ELTS Score (CML) Calculator: Risk Stratification for Chronic Myeloid Leukemia in the TKI Era
Calculate the ELTS Score for chronic myeloid leukemia in seconds. Predict CML-specific survival, guide TKI selection, and streamline MDT decisions — free online calculator.

Quick Navigation
- 1. What Is the ELTS Score?
- 2. Why the ELTS Score Matters in Daily Practice
- 3. Clinical Evidence and Validation for the ELTS Score
- 4. From ELTS at Diagnosis to Molecular Milestones on Treatment
- 5. How Our ELTS Score (CML) Calculator Works
- 6. Supporting Clinical Care and Research
- 7. Frequently Asked Questions (FAQ)
- 8. Start Risk-Stratifying Your CML Patients Today
Chronic myeloid leukemia is one of modern oncology's great success stories. Tyrosine kinase inhibitors have transformed a once-fatal diagnosis into a manageable chronic condition with 10-year overall survival rates exceeding 80%. Yet this progress creates a new clinical challenge: when most patients will not die of their leukemia, how do you identify the minority who will? The ELTS Score (CML) — the EUTOS Long-Term Survival score — was designed precisely for this question. It is the only prognostic tool developed and validated specifically to predict CML-related death in the era of TKI therapy, and the 2025 European LeukemiaNet (ELN) recommendations endorse it as the preferred baseline risk-stratification score.1, 2, 3, 4
At OncoToolkit, we have built a fast, mobile-responsive ELTS Score (CML) calculator so you can risk-stratify a new CML patient in seconds — whether you are in the clinic, at a multidisciplinary team (MDT) meeting, or supervising a trainee on the ward.
1. What Is the ELTS Score?
The ELTS score is a continuous prognostic index for adult patients newly diagnosed with Philadelphia chromosome-positive chronic-phase CML. It was developed by Pfirrmann and colleagues and published in Leukemia in 2016, using data from 2,205 imatinib-treated patients enrolled in the European Treatment and Outcome Study (EUTOS) registry, and independently validated in a separate cohort of 1,120 patients.5, 4
Unlike its predecessors — the Sokal score (1984), the Hasford/Euro score (1998), and the original EUTOS score (2011) — the ELTS score was built using a Fine-Gray competing-risks regression model rather than a standard Cox proportional-hazards approach. This matters because, in an era where over half of patient deaths are unrelated to CML (second cancers, cardiovascular events, infections), a model that accounts for competing risks provides a sharper lens on the probability of dying specifically from leukemia.4, 5
The score incorporates four variables, all measured at diagnosis before any CML therapy:
- Age (completed years)
- Spleen size (cm below the costal margin on palpation)
- Peripheral blood blasts (%, rounded to integer)
- Platelet count (×10⁹/L)
The result maps each patient to one of three risk groups — Low, Intermediate, or High — that carry distinct probabilities of CML-specific death.6, 5
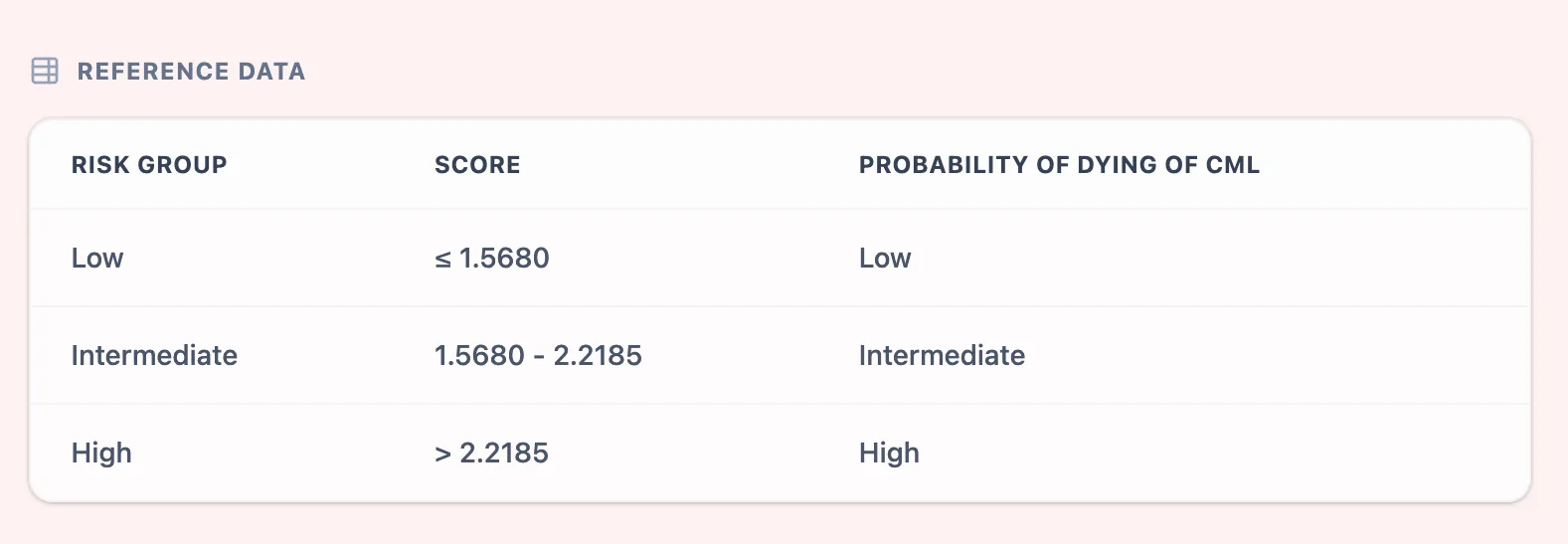
Figure 1. Reference table integrated into the OncoToolkit ELTS calculator. Patients with a score ≤ 1.5680 fall into the low-risk group, those between 1.5680 and 2.2185 into the intermediate-risk group, and those above 2.2185 into the high-risk group. These cutoffs directly inform first-line TKI selection and monitoring intensity.
2. Why the ELTS Score Matters in Daily Practice
It replaces outdated scoring systems at the bedside
The Sokal score remains familiar to many clinicians, but it was developed in the chemotherapy era and optimized for overall survival — not for CML-specific death in TKI-treated patients. A landmark comparison of 5,154 patients demonstrated that the Sokal score classifies roughly 23% of patients as high-risk, whereas the ELTS score classifies only about 12%. Crucially, 56% of Sokal high-risk patients are reclassified as non-high-risk by the ELTS score — and these patients have a significantly more favorable long-term prognosis. Overestimating risk can lead to unnecessary escalation to second-generation TKIs with their attendant cardiovascular and metabolic toxicities.7, 8, 9
It directly influences first-line TKI choice
The 2025 ELN recommendations list a high ELTS score at baseline as a "warning" signal, one that may favor upfront use of a more potent second-generation TKI (e.g., dasatinib, nilotinib, bosutinib) or the newer STAMP inhibitor asciminib. Conversely, a low ELTS score supports first-line imatinib — the safest, most cost-effective option — with confidence that long-term CML-related mortality will be very low.3, 1
It reduces calculator fatigue in busy clinics
Clinicians managing hematologic malignancies already juggle multiple scoring systems across diseases. Having a single, guideline-endorsed score that replaces three legacy tools (Sokal, Hasford, EUTOS) for CML baseline risk assessment meaningfully reduces the cognitive burden of routine care. On our platform, the ELTS calculator is optimized for point-of-care and MDT use — it works on any mobile device, returns a result in one tap, and displays both the numerical score and the risk-group classification with a clear visual indicator.10, 11
3. Clinical Evidence and Validation for the ELTS Score
The Math Behind the Tool
The ELTS score formula is:
ELTS = 0.0025 x (Age / 10)^3 + 0.0615 x Spleen + 0.1052 x Blasts + 0.4104 x (Platelet / 1000)^-0.5
Each coefficient was derived from the Fine-Gray model, weighting the independent contribution of each variable to CML-specific death while treating non-CML death as a competing event. Notice that platelet count enters as an inverse square-root transformation — very low platelet counts drive the score upward more steeply than high counts, reflecting the known adverse prognostic impact of thrombocytopenia in CML. Age enters as a cubic function of decades, capturing the accelerating risk associated with advanced age.5, 6
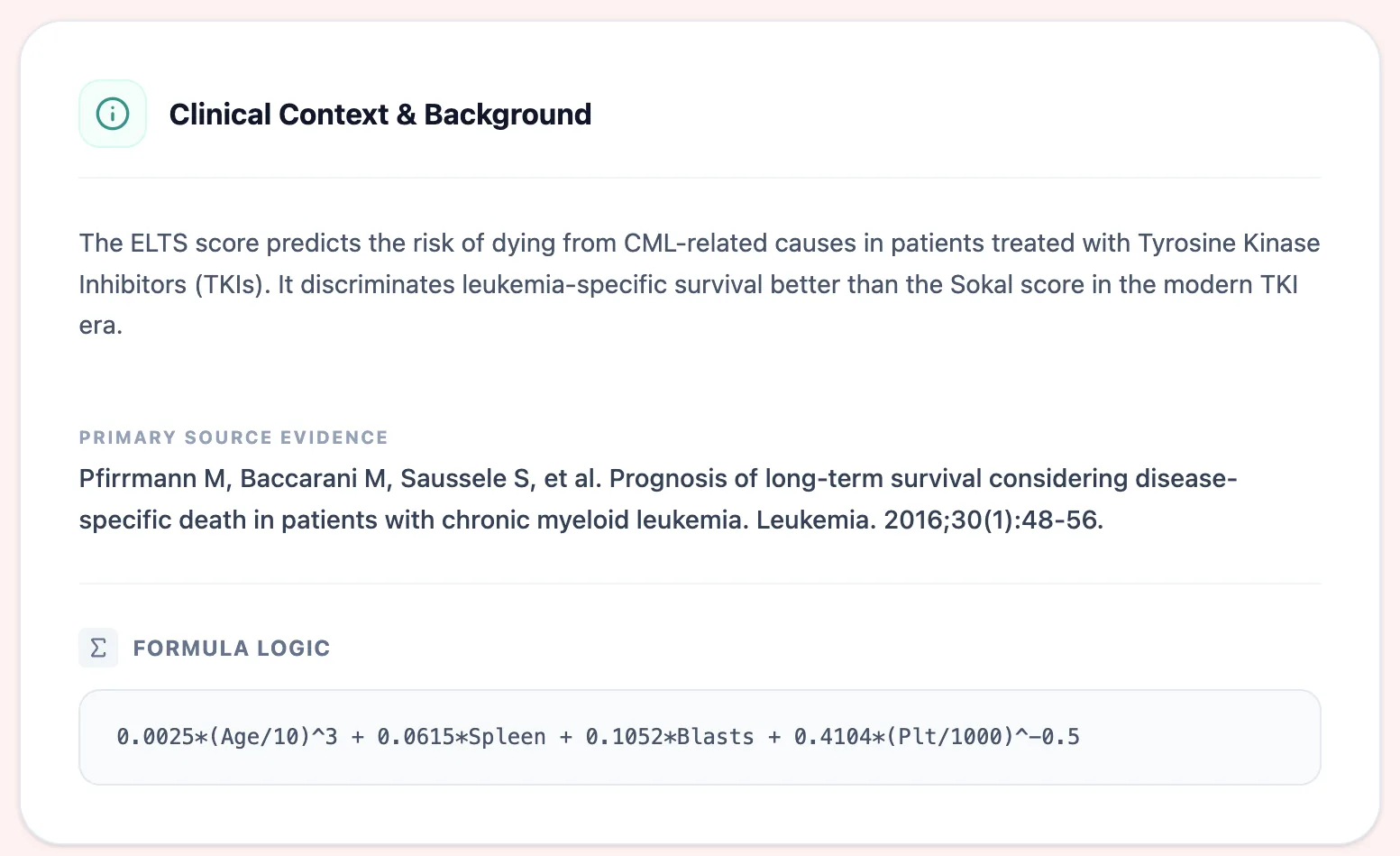
Figure 2. OncoToolkit displays the underlying formula and primary source citation (Pfirrmann et al., Leukemia 2016) directly within the calculator interface, supporting transparency and trust for technical users who want to verify the math.
Key Validation Data
Original development and validation (Pfirrmann 2016): In the development cohort of 2,205 patients, the 8-year overall survival probability was approximately 89%, and the 8-year cumulative incidence of CML-related death was roughly 4%. The score separated the three risk groups with statistical and clinical significance in both the development and independent validation sets.12, 4, 5
Large-scale comparative analysis (Pfirrmann 2020): Across 2,949 patients not involved in score development, the ELTS score achieved higher hazard ratios and concordance indices than the Sokal, Euro, or EUTOS scores in every head-to-head comparison for long-term survival discrimination.9, 7
Japanese real-world cohort (Sato 2020, n = 342): The ELTS score was the most sensitive tool for predicting CML-specific death, event-free survival, progression-free survival, and overall survival — outperforming Sokal, Hasford, and EUTOS. Five-year CML-related death rates were 0.9% (low), 5.4% (intermediate), and 32.6% (high). Notably, the ELTS score was the only scoring system that predicted deep molecular response (DMR) at any time point (65.0%, 43.7%, and 23.5% in low-, intermediate-, and high-risk groups respectively; p = 0.0000569). This finding directly links baseline ELTS risk to the likelihood of achieving treatment-free remission (TFR) downstream.13
Chinese multicenter validation (Yang 2020, n = 479): In a real-world Chinese CML-CP cohort treated with frontline imatinib, the 5-year CML-related death rates were 2% (low), 5% (intermediate), and 11% (high). This cohort presented with greater disease burden at diagnosis (median spleen 8 cm, 62.8% splenomegaly), yet the ELTS score still outperformed all prior scoring systems for CML-related death — a finding the Sokal, Hasford, and EUTOS scores all failed to achieve with statistical significance.14
Additional Asian and Middle Eastern data: Validation studies from Thailand, Bangladesh, and Saudi Arabia have corroborated the ELTS score's prognostic utility in diverse ethnic populations, supporting its use as a globally applicable tool.15, 16, 17
Limitations a Thoughtful Clinician Should Know
- •Diagnosis-only application. The ELTS score was developed and validated exclusively using variables measured at diagnosis, before any CML therapy. Once a TKI is started, blood counts change rapidly. Recalculating the score after treatment initiation is invalid. Post-TKI risk assessment shifts entirely to molecular monitoring of BCR::ABL1 transcript levels.5
- •Imatinib-centric derivation. The original cohort was treated exclusively with imatinib. However, subsequent studies have shown that the ELTS score retains predictive power in patients receiving second-generation TKIs as first-line therapy.18, 13
- •Does not account for genomic features. Somatic mutations such as ASXL1, additional chromosomal abnormalities (ACAs), or BCR::ABL1 transcript type are not captured by the ELTS formula. The 2025 ELN guidelines recommend considering high-risk ACAs alongside the ELTS score for a more complete baseline risk profile.1
4. From ELTS at Diagnosis to Molecular Milestones on Treatment
One of the most important concepts for trainees to grasp is that the ELTS score is the starting line, not the whole race. It tells you where a patient begins; molecular monitoring tells you how they are responding.
Once a TKI is initiated, the 2025 ELN guidelines define response milestones at 3, 6, and 12 months based on BCR::ABL1 transcript levels on the International Scale (IS):19, 1
| Timepoint | Favorable (No Switch) | Warning (May Switch) | Unfavorable (Prefer Switch) |
|---|---|---|---|
| Baseline | — | High ELTS, high-risk ACA | — |
| 3 months | BCR::ABL1^IS ≤ 10% | > 10% | > 10% (confirmed) |
| 6 months | ≤ 1% | > 1–10% | > 10% |
| 12 months | ≤ 0.1% (MMR) | > 0.1–1% | > 1% |
A patient with a high ELTS score who achieves favorable milestones at 3 and 6 months may ultimately do well. Conversely, a low-ELTS patient who fails to reach BCR::ABL1^IS ≤ 10% at 3 months warrants closer scrutiny and potential TKI switch. This two-stage risk framework — ELTS at the gate, molecular milestones along the track — is the backbone of modern CML management.1
For patients who achieve durable deep molecular response (MR⁴ or deeper for ≥ 2–3 years), treatment-free remission (TFR) may be attempted, with approximately 40–50% sustaining remission long-term. The ELTS score indirectly predicts TFR candidacy: low-risk patients are significantly more likely to achieve DMR and therefore more likely to qualify for TKI discontinuation.13, 3, 19
5. How Our ELTS Score (CML) Calculator Works
At OncoToolkit, we've designed the ELTS Score (CML) calculator to mirror the clinician's workflow — minimizing clicks and maximizing clarity.
Step 1: Enter Four Values
Open the calculator at oncotoolkit.com/calculator/lymphoma-elts-score. You will see four input fields, each with increment/decrement buttons for quick adjustment:
- Age (years) — completed years at diagnosis.
- Spleen Size (cm below costal margin) — palpated spleen below the costal margin; enter 0 if not palpable.
- Peripheral Blood Blasts (%) — rounded to the nearest whole number.
- Platelet Count (×10⁹/L) — as reported on the full blood count.
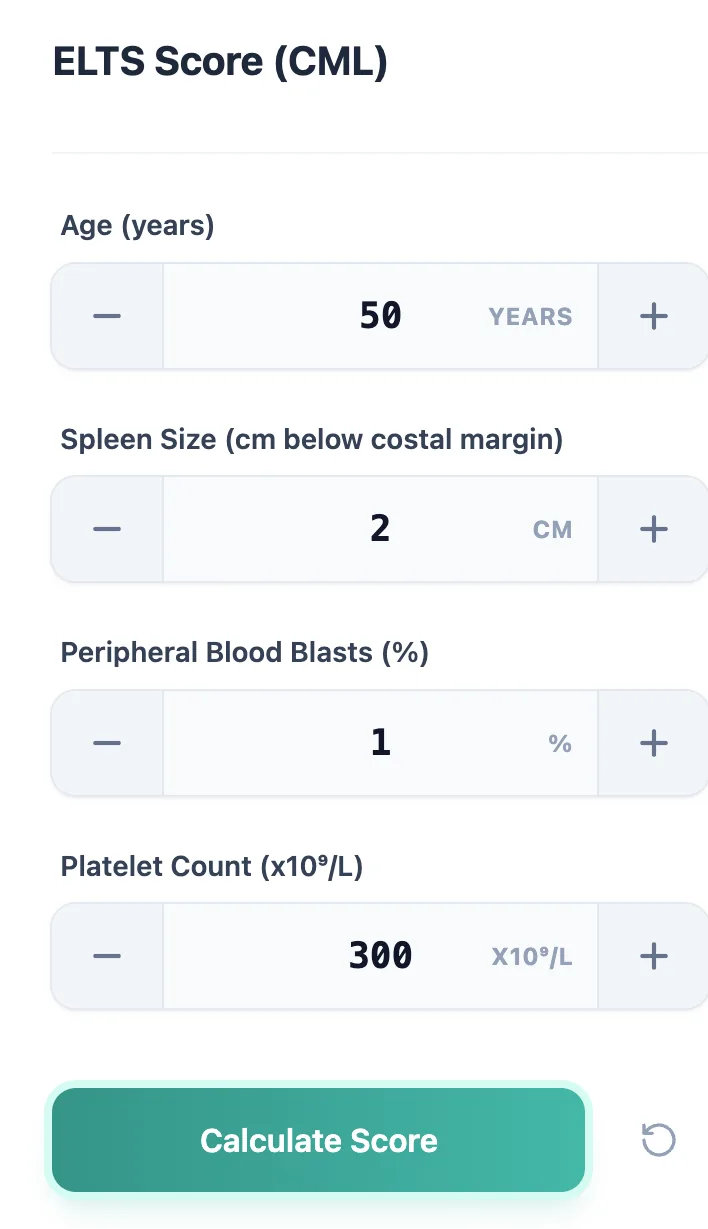
Figure 3. The input interface is optimized for one-handed mobile use — ideal for rounds, clinic, or MDT prep. Stepper controls allow rapid value adjustment without a keyboard, and units are clearly labeled to prevent data-entry errors.
Step 2: Tap "Calculate Score"
A single tap computes the ELTS score using the exact Pfirrmann formula and maps it to the corresponding risk group. The entire calculation takes under one second.
Step 3: Review the Result
The result screen displays:
- ✓ The numerical ELTS score
- ✓ A risk-group label with a badge
- ✓ A visual risk spectrum bar
- ✓ Plain-language interpretation

Figure 4. A sample result for a 50-year-old patient with a 2 cm spleen, 1% peripheral blasts, and a platelet count of 300 × 10⁹/L yields an ELTS score of 1.29 — low risk. The color gradient provides instant visual context for clinical interpretation.
6. Supporting Clinical Care and Research
Routine Clinical Decision Support
The most immediate use case is risk stratification at the point of new CML-CP diagnosis. Calculating the ELTS score should be a reflexive step — analogous to ordering a baseline BCR::ABL1 transcript level. It informs the choice of first-line TKI, the intensity of initial monitoring, and the conversation about long-term prognosis with the patient.
Education and Training
For fellows and residents, the calculator functions as a teaching aid. Walking through a series of example cases — varying age, spleen size, blasts, and platelets — builds intuition for which variables move the score most dramatically and why. The transparent formula display turns the calculator into an interactive learning module.
Clinical Research and Quality Improvement
Consistent use of the ELTS score across a department's CML cohort enables:
- Standardized staging for retrospective analyses. Cohort characterization becomes straightforward.
- Benchmarking against published data. Audit outcomes against validated cohorts to identify systemic gaps.
- Integration with survival analytics. Pair patient data with Kaplan-Meier dashboards to track practice-wide trends.
7. Frequently Asked Questions (FAQ)
Can the ELTS score be used in patients with accelerated-phase or blast-phase CML?
No. The ELTS score was developed and validated exclusively for chronic-phase CML diagnosed before any TKI therapy. Patients presenting in accelerated or blast phase have fundamentally different biology; the ELTS formula does not account for their elevated blast counts or cytogenetic complexity.3, 1, 5
How does the ELTS score differ from the Sokal score?
| Dimension | Sokal Score | ELTS Score |
|---|---|---|
| Year | 1984 | 2016 |
| Era | Chemotherapy | TKI |
| Endpoint | Overall survival | CML-specific death |
| ELN 2025 | Superseded | Preferred |
8. Start Risk-Stratifying Your CML Patients Today
The ELTS score is the current gold standard for baseline risk assessment in chronic-phase CML — endorsed by the 2025 ELN, validated globally, and designed for the treatment era your patients actually live in.
1. Bookmark the calculator and add it to your diagnostic workflow.
2. Run practice cases to build intuition for variable weighting.
3. Present the ELTS risk group at MDTs for structured discussion.
Calculators on OncoToolkit are clinical decision-support tools and do not replace individualized clinical judgment. Always interpret results in the context of the whole patient.
Ready to Simplify Your CML Risk Stratification?
Calculate the ELTS Score in seconds to guide treatment and monitor milestones with confidence.
Open ELTS (CML) Calculator
Free to use. No registration required.
References
- 2025 European LeukemiaNet recommendations for the management of chronic myeloid leukemia. [1]
- JF Apperley et al. 2025 European LeukemiaNet recommendations for the... Leukemia (2025). [2]
- H Kantarjian. Management of Chronic Myeloid Leukemia in 2025. [3]
- New CML Risk Score Incorporates Modern Survival Probability. Cancer Network. [4]
- The EUTOS long-term survival (ELTS) score. ELN. [5]
- ELTS - The EUTOS long-term survival score online calculator. Clincasequest. [6]
- M Pfirrmann et al. The EUTOS long-term survival (ELTS) score is superior to the Sokal score... Leukemia (2020). [7]
- Markus Pfirrmann. THE EUTOS LONG-TERM SURVIVAL (ELTS) SCORE IS SUPERIOR TO THE SOKAL... EHA (2018). [8]
- The EUTOS long-term survival (ELTS) score is superior to the Sokal score for predicting survival. University of Liverpool. [9]
- Supporting clinical decisions with health information technology. NHS England. [10]
- L Samal et al. Refining Clinical Phenotypes to Improve Clinical Decision Support (2023). [11]
- M Pfirrmann et al. Prognosis of long-term survival considering disease-specific death... Leukemia (2016). [12]
- E Sato et al. The EUTOS long-term survival score predicts disease progression in CML. BMC Cancer (2020). [13]
- X Yang et al. Validation of the EUTOS Long-Term Survival Score in Chinese CML Patients (2020). [14]
- Comparison of ELTS Score with Sokal, Euro and EUTOS in CML. PubMed. [15]
- Tyrosine kinase inhibitor (TKI) is the standard treatment for chronic myeloid leukemia (CML). [16]
- Consistency Test between Scoring Systems for Predicting Prognosis in CML. Wiley. [17]
- Sokal, Hasford, and EUTOS scores. [18]
- T Sacha. Advances in diagnosis and treatment of chronic myeloid leukemia. Acta Haematologica Polonica (2025). [19]
- The Sokal, Hasford, EUTOS and ELTS Scores. Clincasequest. [20]