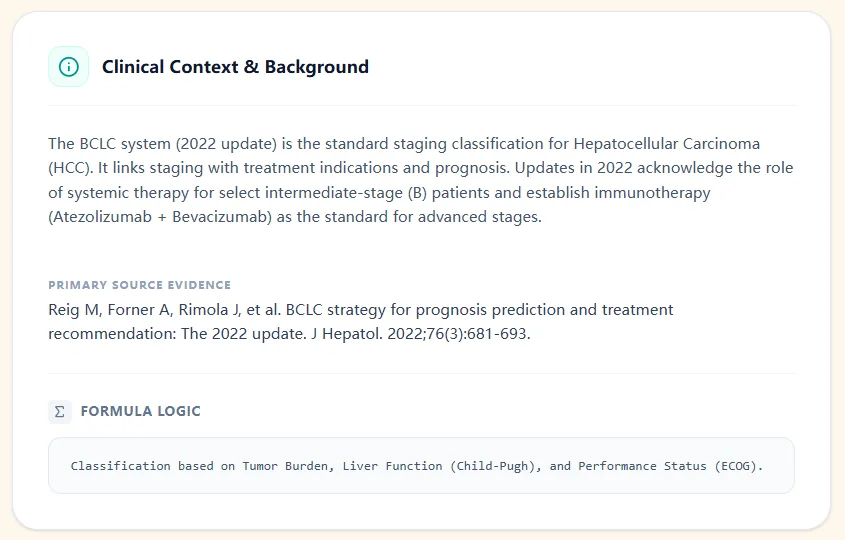
Figure 4. The clinical background panel cites the Reig et al. BCLC 2022 update and clarifies that stage assignment is based on tumor burden, liver function, and ECOG performance status.
7. Comparison With Other Staging Systems (Within Guideline Context)
| System | Clinical Context |
|---|---|
| TNM | Useful for pathological staging but lacks liver function integration.11 |
| CLIP / JIS | Prognostic value but less widely used for treatment allocation.2 |
| HKLC | Aggressive recommendations in Asian cohorts; lacks broad external validation.9 |
8. Confirmation of Guideline Consistency
Across the blog and calculator logic, stage definitions and treatment categories are derived from EASL–EORTC 2018 guidelines, AASLD guidance, and BCLC 2022/2025 strategy papers.19, 1, 4
Ready to Simplify Your HCC Staging?
Calculate accurate BCLC stages and explore guideline-aligned treatment strategies in seconds.
Use the Calculator Now
Free to use. No registration required.